- CABG reroutes blood around blocked coronary arteries and remains the gold standard for complex, multi-vessel disease.
- More grafts is not a bad sign, it reflects the extent of disease and the surgeon’s commitment to complete revascularisation.
- For left main artery disease, triple-vessel disease, or diabetes, surgery consistently outperforms stenting for long-term outcomes.
- Both stents and bypass grafts can last a lifetime, the key is maintaining them through medicines and risk factor control.
There is a moment in every bypass operation that never loses its significance. The new graft is sewn in place, the clamps are released, and blood flows, for the first time in perhaps years, into a part of the heart that had been starved of it. The heart responds almost immediately. That restoration of flow is what coronary artery bypass grafting is fundamentally about.
CABG (pronounced “cabbage”) is one of the most common and well-studied cardiac operations performed worldwide. It involves creating a new route for blood to travel around a blocked or narrowed coronary artery, restoring circulation to the heart muscle and dramatically reducing the risk of heart attack. For many patients, particularly those with complex or multi-vessel disease, it offers outcomes that no other treatment can match.
The operation was first performed by Dr René Favaloro, an Argentinean surgeon, in 1960. In the six decades since, the techniques, grafts, and perioperative care have advanced enormously, but the fundamental principle remains unchanged: give the heart the blood supply it needs.
Who Needs CABG?
CABG is usually recommended when coronary artery disease is too extensive or complex for stenting alone, particularly when multiple arteries are affected, or when the most critical artery supplying the heart is severely diseased.
Surgery is most commonly advised for patients with severe narrowing or blockage affecting the left main coronary artery, which supplies a dominant share of the heart’s blood, or those with significant disease across multiple coronary arteries. It is also considered when angioplasty or stenting has failed, or is technically not feasible given the anatomy of the disease.
Patients with coexisting valve conditions are another important group. When valve repair or replacement is needed alongside coronary revascularisation, CABG and valve surgery can be performed in the same operation, addressing both problems at once.
CABG vs. Stenting: How We Decide
Stenting and bypass surgery are both effective treatments for coronary artery disease, but they are not interchangeable. The decision between them depends on the pattern of disease, your overall health, and the evidence for long-term outcomes in your specific situation. Here is how the two approaches compare across the factors that matter most.
| Factor | CABG Surgery | Stenting (PCI) |
|---|---|---|
| Invasiveness | Major surgery, general anaesthesia | Minimally invasive, local anaesthesia |
| Best for | Left main disease, triple-vessel disease, diabetes, complex anatomy | Single or double vessel disease, simpler anatomy, higher surgical risk |
| Long-term outcomes | Superior evidence in complex disease | Excellent in simpler disease |
| Antiplatelet therapy | Aspirin alone usually sufficient | Dual antiplatelet therapy required (higher bleeding risk) |
| Recovery time | 6–12 weeks | Days to weeks |
| Repeat procedures | Less likely long-term | Higher rate of re-intervention |
| Longevity | Both can last a lifetime, with the right medicines and risk factor control | |
One important advantage of CABG over stenting that is often overlooked: patients who have bypass surgery typically only need aspirin long-term, rather than dual antiplatelet therapy (two blood thinners). For patients who need dental procedures, other surgeries, or who are at higher risk of bleeding, this is a meaningful practical benefit.
Factors that may push the decision toward stenting include high anaesthetic risk, significant respiratory disease, a history of stroke or cerebrovascular disease, or other comorbidities that make a major operation less safe. This is why every case deserves careful individual assessment, there is no one-size-fits-all answer.
The Heart Team
The decision to recommend CABG is never made by a single doctor in isolation. Modern cardiac care is built around the concept of the multidisciplinary heart team, cardiologists, cardiothoracic surgeons, anaesthesiologists, imaging specialists, and cardiac nurses reviewing each case together and reaching a consensus on the best treatment path.
This matters enormously. The choice between stenting and surgery is rarely black and white, and it should never be driven by the specialty of whoever happens to be in the room. A proper heart team discussion ensures every option is evaluated on its merits, the risks are weighed against the individual patient’s profile, and the recommendation reflects the collective expertise of the full team. If you are facing this decision, it is entirely reasonable to ask whether your case has been discussed in this way.
Single, Double, Triple and Quadruple Bypass, What Does It Mean?
One of the most common questions patients ask is: does having more bypasses mean my disease is worse? The answer is nuanced, and more reassuring than most people expect.
The number of grafts reflects the extent of disease across the coronary arteries. More grafts means more complete revascularisation, and that is exactly what we are aiming for. A quadruple bypass is not worse than a double; in many cases it means the surgeon has been more thorough.
A single bypass addresses one blocked artery; double, triple, and quadruple bypasses address two, three, or four respectively. The goal in every case is complete revascularisation restoring adequate blood supply to every region of the heart that needs it. Surgeons prioritise the vessels supplying the most critical territories, with the left anterior descending (LAD) artery almost always at the top of that list.
