Key Points
- A pacemaker is a small device that sends electrical signals to the heart to keep it beating at a safe, regular rate, used when the heart’s own electrical system is too slow or unreliable.
- Traditional pacemakers are excellent, proven devices that have served millions of people reliably for decades. They sit under the skin and connect to the heart via thin wires called leads, which work well for the vast majority of patients.
- Leadless pacemakers are a newer alternative, tiny devices implanted directly inside the heart through a catheter, with no wires and no visible lump under the skin.
- Until recently, leadless pacemakers could only pace one chamber of the heart, limiting who could receive them. A dual-chamber system has now received regulatory approval in the United States and Europe, though it remains an emerging technology not yet available at all centres.
- Conventional pacemakers remain the proven standard of care for most patients today. Leadless technology is a promising development that will no doubt expand in the years ahead as clinical evidence grows.
When the heart beats too slowly, or pauses for too long, it can cause dizziness, blackouts, extreme fatigue, or in serious cases, a life-threatening loss of consciousness. A pacemaker solves this by stepping in whenever the heart needs it, delivering a small electrical nudge that triggers a beat.
Pacemakers have been saving and improving lives for more than six decades. But the technology has not stood still. A significant development is underway, one that removes the wires entirely and changes what it means to have a pacemaker implanted. This technology is still emerging, and conventional pacemakers remain the standard of care for most patients, but the direction of progress is worth understanding.
Why do people need pacemakers?
The heart has its own electrical system, a network of specialised cells that generate and conduct the signals that trigger each beat. When this system develops problems, the heart can beat too slowly, pause unpredictably, or lose the coordinated timing between its upper and lower chambers.
The most common reasons a pacemaker is needed include a naturally slow heart rate that causes symptoms, a condition called heart block where the electrical signal between the upper and lower chambers is delayed or blocked, and sick sinus syndrome where the heart’s natural pacemaker, a cluster of cells in the right atrium, becomes unreliable. Atrial fibrillation can also sometimes lead to a very slow ventricular rate that requires pacing.
How does a traditional pacemaker work?
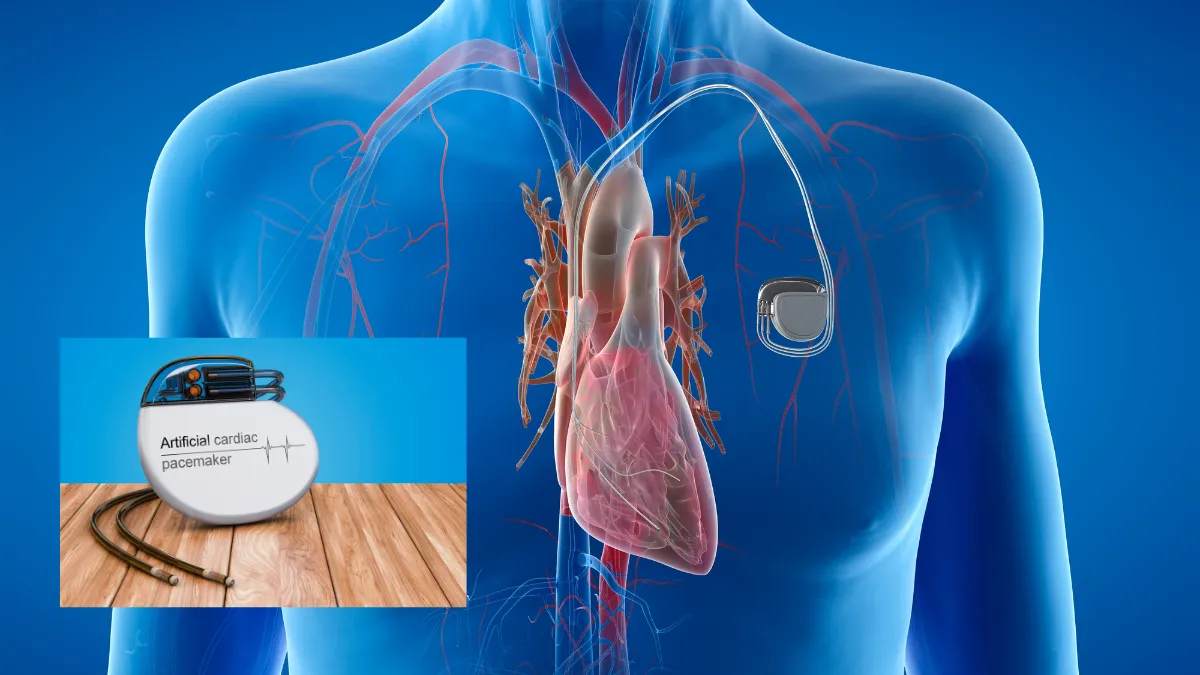
A conventional pacemaker has two main components, a small metal generator about the size of a matchbox, implanted just under the skin in the upper chest, and one or more thin, insulated wires called leads that thread through a vein into the heart. The generator monitors the heart’s rhythm continuously and delivers an electrical impulse through the leads whenever the rate drops below the programmed threshold.
