- A stress echocardiogram combines a standard echocardiogram with exercise, capturing ultrasound images of the heart at rest and immediately after peak exertion to assess how the heart responds to increased demand.
- It is primarily used to detect coronary artery disease, identifying areas of the heart muscle that receive reduced blood flow during exercise, suggesting a significant narrowing in one or more coronary arteries.
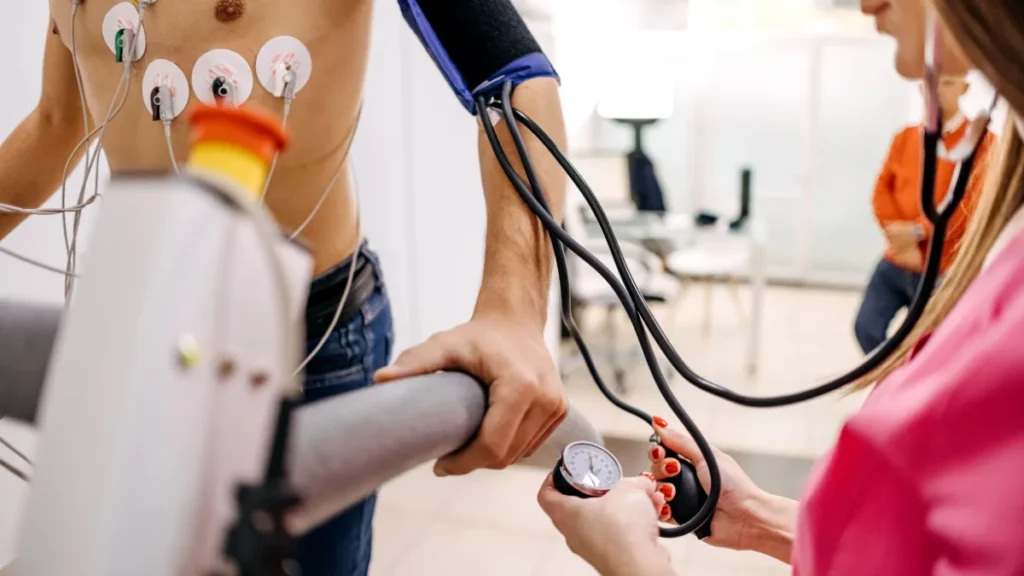
- The test involves exercising on a treadmill or exercise bike while your heart rate, blood pressure, and ECG are continuously monitored.
- Some medications, particularly beta-blockers and calcium channel blockers, may need to be withheld beforehand. Your team will advise specifically.
- No radiation is involved. The test is safe and well-tolerated in appropriate patients, with trained staff and emergency equipment present throughout.
Being referred for a stress echocardiogram can sound more daunting than it is. The name suggests something technically complex, and it is, in the sense that it combines two investigations simultaneously, but from the patient’s perspective, it is simply a matter of exercising on a treadmill while the clinical team monitors your heart, then lying down quickly for an ultrasound scan.
Understanding what the test is looking for, how to prepare, and what the results mean helps make the whole experience considerably less uncertain.
What Is a Stress Echocardiogram?
The two tests combined
A stress echocardiogram, or stress echo, combines two investigations that are highly informative individually but even more so together. The first is an echocardiogram: an ultrasound of the heart that shows how the chambers are moving and how well the muscle is contracting. The second is an exercise stress test: monitored physical exertion designed to push the heart rate and demand on the coronary arteries.
By comparing ultrasound images of the heart at rest with images taken immediately after peak exercise, the cardiologist can see whether all areas of the heart muscle contract equally well under load, or whether some regions fall behind, suggesting they are not receiving adequate blood supply during exertion.
What it is looking for
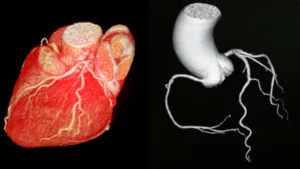
The stress echo does not directly visualise the coronary arteries, that is the role of a CT coronary angiogram or invasive angiogram. What it does is assess the functional consequence of any narrowings that may be present.
A coronary artery narrowing of 60–70% or more typically restricts blood flow significantly during exercise, even if blood supply appears adequate at rest. When a region of heart muscle receives less blood during exertion, it contracts less vigorously, a change visible on the post-exercise echo images. This is what the cardiologist is looking for.
I often explain to patients that the stress echo is like asking the heart to reveal what it can manage under pressure. A resting echo tells you about the heart at idle. The stress echo tells you what happens when you ask it to work, and that’s often where the important information lives.
Why Has It Been Requested?
Your cardiologist or doctor may have recommended a stress echo for any of several reasons. The most common is investigation of chest tightness, breathlessness, or other symptoms that occur with exertion and could suggest coronary artery disease.
It is also used to assess the significance of a known coronary narrowing, whether it is causing functional ischaemia or not, and to evaluate heart function and valve behaviour under exercise conditions. After a heart attack or cardiac procedure, it can help assess the heart’s recovery and exercise capacity.
What to Expect
What to Expect, Stress Echocardiogram
Duration
Approximately 60 minutes in total, preparation, rest images, exercise, and recovery imaging.
Preparation
Fast for 3–4 hours beforehand. Avoid caffeine on the day. Some medications, particularly beta-blockers and calcium channel blockers, may need to be withheld. Follow your clinic’s specific instructions. Wear comfortable clothing and walking shoes.
