- Inflammation is the body’s essential healing response, but when it becomes chronic and low-grade, it actively drives atherosclerosis and significantly raises cardiovascular risk.
- In some cardiac conditions, pericarditis, myocarditis, and rheumatic heart disease, inflammation is not a background risk factor but the primary disease mechanism itself.
- High-sensitivity CRP (hs-CRP) is the most widely used blood marker of cardiovascular inflammation and is increasingly used alongside traditional risk factors to refine risk assessment.
- Most lifestyle changes that benefit cardiovascular health also directly reduce inflammatory burden, exercise, Mediterranean diet, smoking cessation, and weight loss all work partly through anti-inflammatory pathways.
- Colchicine, a well-established anti-inflammatory, has recently demonstrated significant reductions in cardiovascular events in clinical trials, representing a major advance in directly targeting inflammation.
When most people think about cardiovascular risk, they think about cholesterol, blood pressure, and smoking. These are the well-established pillars of prevention and remain critically important.
But inflammation plays a central role in heart disease that goes well beyond the traditional risk factors, and it operates in two quite different ways. In atherosclerosis, chronic low-grade inflammation quietly drives plaque formation and instability over decades. In conditions like pericarditis, myocarditis, and rheumatic heart disease, inflammation is not a background contributor, it is the primary disease process itself.
Understanding the role inflammation plays across these different contexts is increasingly important for anyone navigating a cardiac diagnosis.
Inflammation, the Basics
When it helps
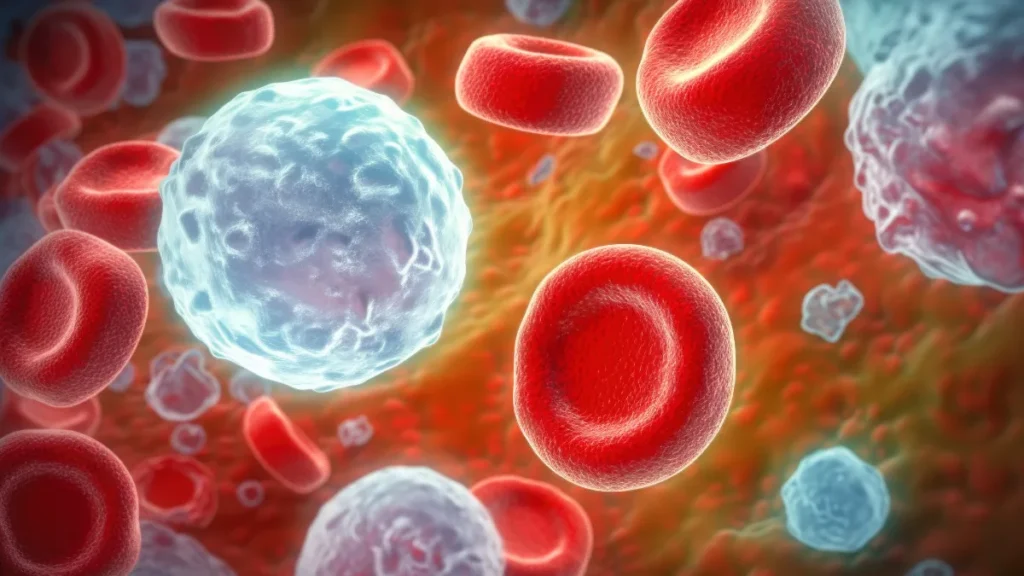
Acute inflammation is entirely beneficial. When the body detects tissue damage or infection, the immune system mobilises rapidly, white blood cells are recruited, inflammatory proteins are released, and healing begins. This is the redness, warmth, and swelling of a wound, visible and purposeful.
When it harms
The problem arises when inflammation becomes chronic and systemic, a persistent, low-level activation of the immune system that doesn’t switch off. This kind of inflammation produces no obvious symptoms. But at the level of the blood vessel wall, it quietly and persistently promotes the processes that lead to atherosclerosis and cardiovascular events.