This technology has been refined over decades and is highly reliable, millions of people around the world live full, active lives with conventional pacemakers and never experience any issue with their leads. For the vast majority, a lead-based pacemaker performs exactly as intended for its entire lifespan. The search for leadless technology is not driven by a failure of conventional devices, it is driven by the ambition to do even better, and to eliminate a small but real source of potential complications for future patients.
What is a leadless pacemaker?
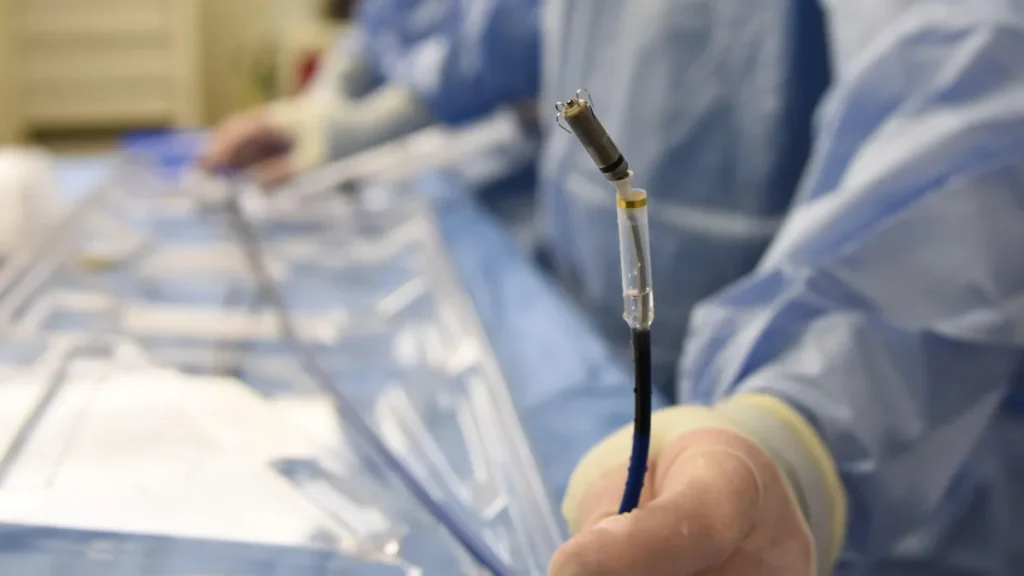
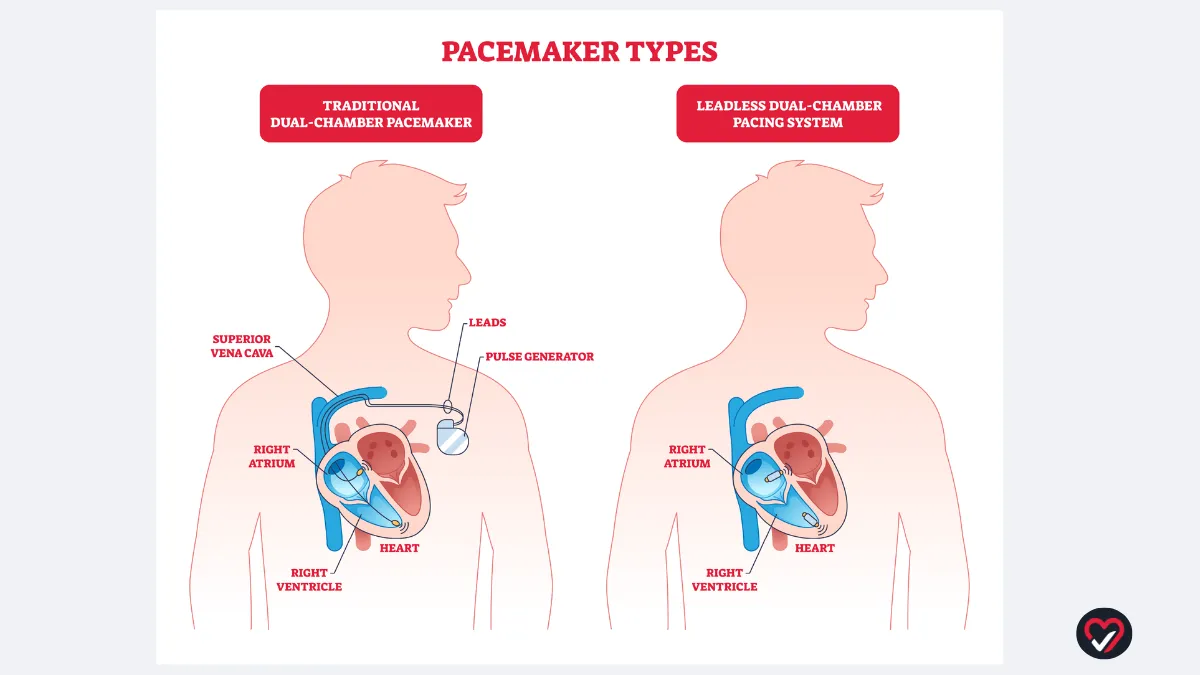
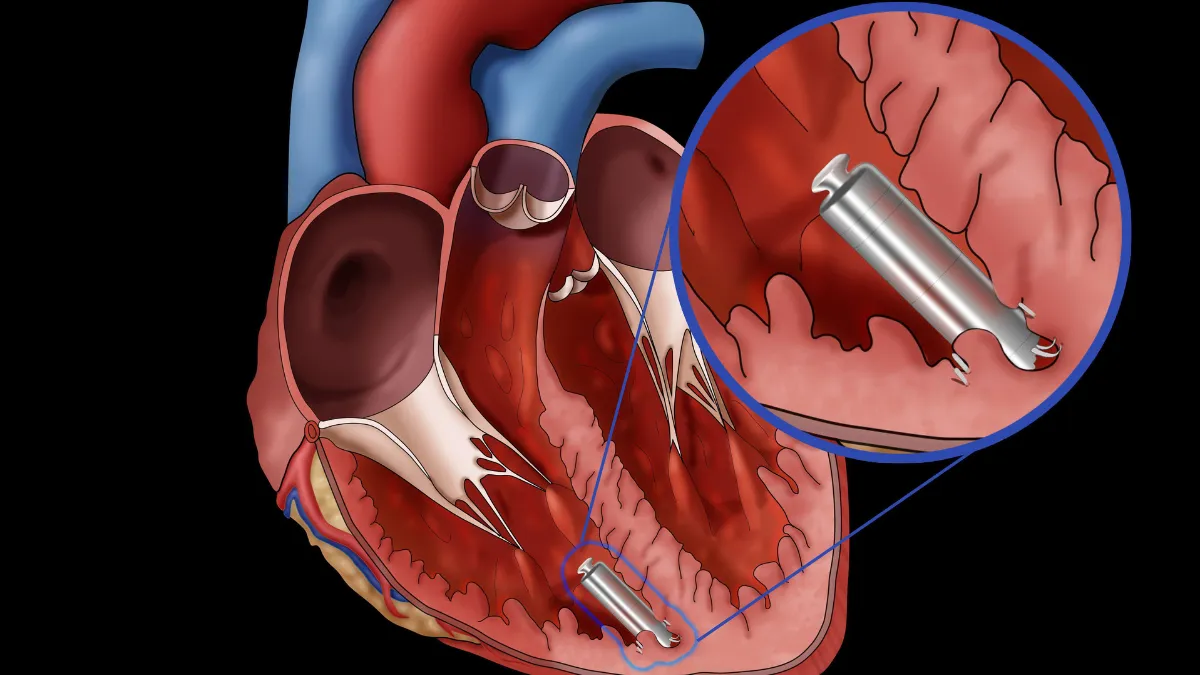
A leadless pacemaker is a self-contained device, no generator in the chest, no wires threading through the veins. Instead, the entire device sits inside the heart itself, anchored directly to the heart muscle. It is implanted through a catheter, a thin flexible tube introduced through a vein in the groin, in a procedure that typically takes under an hour and does not require a general anaesthetic.
The device is remarkable in scale. Current leadless pacemakers are roughly the size of a large vitamin capsule, about one tenth the size of a conventional pacemaker generator. Once in place, there is no visible lump under the skin, no scar on the chest wall, and no restriction on arm movement. For carefully selected patients, particularly those who are active or self-conscious about the appearance of a conventional device, this can be meaningful.
Who has been able to use leadless pacemakers, until now?