Learn more about how blood flows through the heart on our dedicated Heart Basics page.
The Left Anterior Descending (LAD) Artery
The left anterior descending (LAD) artery is often called the “widow maker”, a stark reflection of its importance. It supplies blood to the largest territory of the left ventricle, the heart’s main pumping chamber. Significant blockage of the LAD carries serious prognostic implications, and bypassing it, typically with the left internal mammary artery, is one of the most durable and impactful things a cardiac surgeon can do for a patient.
The evidence for CABG over stenting is particularly strong when the left main artery or LAD is involved. In these situations, surgery offers a more robust long-term result, and this is one of the most important factors in the heart team’s decision-making process.
Choosing the Right Grafts
Arterial grafts are the preferred choice wherever possible. The left internal mammary artery (LIMA), harvested from inside the chest wall, is the workhorse of modern bypass surgery, when connected to the LAD, it can remain open and functional for 20 years or more, with a blockage rate below 10%. The right internal mammary artery (RIMA) and the radial artery from the forearm are also frequently used.
Venous grafts taken from the saphenous vein in the leg, are used when there are insufficient arterial conduits available. They are easier to harvest and versatile, but their lifespan is shorter, roughly 10–20% close within the first year after surgery, and approximately half are affected within ten years. This is why surgeons aim to maximise arterial grafting wherever feasible.
years arterial grafts can last
blockage rate for LIMA grafts over 20 years
how long grafts can last with the right care
I tell my patients that stents and bypass grafts can last a lifetime, the surgery gives you the infrastructure, but it is the medicines and lifestyle choices afterwards that keep them working.
The Surgical Procedure: What to Expect
You will be admitted to hospital and cared for by a team that includes your cardiothoracic surgeon, cardiologist, anaesthesiologist, and specialist cardiac nurses. Before the operation, an anaesthesiologist will review your full medical history, confirm the anaesthetic plan, and answer your questions.
The surgery typically lasts 3 to 6 hours, depending on the number of arteries being bypassed.
The surgeon makes a single incision down the centre of the chest, a sternotomy to access the heart. The heart is briefly stopped while the new grafts are sewn into place. Once all grafts are complete and blood flow is confirmed, the heart is restarted and the chest is carefully closed.
On-Pump and Off-Pump Surgery
On-pump CABG uses a cardiopulmonary bypass machine (the heart-lung machine) to circulate oxygenated blood while the heart is stopped, giving the surgeon a still, bloodless field. Off-pump CABG performs the grafts on a beating heart using mechanical stabilisers to minimise movement at the area being sutured.
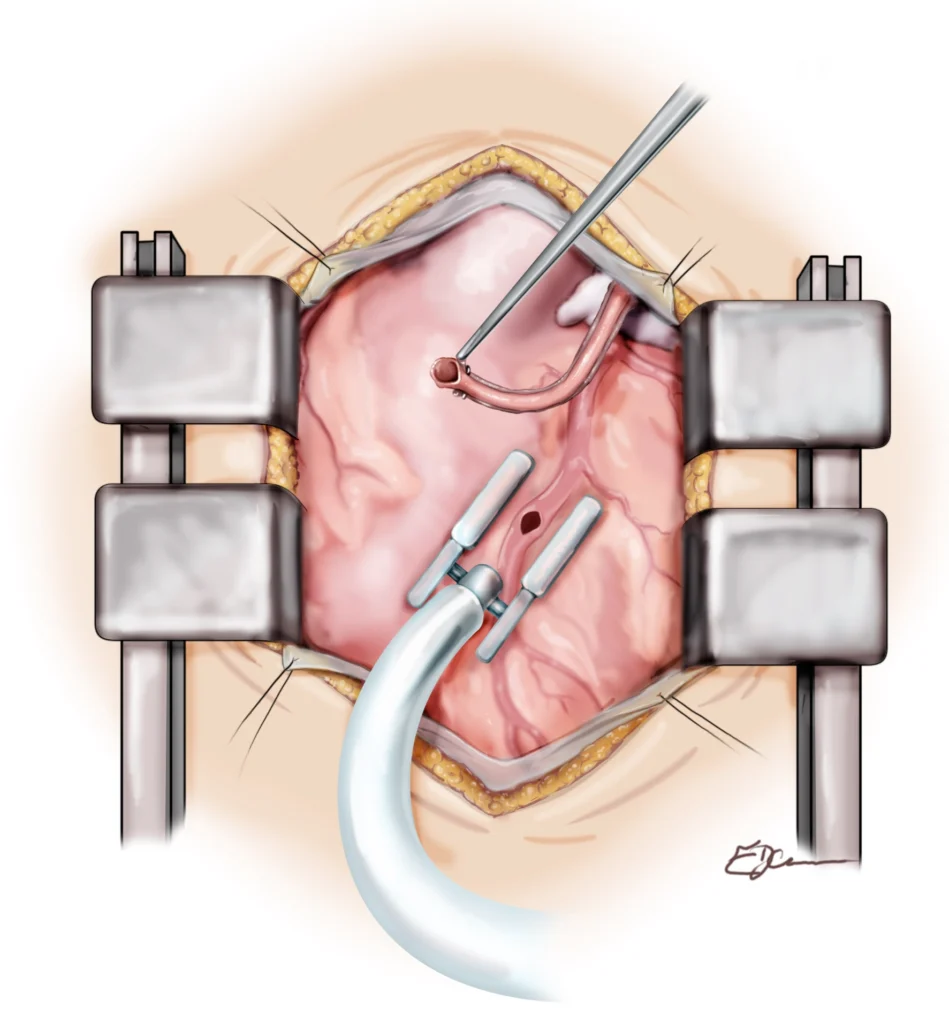
Off-pump surgery may reduce certain complications, particularly relevant for patients at higher stroke or kidney risk, though both approaches produce excellent results in experienced hands. The choice between them is made by the surgeon based on your individual anatomy and health profile.