Inflammation and Atherosclerosis
How plaques form
When the inner lining of arteries, the endothelium, is damaged by high blood pressure, oxidised LDL cholesterol, cigarette toxins, or elevated blood sugar, it becomes dysfunctional and inflamed. This damaged lining signals to immune cells, which migrate into the artery wall and begin engulfing lipid deposits, forming the foam cells that are the building blocks of atherosclerotic plaque.
Inflammation doesn’t only initiate plaque formation, it also determines how dangerous existing plaques are. A plaque rich in inflammatory cells with a thin fibrous cap is vulnerable, more likely to rupture suddenly and trigger the clot formation that causes a heart attack.
What drives chronic inflammation
Obesity
Visceral fat releases inflammatory cytokines continuously, one of the most powerful drivers of chronic systemic inflammation.
Smoking
Activates inflammatory pathways directly through chemical toxins delivered to the circulation with every cigarette.
Physical inactivity
A sedentary lifestyle is pro-inflammatory. Conversely, regular moderate exercise has well-documented anti-inflammatory effects.
Poor diet
Refined carbohydrates, saturated fat, and ultra-processed foods promote inflammation. Mediterranean-style diets consistently reduce inflammatory markers.
Diabetes and insulin resistance
Elevated blood sugar damages the vessel wall directly and drives inflammation through multiple metabolic pathways.
Chronic stress and poor sleep
Sustained sympathetic nervous system activation and sleep apnoea both raise inflammatory markers through distinct but overlapping pathways.
When Inflammation Is the Primary Disease
In atherosclerosis, inflammation is a driver operating in the background over decades. In some cardiac conditions, it moves to the foreground entirely, the inflammation itself is the diagnosis.
Pericarditis
The pericardium is the thin sac surrounding the heart. Pericarditis is inflammation of this sac, most commonly triggered by a viral infection, though it can occur after a heart attack, following cardiac surgery, or in the context of autoimmune conditions.
The hallmark symptom is sharp chest pain that is typically worse when lying flat and better when sitting forward. It can closely mimic the chest pain of a heart attack, which is why urgent assessment is always appropriate. Blood tests show elevated inflammatory markers, and an ECG and echocardiogram are used to confirm the diagnosis and assess for fluid around the heart.
Most cases of acute pericarditis resolve with anti-inflammatory treatment, NSAIDs and colchicine are the mainstays. Colchicine in particular has been shown in clinical trials to significantly reduce the risk of pericarditis recurring, which is one of the more troublesome aspects of the condition for some patients.
Myocarditis
Myocarditis is inflammation of the heart muscle itself, most commonly caused by a viral infection, though it can also occur as a reaction to medications, toxins, or in the context of autoimmune disease.
It can present in many ways, from mild breathlessness and palpitations to severe heart failure or dangerous arrhythmias. In young people and athletes, myocarditis is one of the more important causes of sudden cardiac death, which is why any unexplained cardiac symptoms following a recent viral illness should be assessed promptly.
Cardiac MRI is the investigation of choice, it can identify the characteristic pattern of myocardial inflammation and oedema with high sensitivity. Treatment is primarily supportive, with rest and avoidance of strenuous exercise while active inflammation is present.
Rheumatic heart disease
Rheumatic fever is an inflammatory condition triggered by an immune response to group A streptococcal infection, the same bacteria responsible for strep throat. In susceptible individuals, the immune response misfires and attacks the heart’s own tissues.
The lasting damage from rheumatic fever, rheumatic heart disease, primarily affects the heart valves. The mitral valve is most commonly involved, leading to mitral stenosis or regurgitation that may not become clinically apparent until decades after the original infection. Rheumatic heart disease remains a major cause of acquired valve disease worldwide, particularly in low and middle income countries.
Prevention is the most important strategy, prompt antibiotic treatment of streptococcal throat infections prevents the inflammatory cascade. For those who have already had rheumatic fever, long-term penicillin prophylaxis reduces the risk of recurrence and further valve damage.
