- High blood pressure is one of the leading modifiable cardiovascular risk factors, and it produces no symptoms in the vast majority of cases.
- Regular monitoring is the only reliable way to detect it. A normal blood pressure is below 120/80 mmHg.
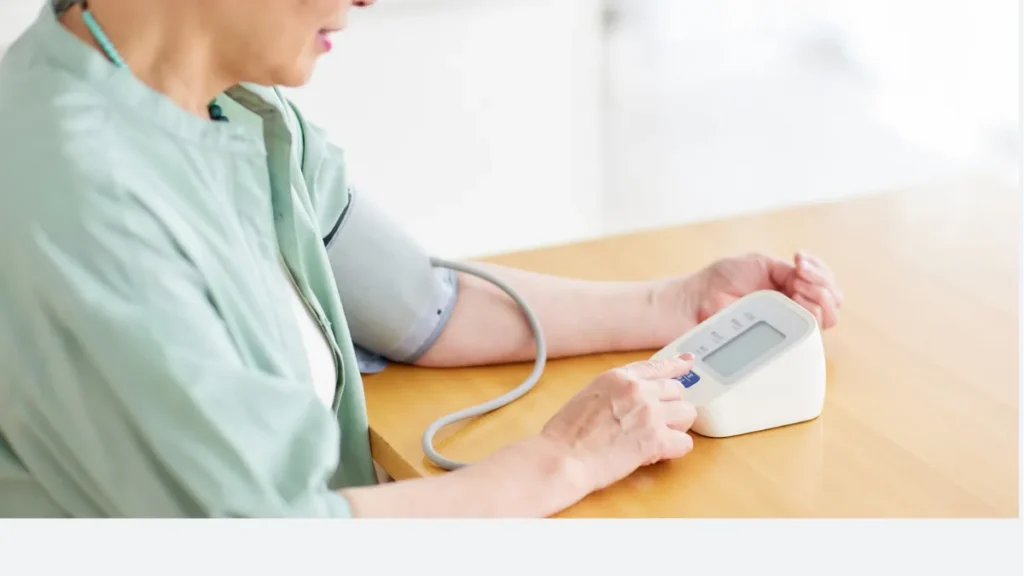
- Home blood pressure monitoring gives a far more accurate picture of your true blood pressure than occasional clinic readings alone, and eliminates the distorting effect of white coat hypertension.
- Our free Blood Pressure Tracking Chart is available to download, print, and bring to every appointment.
Blood pressure is one of the most important numbers in cardiovascular medicine, and one of the most commonly neglected.
The reason it gets neglected is understandable: high blood pressure produces no symptoms. There is no pain, no obvious warning. A person can have significantly elevated blood pressure for years without knowing, while that pressure quietly and steadily damages artery walls, strains the heart, and raises the risk of stroke, heart attack, and kidney disease.
This is precisely why monitoring matters. Blood pressure is one of the most readily measurable cardiovascular risk factors, and one of the most modifiable. Detecting it early and tracking it over time puts you in a genuinely strong position to protect your heart.
What Is Blood Pressure?
Blood pressure is the force your circulating blood exerts on the walls of your arteries. It is expressed as two numbers, for example, 120/80 mmHg.
The first, higher number is the systolic pressure the pressure when the heart contracts and pumps blood out. The second is the diastolic pressure the pressure when the heart is relaxed and filling between beats. Both numbers matter and both contribute to cardiovascular risk.
Blood pressure is not fixed, it varies naturally throughout the day, rising during activity, stress, and stimulant intake, and falling during rest and sleep. What matters clinically is the sustained average over time, not any single reading.
Understanding the Numbers
| Category | Systolic (mmHg) | Diastolic (mmHg) | What it means |
|---|---|---|---|
| Normal | Below 120 | Below 80 | Optimal, maintain through healthy lifestyle |
| Elevated | 120–129 | Below 80 | Worth monitoring, lifestyle changes recommended |
| Hypertension Stage 1 | 130–139 | 80–89 | Discuss with your doctor, lifestyle changes ± medication |
| Hypertension Stage 2 | 140 or above | 90 or above | Medication usually recommended alongside lifestyle changes |
| Hypertensive crisis | Above 180 | Above 120 | Seek urgent medical assessment |
The key principle across all guidelines is consistent: the higher the sustained blood pressure, the greater the cardiovascular risk, and the greater the benefit of reducing it.