The Heart-Lung Machine
The heart-lung machine, operated by a specialist called a perfusionist temporarily takes over the work of your heart and lungs during surgery. It drains blood from the heart, replenishes its oxygen, and pumps it back at a controlled rate and pressure. It is one of the most remarkable pieces of technology in modern medicine, and its safe operation is central to the success of every bypass procedure.
Brain Fog After Bypass, What Patients Tell Us
One of the most commonly reported experiences after bypass surgery is a period of cognitive cloudiness, difficulty concentrating, mild memory lapses, a sense of mental slowness. Patients often describe it as feeling “not quite themselves” for weeks or even months after the operation. This is real, it is common, and it deserves an honest explanation.
When blood is routed through the bypass machine, the pattern of flow to the brain is temporarily different to normal. Tiny air bubbles or microscopic particles can occasionally reach the cerebral circulation, and the non-pulsatile flow of the machine differs from the natural rhythm of the beating heart. The brain, highly sensitive to these changes, can show a temporary reduction in function as a result.
The good news is that in the vast majority of patients, these effects are fully reversible. Most people find their mental sharpness returns to normal within 3 to 6 months. Off-pump surgery may reduce the incidence of these effects, and this is one of the factors surgeons weigh when deciding which technique to use. If you notice cognitive changes after surgery, tell your surgical team, it is a recognised and well-understood phenomenon, not a sign that something has gone wrong.
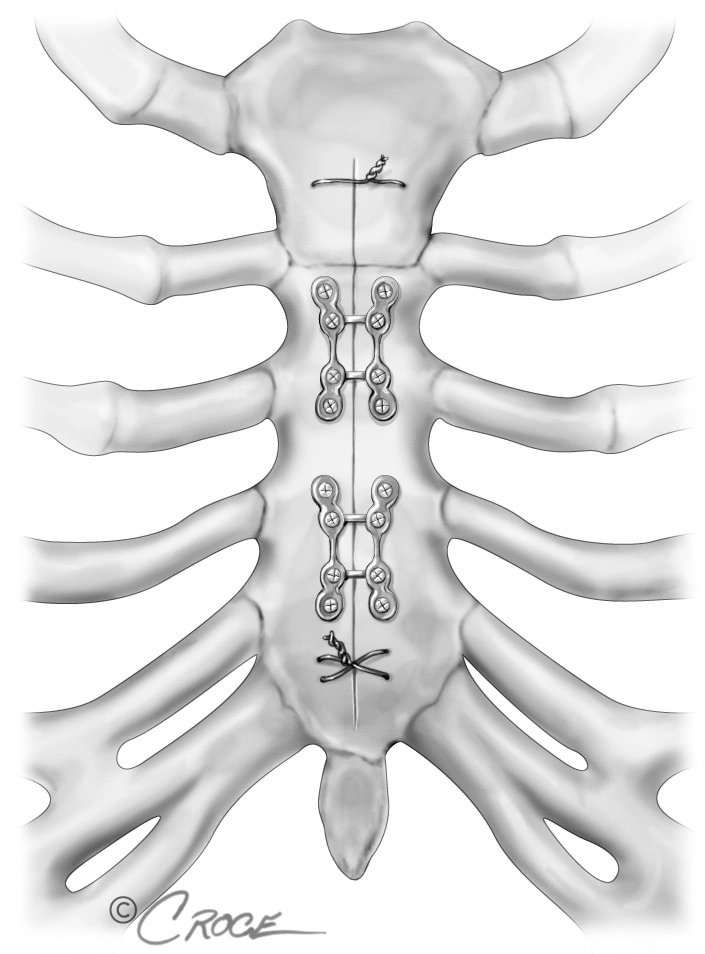
Closing the Chest
Once the grafts are in place and the heart is beating well, the sternum is carefully brought back together and secured, either with stainless steel wires (the traditional, time-tested method) or with rigid titanium plate systems that provide superior stability, particularly for patients at higher risk of sternal complications.
