- An echocardiogram, “echo”, is an ultrasound of the heart, using sound waves to create real-time images of the chambers, valves, walls, and blood flow.
- It is the most important imaging test in cardiology for assessing cardiac structure and pump function, measuring ejection fraction, valve function, wall thickness, and chamber size.
- Completely non-invasive, painless, no radiation, and takes approximately 30–45 minutes.
- Requested across an enormous range of clinical situations, from investigating a murmur or breathlessness to monitoring heart failure, assessing the heart before surgery, or following a heart attack.
- Specialised forms include the stress echocardiogram and the transoesophageal echocardiogram (TOE/TEE), both covered in dedicated articles in this section.
If the ECG is the heart’s electrical portrait, the echocardiogram is its structural one. Where the ECG tells you about rhythm and electrical signals, the echo shows you the physical heart, how large the chambers are, how the walls move with each contraction, whether the valves open and close properly, and how blood flows through the cardiac structures.
It answers questions about structure and function that no other investigation addresses as comprehensively, safely, and non-invasively. For many patients it is the investigation that finally explains their symptoms.
How It Works
Sound waves, not radiation
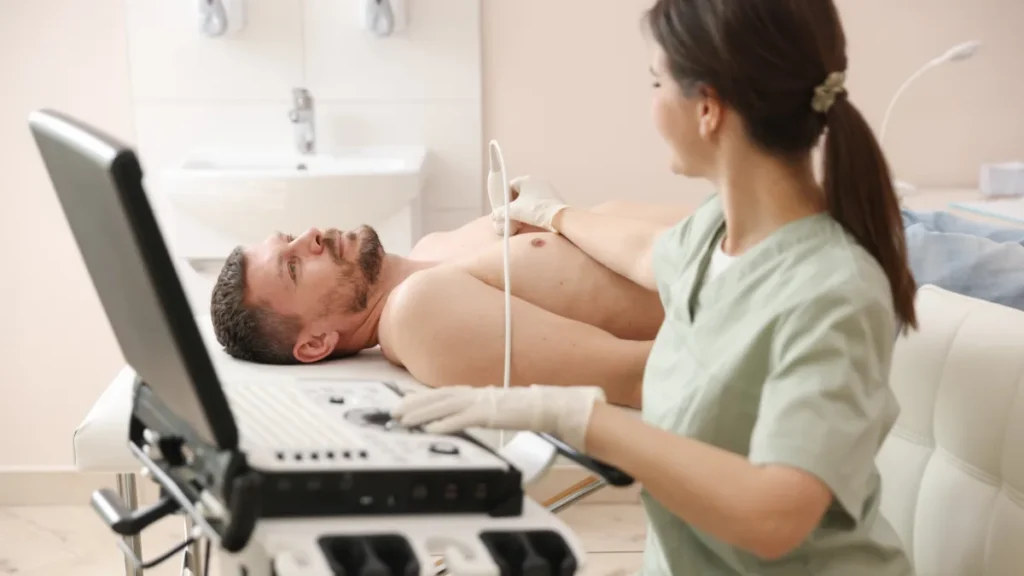
An echocardiogram uses the same ultrasound physics as a pregnancy scan, high-frequency sound waves emitted from a handheld probe, reflected back from internal structures, and converted into images on a monitor. There is no radiation involved at any point.
The cardiac sonographer positions the probe on the skin of the chest, applying a clear gel to eliminate the air gap between probe and skin, air blocks ultrasound transmission. By moving the probe to different positions around the chest, multiple viewing angles are obtained, providing a comprehensive assessment of every cardiac structure.
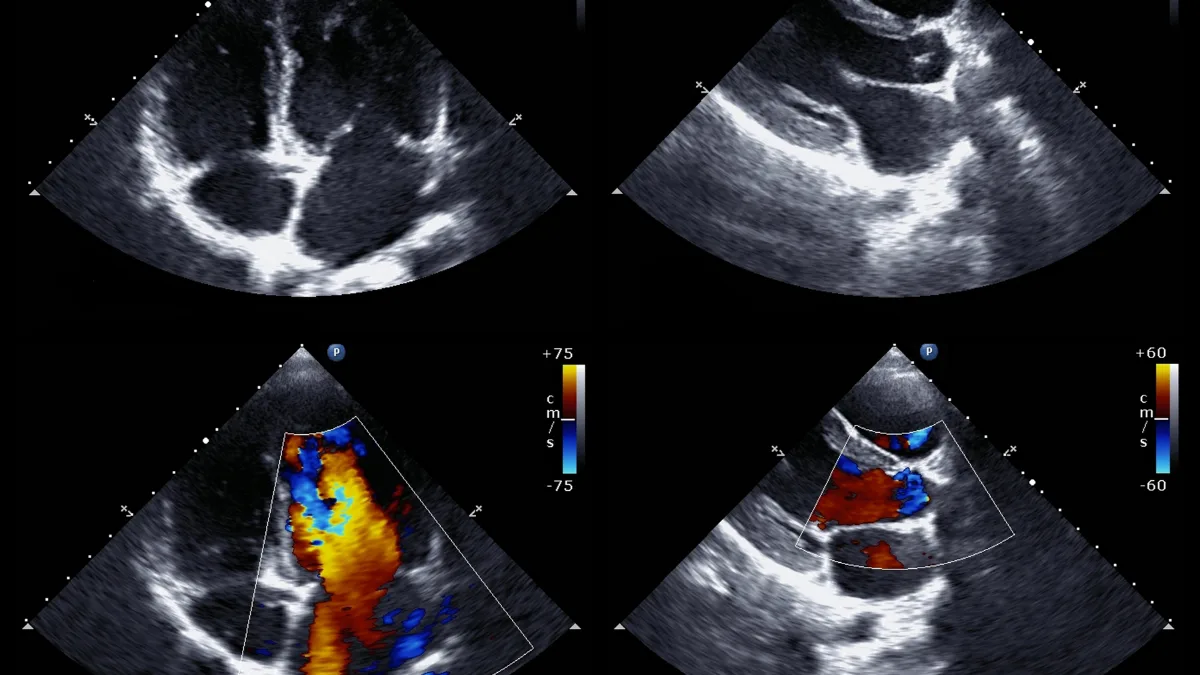
Doppler imaging, measuring blood flow
Modern echocardiography also uses Doppler imaging, which detects the speed and direction of blood flow through the heart. This allows the cardiologist to measure the severity of any valve narrowing or leaking with precision, tracking changes over time and informing decisions about whether and when surgical intervention is needed.
