Key Points
- A blood clot inside a vein, known as a deep vein thrombosis (DVT) or pulmonary embolism (PE) is a serious but very treatable condition. Anticoagulation is the cornerstone of treatment.
- Anticoagulants do not dissolve existing clots, they prevent the clot from growing and give the body time to break it down naturally through its own healing processes.
- DOACs (direct oral anticoagulants) apixaban, rivaroxaban, dabigatran, and edoxaban, are now the preferred treatment for most patients with DVT and PE, replacing warfarin as the standard of care.
- The duration of anticoagulation is one of the most important decisions in managing blood clots, ranging from three months to lifelong treatment depending on the cause, location, and individual risk factors.
- Finding an underlying cause for the clot is a critical part of the initial assessment, particularly in younger patients, those with recurrent clots, or those with a strong family history.
- Anticoagulation significantly reduces the risk of a further clotting event, but carries a bleeding risk that must always be balanced against the risk of stopping treatment too early.
Being told you have a blood clot can be frightening. The diagnosis, whether a deep vein thrombosis in the leg, a pulmonary embolism in the lungs, or a clot elsewhere in the body, raises immediate questions: How serious is this? What happens now? How long will I need treatment? Could it happen again?
As a haematologist, these are questions I work through with patients every day. This article aims to give you a clear, honest understanding of how blood clots are treated, why anticoagulants are used, and what the key decisions in management look like, so that your conversations with your treating team are as informed and productive as possible.
What Is a Blood Clot and Why Does It Form?
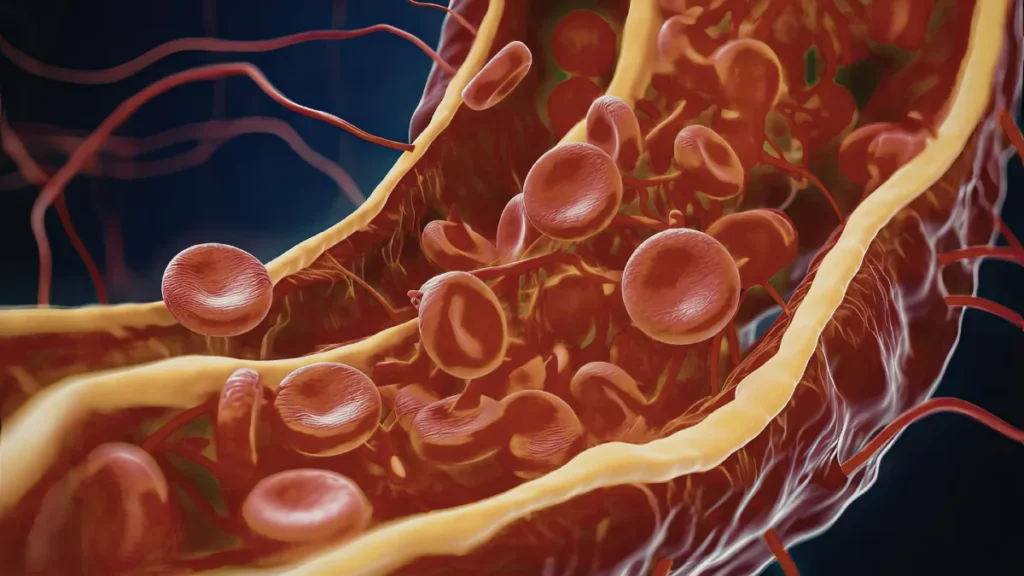
The blood’s ability to clot is an essential survival mechanism, without it, even a small injury could cause uncontrolled bleeding. The clotting process involves a complex cascade of proteins that work together to form a stable clot at the site of injury.
Problems arise when this system activates inappropriately, forming clots inside blood vessels where they are not needed. This tends to occur when three conditions coincide, described by Virchow’s Triad:
| Factor | What It Means | Common Examples |
|---|---|---|
| Sluggish blood flow | Blood pooling or moving too slowly through vessels | Long-haul flights, prolonged bed rest, immobility after surgery, heart failure |
| Vessel wall injury | Damage to the lining of a blood vessel | Surgery, trauma, inflammation, cancer, central venous catheters |
| Increased clotting tendency | The blood is more prone to clotting than normal | Inherited clotting disorders, cancer, pregnancy, oestrogen-containing contraceptives, antiphospholipid syndrome |
Understanding which of these factors contributed to your clot is important, not just for treatment planning, but for assessing the risk of recurrence and deciding how long anticoagulation should continue.