Why Home Monitoring Matters
White coat and masked hypertension
A single reading in a clinical setting tells you relatively little on its own. Many people experience a transient rise in blood pressure in clinical environments due to anxiety, a well-recognised phenomenon called white coat hypertension. Conversely, some people with normal clinic readings have elevated blood pressure at home and during daily activity, called masked hypertension. Neither is reliably detected by occasional clinic readings alone.
What home monitoring adds
A series of readings taken in a relaxed, familiar environment, at the same time of day, using a consistent technique, provides a much more accurate picture of your true average blood pressure.
For people already on blood pressure medication, home monitoring is one of the most useful ways to assess whether treatment is working effectively across the full day, rather than just at the moment of a clinic visit.
How to do it correctly
Step-by-step guide
Sit quietly for 5 minutes first
Avoid caffeine, exercise, and smoking for at least 30 minutes before measuring. Sit with your back supported and feet flat on the floor.
Use a validated upper arm monitor
Upper arm monitors are more accurate than wrist devices. Position the cuff on bare skin, at heart level, following the device instructions precisely.
Take two readings per session
Wait one minute between readings. Discard the first and record the second. Repeat morning and evening for at least five days.
Record and share your results
Note the date, time, and reading. Average the results and bring them to your next appointment, our free BP tracking chart makes this straightforward.
What Causes High Blood Pressure?
Primary hypertension, the most common type
In around 90 to 95% of cases, high blood pressure is primary, developing gradually over years as a result of genetic predisposition combined with lifestyle factors. Age, family history, obesity, physical inactivity, a diet high in salt and processed foods, excess alcohol, and chronic stress all contribute.
Secondary hypertension, an identifiable cause
In 5 to 10% of cases, hypertension is secondary to an underlying condition, kidney disease, hormonal disorders such as primary aldosteronism, sleep apnoea, or certain medications including the combined oral contraceptive pill and some anti-inflammatory drugs.
Secondary causes are more likely in younger patients, those with very difficult-to-control blood pressure, or those with specific clinical features. Investigating for them is part of a thorough hypertension assessment.
Treatment
Lifestyle first
Blood pressure management begins with lifestyle. Regular aerobic exercise consistently reduces blood pressure. A diet low in salt, below 5 to 6 grams per day, and rich in vegetables, fruit, whole grains, and lean protein supports blood pressure control. Reducing alcohol, maintaining a healthy weight, managing stress, and treating sleep apnoea where present all contribute meaningfully.
Medication when needed
For those whose blood pressure remains above target despite lifestyle modification, or those at high overall cardiovascular risk, medication is appropriate and effective. ACE inhibitors, ARBs, calcium channel blockers, and thiazide diuretics are the main classes used, often in combination. The right choice depends on your individual circumstances, other conditions, and other medications you take.
One of the most common conversations I have with patients is explaining that blood pressure medication, when it is needed, is not a sign of failure or weakness, it is a recognition that genetics plays a powerful role in blood pressure, and that medication and lifestyle work best together. Many people need both.
- What is my target blood pressure, given my other risk factors?
- Should I be monitoring at home, and how often?
- Could white coat hypertension be affecting my clinic readings?
- Is my current medication working effectively across the full day?
- Are there secondary causes of hypertension worth investigating in my case?
Free Download, Heart Matters
Our Blood Pressure Tracking Chart provides a clean layout for recording home readings, with columns for systolic, diastolic, and heart rate, space for notes, and target range guidance. Free to download, print, and bring to every appointment.
Heart Matters Resource
When in Doubt, Get Checked Out
If your home readings are consistently above 130/80, or if you experience a sudden severe headache, visual disturbance, or chest pain alongside an elevated reading, contact your doctor promptly rather than waiting to see if it settles.
Conclusion
Blood pressure monitoring is one of the simplest and most impactful things you can do for your cardiovascular health. A modest investment of time and an inexpensive device gives you direct visibility of one of the most important risk factors for heart disease, stroke, and kidney disease.
If you don’t know your blood pressure, finding out is a good first step. If you do know it and it is elevated, taking it seriously, with lifestyle changes, medication where needed, and consistent monitoring, is one of the most effective cardiovascular protection strategies available.
Used consistently and shared with your doctor, home blood pressure records are genuinely useful clinical information. Bring them to every appointment.