Comfort
The resting echo and exercise phases are straightforward. The exercise is deliberately progressive, you are encouraged to reach your maximum tolerated level. You can stop at any time if symptoms develop.
Radiation / Contrast
No radiation. Ultrasound only. Occasionally an ultrasound contrast agent (not iodine) is used to improve image quality, your team will advise if this applies.
Results
The cardiologist reviews both rest and stress images together. A formal report is typically available within a few days and discussed with you at follow-up.
Afterwards
No restrictions. Resume normal activities the same day. If you withheld medications for the test, confirm with your team when to restart them.
Preparing for the Test
Medications that may need to be withheld
The stress echo works by pushing the heart rate to a target level during exercise. Certain medications that slow the heart rate, particularly beta-blockers and rate-limiting calcium channel blockers such as diltiazem and verapamil, can prevent the heart rate from reaching the level needed for a meaningful test. Your team will advise whether to withhold these on the day.
Do not stop any cardiac medication without specific instructions from your referring team. If you are unsure, call the clinic before the test rather than making your own decision.
On the day
Avoid caffeine on the day of the test, coffee, tea, and energy drinks all affect heart rate. Fast for approximately three to four hours beforehand. Wear comfortable clothing and supportive walking or running shoes. You will have ECG electrodes placed on your chest, so a loose-fitting top that can be easily adjusted is helpful.
During the Test, Step by Step
Resting images first
You will lie on your left side while the sonographer takes baseline ultrasound images of your heart at rest. ECG leads are placed on your chest and a blood pressure cuff on your arm. These resting images are the reference point against which the post-exercise images will be compared.
Exercise phase
You then exercise on a treadmill or stationary bike, with speed and incline increasing in stages according to a standard protocol. Your heart rate, blood pressure, and ECG are monitored continuously throughout. The aim is to reach your target heart rate, typically around 85% of the maximum predicted for your age, or to exercise to the point of symptoms.
You can stop at any time if you experience chest tightness, significant breathlessness, or feel unwell. The clinical team will also stop the test if the ECG or blood pressure shows a concerning change. Stopping the test is not a failure, it provides important clinical information regardless of when it occurs.
Post-exercise imaging
Immediately after peak exercise, within 60 to 90 seconds, you lie back down and the sonographer takes the post-exercise echo images while the heart rate is still elevated. This timing window is critical: the images need to be captured before the heart rate returns to normal. The speed and smoothness of this transition is something the clinical team practise carefully.
Safety
The stress echocardiogram is a safe test in appropriately selected patients. Serious complications, such as a significant arrhythmia or cardiac event, are uncommon and are managed immediately by the trained clinical team, who have resuscitation equipment available throughout. The test is not performed if there are clinical reasons that would make it unsafe for a particular patient, this assessment is made before the test is arranged.
Temporary symptoms during exercise, mild chest tightness, breathlessness at peak effort, or a brief period of dizziness, are expected and normal. They typically resolve within minutes of stopping exercise.
When Exercise Is Not Possible, Pharmacological Stress Echo
For patients who are unable to exercise adequately, due to orthopaedic problems, severe deconditioning, or other limitations, a pharmacological stress echo can be performed instead. A medication such as dobutamine is infused intravenously to mimic the effect of exercise on the heart, increasing heart rate and myocardial demand without the patient needing to exercise. The echo imaging proceeds in the same way. This option makes the stress echo accessible to patients who could not otherwise have a meaningful exercise test.
Understanding the Results
A normal result
A normal stress echo means that all areas of the heart muscle contract equally well at peak exercise as they do at rest, no regional wall motion abnormalities are identified. This is a genuinely reassuring result. It makes significant flow-limiting coronary artery disease unlikely as the cause of the patient’s symptoms.
An abnormal result
An abnormal result, a region of heart muscle that contracts well at rest but less well or not at all at peak exercise, suggests that area is receiving reduced blood flow during exertion, consistent with a significant coronary narrowing. This finding typically leads to further investigation, most commonly a CT coronary angiogram or invasive coronary angiogram, to identify the location and severity of the narrowing.
Limitations to be aware of
Like all investigations, the stress echo is not perfect. In some patients, particularly those with poor acoustic windows from body habitus, lung disease, or prior cardiac surgery, ultrasound image quality may limit the information available. The test is also better at detecting significant narrowings than mild ones. Your cardiologist will interpret the result alongside your clinical history and other investigations rather than in isolation.
- Should I withhold any of my regular medications before the test, and when should I restart them?
- What heart rate am I aiming to reach, and what happens if I cannot reach it?
- If I cannot exercise adequately, is a pharmacological stress echo an option?
- What would an abnormal result mean for my management?
- Is a CT coronary angiogram an alternative that might give more direct anatomical information?
Heart Matters Resource
When in Doubt, Get Checked Out
Chest tightness, breathlessness on exertion, or symptoms that only appear with exercise deserve proper cardiac assessment. A stress echo is often one of the most informative first steps.
Conclusion
The stress echocardiogram is one of the most informative non-invasive cardiac investigations available, combining the structural detail of echocardiography with the functional challenge of exercise to reveal how the heart performs under real demand.
A normal result provides meaningful reassurance. An abnormal result gives specific, actionable information that directly guides the next step. Either way, the test moves the clinical picture forward, and that is always the goal.
Prepare carefully, communicate your symptoms clearly to the team during the test, and attend your follow-up appointment ready to discuss what the result means for your management.