DVT and Pulmonary Embolism, Understanding the Spectrum
A deep vein thrombosis (DVT) is a clot that forms in a deep vein, most commonly in the calf, thigh, or pelvis. Symptoms typically include swelling, warmth, redness, and pain in the affected leg, though DVT can occasionally be present without obvious symptoms.
If a portion of the clot breaks off and travels through the circulation to the lungs, it becomes a pulmonary embolism (PE). Symptoms include sudden breathlessness, chest pain, often sharp and worse on breathing, a rapid heart rate, and sometimes light-headedness or collapse. A large PE is a medical emergency. Smaller PEs may cause milder symptoms that build gradually.
DVT and PE are collectively referred to as venous thromboembolism (VTE) they represent different points on the same spectrum and are managed with the same class of treatment: anticoagulation.
Anticoagulants do not dissolve a blood clot that has already formed, this is one of the most important things to understand about treatment. What they do is prevent the clot from enlarging, reduce the risk of further clots forming, and buy the body time to break down the existing clot through its own natural processes. Most clots do resolve over weeks to months with appropriate anticoagulation.
How Are Blood Clots Treated?
The mainstay of treatment for DVT and PE is anticoagulation. For most patients, this means starting a DOAC (direct oral anticoagulant) promptly, often the same day as diagnosis. The rapid onset of action of these medicines means effective anticoagulation can be established within hours.
In some situations, particularly in hospital for a large or haemodynamically significant PE, initial treatment with injectable heparin (either unfractionated heparin or low molecular weight heparin such as enoxaparin) may be used before transitioning to an oral agent.
For the most severe cases of PE, where the clot is causing significant haemodynamic compromise, meaning the heart and circulation are under serious strain, a treatment called thrombolysis may be considered. This uses a powerful clot-dissolving drug to break down the clot rapidly. It carries a significant bleeding risk and is reserved for situations where the benefit clearly outweighs that risk.
DOACs, The Current Standard of Care for VTE
Over the past decade, DOACs have largely replaced warfarin as the preferred treatment for DVT and PE in patients without specific contraindications. The reasons are compelling: they are at least as effective as warfarin, cause significantly less serious bleeding in clinical trials, require no routine blood monitoring, and are taken as a fixed dose without dietary restrictions.
| Drug | Brand Name | VTE Dosing, Typical Regimen | Notes |
|---|---|---|---|
| Apixaban | Eliquis | 10mg twice daily for 7 days, then 5mg twice daily | Can be started immediately; lowest kidney dependence |
| Rivaroxaban | Xarelto | 15mg twice daily for 21 days, then 20mg once daily | Take with food for best absorption; once daily after initial phase |
| Dabigatran | Pradaxa | 150mg twice daily after initial 5–10 days of heparin | Requires initial heparin treatment before switching |
| Edoxaban | Lixiana, Savaysa | 60mg once daily after initial 5–10 days of heparin | Requires initial heparin treatment before switching |
For patients who cannot take DOACs, including those with mechanical heart valves, significant kidney disease, or antiphospholipid syndrome with high-risk features, warfarin remains an important and effective option. For a detailed comparison of warfarin and DOACs, see our dedicated article: Warfarin vs NOACs: Which Blood Thinner Is Right for You?
How Long Does Treatment Last?
This is one of the most important, and sometimes most difficult, questions in managing blood clots. The answer is genuinely individual and depends on several factors.
| Clinical Situation | Typical Duration | Rationale |
|---|---|---|
| Provoked DVT or PE clot related to a clear temporary risk factor (surgery, trauma, hospitalisation, flight) | 3 months | Once the provoking factor has resolved, the ongoing clot risk returns to baseline. Stopping at 3 months is appropriate for most |
| Unprovoked DVT or PE no clear precipitating cause identified | At least 3–6 months, often extended or indefinite | Higher recurrence risk without an identifiable and reversible trigger. Extended treatment decision based on bleeding vs clot risk balance |
| Cancer-associated VTE | Ongoing, typically for as long as cancer is active | Cancer significantly raises the clotting tendency. Low molecular weight heparin or certain DOACs preferred |
| Recurrent VTE | Indefinite anticoagulation generally recommended | Second clot substantially increases the likelihood of further events, ongoing protection outweighs bleeding risk for most |
| Inherited thrombophilia (e.g. antiphospholipid syndrome, protein C/S deficiency) | Often indefinite, determined by thrombophilia type and severity | Underlying genetic tendency to clot persists regardless of provoking factors |
The decision to stop anticoagulation is never taken lightly, the risk of a further clotting event must always be weighed against the ongoing bleeding risk of continued treatment. This is a conversation your haematologist or treating doctor will have with you carefully, taking your full medical history and personal circumstances into account.