What an Echo Can Show
The echocardiogram provides information across multiple dimensions simultaneously, making it one of the most comprehensive single investigations available in cardiology.
Key measurements and findings
Ejection fraction
The percentage of blood pumped out with each beat, normally above 55%. The primary measure of systolic heart function.
Chamber dimensions
Whether the heart is enlarged in response to volume or pressure overload, informing diagnosis and management decisions.
Valve function
All four valves assessed for stenosis (narrowing) and regurgitation (leaking), with Doppler quantifying severity precisely.
Wall motion
Areas of the ventricle contracting poorly can indicate previous heart attack, ischaemia, or cardiomyopathy.
Pericardial effusion
Fluid around the heart, detected immediately and quantified. Can indicate pericarditis, malignancy, or other conditions.
Structural abnormalities
Congenital defects, cardiac masses, and other structural findings, often first identified on a routine echo.
What to Expect
What to Expect, Transthoracic Echocardiogram (TTE)
Duration
30–45 minutes for a comprehensive study. Brief targeted studies in an emergency may take 10–15 minutes.
Preparation
No fasting or special preparation required. Wear comfortable clothing that allows access to the chest.
Comfort
Painless and non-invasive. You lie on your left side for much of the study, this moves the heart closer to the chest wall for better images. The gel is cold initially. Occasionally firmer probe pressure is needed for better image windows.
Radiation / Contrast
No radiation. Ultrasound only. For some studies, a microbubble ultrasound contrast agent may be injected to improve image quality, this is not iodine contrast and is different from CT contrast.
Results
Interpreted by a cardiologist from recorded images. A formal report is typically available within a few days and discussed at follow-up.
Afterwards
No restrictions. Drive home and resume normal activities immediately. The gel washes off easily.
Why Your Cardiologist Has Requested One
The echocardiogram is one of the most broadly requested investigations in cardiology, because structural and functional information about the heart is relevant across an enormous range of clinical situations.
Common reasons include investigation of a cardiac murmur heard through the stethoscope; assessment of breathlessness where a cardiac cause is possible; baseline assessment and monitoring of known valve disease or heart failure; evaluation of cardiac function after a heart attack; assessment before cardiac surgery or other major procedures; investigation of atrial fibrillation to assess left atrial size and ventricular function; evaluation of suspected cardiomyopathy; and monitoring the cardiac effects of some cancer chemotherapy agents.
The echocardiogram often provides the single most important piece of information in a cardiac assessment. Knowing the ejection fraction, the valve function, and the chamber dimensions simultaneously, in real time, without any radiation or invasive procedure, is remarkable. It is the investigation I rely on most in clinical practice.
Types of Echocardiogram
Standard transthoracic echocardiogram (TTE)
The most common form, probe on the chest wall. The starting point for most echocardiographic assessment and the investigation described in this article.
Stress echocardiogram
Combines a TTE with exercise on a treadmill or bicycle, or a pharmacological stress agent, to assess how the heart responds to increased demand. Used primarily to detect coronary artery disease and assess valve function under load. We have a dedicated article on the stress echocardiogram in this section.
Transoesophageal echocardiogram (TOE/TEE)
Passes the probe into the oesophagus for superior imaging of posterior cardiac structures, particularly the mitral valve, the left atrium, and the aorta. Used when a standard TTE cannot provide sufficient detail, or when very high-resolution images are needed for procedural planning. Covered in a dedicated article in this section.
- What is my ejection fraction, and what does that number mean for my situation?
- Were any valve abnormalities identified, and if so, how significant are they?
- Will I need a repeat echo, and if so, how often?
- Is a stress echo or TOE needed to provide additional information?
- What did the echo show that the ECG or other tests could not?
Heart Matters Resource
When in Doubt, Get Checked Out
Breathlessness, a cardiac murmur, palpitations, or chest discomfort that has not been explained, an echocardiogram is often one of the first and most informative steps towards an answer.
Conclusion
The echocardiogram is one of cardiology’s most versatile and informative investigations, answering questions about structure, function, and blood flow that no blood test or ECG can provide, with no radiation and no invasive procedure required.
Whether it is confirming a normal ejection fraction in someone worried about their heart, quantifying the severity of valve disease that needs monitoring, or identifying wall motion abnormalities after a heart attack, the information it provides directly shapes clinical decisions.
If you have had an echo and are unsure what the report means, the questions box above is a good starting point for your next conversation with your cardiologist.