Understanding the Risks
CABG is a major operation and carries real risks, it would be wrong to minimise that. But context matters: when surgery is recommended, it is because the risk of not operating is judged to be greater than the risk of the procedure itself. The risks below vary considerably depending on your individual health profile, and your surgical team will give you a personalised assessment before any decision is made.
Cardiac risks include arrhythmias (irregular heart rhythms), which are common and usually temporary, and, rarely, a perioperative heart attack.
Neurological risks include stroke, which occurs in a small percentage of patients, and temporary cognitive changes such as the brain fog described above. These effects typically resolve over weeks to months.
Wound and infection risks include bleeding, superficial wound infection, and, less commonly, deep sternal wound infection, which is a more serious but manageable complication.
Organ-related risks include temporary changes to kidney function and breathing difficulties in the early post-operative period. Both are closely monitored and usually resolve with appropriate support.
Other risks include blood clots, fluid accumulation around the heart or lungs, graft failure, and the emotional and psychological adjustment that can follow major heart surgery. Anxiety and low mood post-operatively are common and entirely normal, good cardiac rehabilitation programmes address this directly.
Patients with pre-existing conditions such as diabetes, COPD, kidney disease, cerebrovascular disease, or a prior stroke face a somewhat elevated risk profile. This is why the conversation with your cardiologist and surgeon before the operation is so important.
Recovery: Your Day-by-Day Journey
Knowing what to expect at each stage of recovery makes the whole experience significantly less daunting. Here is a typical timeline, though every patient’s journey is individual.
Surgery Day
You are admitted, prepared, and taken to the operating room. General anaesthesia is administered, the surgery takes 3–6 hours, and you are transferred directly to the ICU when complete.
ICU, Days 1 to 2
You will spend 24–48 hours in the ICU on average. Do not be alarmed by the number of lines and monitors, these are standard post-operative monitoring tools, not a sign that anything is wrong. You will have a breathing tube (usually removed within 24 hours), arterial lines, IV drips, drain tubes from the chest, and temporary pacing wires as a precaution. Your team will be watching everything closely.
Ward, Days 3 to 7
You move to the cardiac ward. Drain tubes and pacing wires are removed. You begin sitting up, walking short distances, and cardiac rehabilitation starts. Most patients go home around day 7.
Home, Weeks 1 to 6
Gradual increase in activity. The sternum takes 6–8 weeks to heal solidly, avoid heavy lifting and certain upper body movements during this period. Outpatient cardiac rehabilitation continues.
Return to Normal, Weeks 6 to 12
Most patients return to driving, work, and normal activity within 6–12 weeks. Energy levels and cognitive sharpness continue to improve through this period.
Medicines After Surgery
You will leave hospital on a carefully considered medication regimen, typically aspirin, cholesterol-lowering therapy, and blood pressure medication. These are not temporary, they are long-term tools that protect your grafts and slow the progression of coronary artery disease. A full overview of medications used in coronary artery disease is on our Coronary Artery Disease page.
Cardiac Rehabilitation
Cardiac rehabilitation is not optional, it is one of the most effective interventions available after bypass surgery. A structured programme combining supervised exercise, education, dietary guidance, and psychological support begins in hospital and continues as an outpatient programme for several weeks. Patients who complete cardiac rehab have measurably better outcomes and significantly improved quality of life.

Protecting Your Grafts Long-Term
Surgery restores blood flow, but how long those grafts last depends significantly on what happens next. Optimising your cardiovascular risk factors is essential: not smoking, controlling blood pressure and diabetes, managing cholesterol, and staying physically active. Compliance with your prescribed medicines is equally important.
I tell every patient the same thing: your grafts and stents can last a lifetime. The surgery gives you the infrastructure, your job is to maintain it.
Conclusion
CABG surgery is a highly effective treatment for severe coronary artery disease, particularly in patients with left main or multi-vessel disease, diabetes, or coexisting valve conditions. The number of grafts is not something to fear; it reflects the thoroughness of the revascularisation. Recovery takes several weeks, but most patients return to full activity with significantly improved heart health and quality of life. The surgery gives you the infrastructure, the medicines, the rehabilitation, and the lifestyle choices are what keep it working for a lifetime.
Heart Matters Resource
When in Doubt, Get Checked Out
If you have been told you may need bypass surgery and want to understand your options, or if you have had CABG and have questions about your recovery or long-term care, speak with your cardiologist or cardiothoracic surgeon. Good information and the right specialist team make an enormous difference.