Inflammation connects some of cardiology’s most important conditions, from the slow burn of atherosclerosis over decades, to the acute chest pain of pericarditis, to the lasting valve damage of rheumatic fever. Understanding the inflammatory mechanism in each of these is genuinely useful for patients, it explains the treatment, the monitoring, and often the prognosis.
Measuring Inflammation, hs-CRP
High-sensitivity C-reactive protein (hs-CRP) is the most widely used blood marker of cardiovascular inflammation. It is produced by the liver in response to inflammatory signalling, and the high-sensitivity assay detects the very low levels associated with chronic vascular inflammation.
| hs-CRP level | Cardiovascular inflammatory risk | Interpretation |
|---|---|---|
| Below 1 mg/L | Low | Reassuring, low inflammatory burden |
| 1–3 mg/L | Intermediate | Worth considering alongside other risk factors |
| Above 3 mg/L | Elevated | Suggests meaningful inflammatory cardiovascular risk, warrants review |
hs-CRP is increasingly used to refine risk stratification, particularly in people at intermediate risk based on traditional factors, where an elevated result can tip the balance toward more intensive prevention. It was central to the JUPITER trial, which showed statin therapy reduced cardiovascular events in people with normal LDL but elevated hs-CRP.
What Can Be Done
Lifestyle, the foundation
The same lifestyle changes that benefit cardiovascular health broadly also reduce inflammatory burden directly. Regular exercise reduces hs-CRP and a range of inflammatory markers, as few as 150 minutes of moderate activity per week produces measurable effects. A Mediterranean-style diet consistently reduces inflammatory markers. Smoking cessation reduces inflammatory activation rapidly after quitting. Weight loss, particularly of visceral fat, produces substantial reductions in hs-CRP.
Statins, more than cholesterol lowering
Statins have anti-inflammatory effects on plaques beyond their LDL-lowering action, they reduce hs-CRP and stabilise plaque composition. This is one reason why their benefits extend to patients with normal LDL and elevated inflammatory markers, and why they remain one of the most broadly effective cardiovascular medications available.
Colchicine, a landmark advance
The most significant recent development in directly targeting cardiovascular inflammation is the emergence of colchicine as a cardiovascular therapy. Long established for gout and pericarditis, colchicine’s role in coronary disease was confirmed by two landmark trials, COLCOT (2019) and LoDoCo2 (2020), which demonstrated that low-dose colchicine significantly reduced major cardiovascular events in patients with established coronary artery disease, independent of statin therapy.
This represents the first direct clinical trial evidence that targeting the inflammatory pathway in atherosclerosis translates into meaningful reductions in heart attacks and strokes. Colchicine is now incorporated into guidelines as a treatment option for selected patients with established coronary disease.
Free Download, Heart Matters
Our Heart Health Risk Factor Checklist covers 12 cardiovascular risk categories, including lifestyle factors that drive inflammation, with a traffic light self-assessment and space for questions to raise with your doctor.
Heart Matters Resource
When in Doubt, Get Checked Out
If you have established cardiovascular disease and want to understand your inflammatory risk, or if your hs-CRP has been flagged as elevated, it is worth a conversation with your cardiologist about what this means for your treatment.
Conclusion
Inflammation connects some of cardiology’s most important conditions, from the slow burn of atherosclerosis, to the acute chest pain of pericarditis, to the lasting valve damage of rheumatic fever. Recognising this connection matters, because it shapes both the diagnosis and the treatment.
For most people, the most powerful anti-inflammatory interventions available are not medications, they are lifestyle. Exercise, diet, not smoking, managing weight. These work through multiple pathways simultaneously, and their anti-inflammatory effects are one of the most important reasons why they work so well.
Where medication is needed, statins, colchicine, targeted therapy for specific conditions, the evidence now supports direct anti-inflammatory treatment as part of comprehensive cardiovascular care. That is a genuinely meaningful advance for patients who remain at risk despite optimal conventional therapy.