Investigating the Cause, Thrombophilia Testing
After a blood clot, particularly an unprovoked one, a clot in an unusual site, a clot in a younger patient, or recurrent clotting, investigating for an underlying cause is an important part of management.
This may include testing for inherited thrombophilias genetic conditions that increase the blood’s tendency to clot. Common ones include Factor V Leiden mutation, prothrombin gene mutation and deficiencies of the natural anticoagulant proteins protein C protein S and antithrombin.
Testing for antiphospholipid syndrome an acquired autoimmune condition causing increased clotting tendency, is also routinely considered, particularly in younger patients and those with recurrent events or pregnancy-related complications.
Importantly, many thrombophilia tests are affected by anticoagulant treatment itself, so timing of testing requires careful planning, often deferred until anticoagulation has been completed, or interpreted with this in mind. Your haematologist will guide the appropriate approach for your situation.
In older patients presenting with an unprovoked clot, screening for underlying malignancy is also considered, as cancer is one of the most important acquired causes of a clotting tendency and can occasionally present this way before other symptoms appear.
Compression Stockings and DVT
For patients with a DVT affecting the leg, compression stockings are frequently recommended alongside anticoagulation. They help reduce swelling, improve venous return, and may reduce the risk of a long-term complication called post-thrombotic syndrome a condition of chronic leg swelling, heaviness, and discomfort that can develop if the deep veins are damaged by a clot and do not recover fully.
Graduated compression stockings, typically knee-high, with a pressure of 30–40 mmHg, are the standard recommendation for most patients with proximal DVT. Your doctor or vascular team will advise on the appropriate class and duration of use.
Living With Anticoagulation, Practical Guidance
Day-to-Day Guidance for Patients on Anticoagulants for VTE
- Take your medicine consistently anticoagulants must be taken every day at roughly the same time. Missing doses reduces protection against further clots. Do not double-dose if you miss one, take the next dose as scheduled and inform your doctor.
- Tell all healthcare providers dentists, surgeons, GPs, and emergency doctors all need to know you are on an anticoagulant before any procedure or new prescription.
- NSAIDs and anticoagulants do not mix well ibuprofen, naproxen, and other anti-inflammatory pain medicines significantly increase bleeding risk. Use paracetamol unless your doctor advises otherwise.
- Stay active immobility is itself a risk factor for further clots. Regular walking and staying hydrated, particularly on long journeys, are simple but genuinely effective preventive steps.
- Know the bleeding warning signs unusual bruising, blood in urine or stools, prolonged bleeding from cuts, or sudden severe headache should be reported promptly. Seek emergency care for severe or sudden symptoms.
- Do not stop without discussion even if you feel completely well, stopping anticoagulation early increases the risk of the clot recurring or extending. Always discuss timing of cessation with your treating doctor.
- Pregnancy and anticoagulation if you are on anticoagulation and become pregnant, or are planning to, inform your haematologist immediately. DOACs are not safe in pregnancy, low molecular weight heparin is the standard treatment and requires specialist oversight throughout.
Conclusion
A blood clot diagnosis is understandably alarming, but with prompt treatment and appropriate anticoagulation, the vast majority of patients recover fully and go on to live completely normal lives. The medicines available today are more effective, more convenient, and safer than those of even a decade ago.
The key decisions in managing blood clots, which anticoagulant, for how long, whether to investigate further, are individual ones that depend on your specific circumstances. Working with your treating team, asking questions, and understanding your treatment are all part of managing this well.
If you have concerns about your anticoagulation, side effects, duration, the risk of recurrence, or what to expect going forward, your haematologist, cardiologist, or GP is always the right person to ask. These are exactly the conversations that lead to better-informed, more confident care.