For most of their history, leadless pacemakers could only pace one chamber of the heart, the lower right chamber, or right ventricle. This made them suitable for a specific group of patients, primarily those with atrial fibrillation and a slow ventricular rate, where coordinating the upper and lower chambers is less critical because the upper chambers are already beating chaotically.
This group represents around one in five people who need a pacemaker. The majority, those with a slow heart rate in normal rhythm, or with heart block where the upper and lower chambers need to stay in sync, could not benefit from leadless technology and still required a conventional device with leads.
Leadless pacing has always been an exciting concept, but until recently it was an option for a minority of patients. The ability to pace both chambers of the heart wirelessly is a meaningful step forward, though the technology is still maturing and not yet widely available at all centres.
The breakthrough, dual-chamber leadless pacing
The most significant development in pacemaker technology in recent years is the arrival of a system that can pace both the upper and lower chambers of the heart without any wires connecting them. Instead of a physical lead, two separate miniature devices, one in the right atrium and one in the right ventricle, communicate wirelessly with each other on every single heartbeat, maintaining the coordinated timing that the heart needs to pump efficiently.
This system has received regulatory approval in both the United States and Europe, and is being implanted at a growing number of specialist centres worldwide. It is important to note that this technology is not yet universally available, and eligibility depends on individual patient factors that your cardiologist will assess carefully.
fewer overall complications at six months with dual-chamber leadless pacing compared to traditional pacemakers in early clinical studies
Source: Steinwender et al., NEJM Evidence, 2024
What are the advantages of leadless pacing?
| Potential advantage | What it may mean for patients |
|---|---|
| No leads | Removes the most common source of long-term complications, lead fracture, displacement, and infection, though longer-term data is still accumulating |
| No chest incision | No visible scar, no lump under the skin, no restriction on arm or shoulder movement |
| Minimally invasive | Shorter procedure, faster recovery, and typically a shorter hospital stay than conventional implantation |
| Long battery life | Designed to last over a decade, comparable to conventional devices, though real-world longevity data is still emerging |
| Retrievable | The device can potentially be retrieved and replaced at end of battery life, though this depends on individual circumstances |
| Upgradeable | It may be possible to start with one device and add the second later if clinical needs change, subject to suitability assessment |
Are there any limitations?
Leadless pacemakers are not suitable for everyone. People with certain mechanical heart valves, existing pacing hardware already in place, or some anatomical considerations may not be candidates. The procedure also has a learning curve, outcomes improve significantly as operators accumulate experience, and it is best performed at centres with established expertise in the technique.
Cost is also a consideration. Leadless devices are currently more expensive than conventional pacemakers, which may affect availability and access depending on your healthcare system. This is expected to improve as the technology becomes more widely adopted.
Longer-term data on leadless pacemakers is also still accumulating. Conventional pacemakers have decades of real-world evidence behind them. Leadless technology, while promising, does not yet have that same depth of long-term follow-up data, something your cardiologist will factor into any recommendation.
There are also some patients who require more complex pacing, for example, those who also need a defibrillator function, for whom conventional systems remain the appropriate choice. Your electrophysiologist will assess your specific situation carefully before recommending one approach over another.
What does this mean if you are being considered for a pacemaker?
If you have been told you may need a pacemaker, the most important thing is to have a thorough conversation with your cardiologist or electrophysiologist about all available options. Conventional pacemakers remain the proven standard of care for most patients, they are highly reliable, well understood, and backed by decades of evidence. Leadless technology is a promising development, but whether it is appropriate for you depends on your specific heart rhythm problem, your anatomy, and whether your centre has the experience to offer it safely.
Questions worth raising at that appointment are below.
Questions to ask your cardiologist
Questions worth asking
- Given my specific heart rhythm problem, am I a candidate for a leadless pacemaker or does my situation require a conventional device with leads?
- Does this centre have experience with leadless pacemaker implantation, and how many procedures has the team performed?
- Would I need pacing in one chamber or both, and does that affect which type of device is most suitable?
- What are the battery life expectations for the device being recommended, and what happens when the battery needs replacing?
- Are there any lifestyle restrictions after implantation, and do these differ between conventional and leadless devices?
Conclusion
Leadless pacemakers herald an exciting shift in cardiac rhythm management. At present, conventional lead-based devices remain the standard of care for the vast majority of patients, backed by decades of evidence and an excellent long-term safety record. As the technology matures, increasing scientific rigour through clinical trials will no doubt expand the indications for leadless pacing and drive broader adoption in the years ahead.
Free Resources
Our Heart Glossary explains terms like bradycardia, heart block, atrial fibrillation, electrophysiologist, and catheter in plain language.