Key Points
- Hypertrophic cardiomyopathy (HCM) is one of the most common inherited heart conditions, caused by a genetic mutation that makes the heart muscle thicken abnormally
- In many patients, HCM is well managed with medication, but for others, symptoms persist and more invasive treatment has historically been the only option
- Mavacamten works differently from most heart medications, it targets the heart muscle directly, reducing the obstruction that drives symptoms in HCM
- In a major clinical trial, 37% of patients on Mavacamten showed significant improvement in symptoms and exercise capacity, compared to 17% on placebo
- Mavacamten has been approved by the FDA and the Australian Therapeutic Goods Administration for eligible patients with symptomatic obstructive HCM
- Regular echocardiograms are essential during treatment, your cardiologist will monitor your heart function closely and adjust the dose as needed
One of the more common inherited heart conditions I see in my practice is hypertrophic cardiomyopathy, HCM. For many patients, medications manage it well. For others, symptoms persist despite treatment, and that has historically meant considering more invasive options, including open heart surgery. The arrival of a new medication called Mavacamten has changed that conversation considerably, and I think it is worth understanding why.
What Is Hypertrophic Cardiomyopathy?
Most people who receive a diagnosis of HCM have never heard of it before, which is understandable, because despite being one of the most common genetic heart conditions, it rarely makes headlines.
In HCM, the heart muscle, particularly the wall of the left ventricle, thickens abnormally. This makes the muscle stiffer and less able to relax properly between beats, affecting how efficiently the heart fills and pumps. In some patients, the thickening also narrows the outflow tract, the channel through which blood leaves the heart, creating an obstruction that drives many of the symptoms.
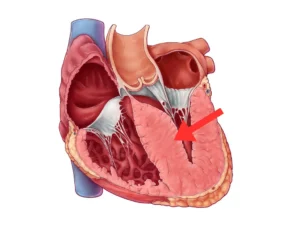
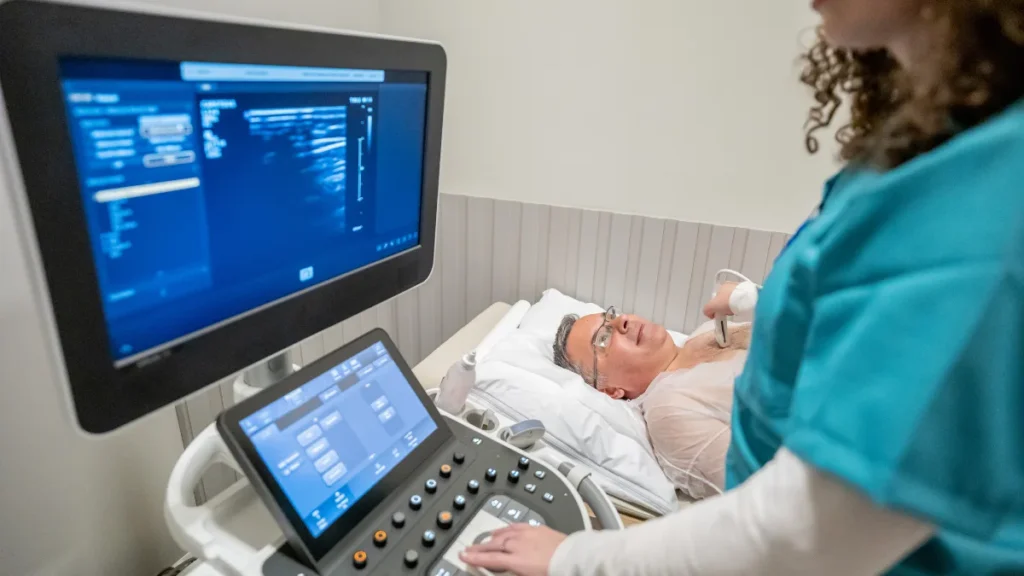
HCM is caused by genetic mutations affecting proteins in the heart muscle cells. It can develop at any age and runs in families, so if you have been diagnosed, it is worth your close relatives being assessed too. Diagnosis typically involves an echocardiogram, cardiac MRI, ECG, and a detailed family history. Genetic testing can help identify who else in the family may be at risk.
Symptoms vary widely. Some people have none at all. Others experience breathlessness, chest discomfort, fatigue, dizziness, palpitations or fainting, particularly with exertion. Many live full, active lives with the right management in place.
HCM is one of those conditions where the diagnosis can feel alarming, but with the right management, most people do very well. The goal is always to understand your individual situation and tailor treatment accordingly.
How Mavacamten Works
Most heart medications work indirectly, managing blood pressure, heart rate, or electrical rhythm. Mavacamten is different. It works directly on the heart muscle itself.
Specifically, it is a small molecule inhibitor of cardiac myosin, the protein responsible for generating the force of each heartbeat. By modulating myosin activity, Mavacamten reduces the excessive contraction that characterises obstructive HCM, easing the pressure gradient across the outflow tract and allowing the heart to work more efficiently.
This is a genuinely new mechanism of action, and that is what makes it significant for patients who have not responded adequately to existing treatments.
What the Evidence Shows
The pivotal clinical trial, the EXPLORER-HCM study, published in The Lancet in 2020, enrolled 251 patients with symptomatic obstructive HCM. Participants received either Mavacamten or placebo for 30 weeks.
The results were meaningful. By the end of the study, a significantly greater proportion of patients treated with Mavacamten showed improvement in both exercise capacity and symptoms, and the pressure gradient across the outflow tract was substantially reduced, with a good safety profile throughout.
of patients on Mavacamten improved significantly in exercise capacity and symptoms
vs 17% on placebo, EXPLORER-HCM trial, The Lancet 2020
On the basis of this evidence, Mavacamten has been approved by the FDA in the United States and, more recently, by the Therapeutic Goods Administration here in Australia, under the brand name Camzyos.
Dosing and What to Expect
Mavacamten is taken once daily as a capsule. Doses range from 2.5mg to 15mg depending on your individual response. Your cardiologist will start at a lower dose and adjust gradually, this is not a medication where you start at the full dose from day one.
The titration process is guided by regular echocardiograms, which allow your team to see exactly how your heart is responding and whether any dose adjustment is needed. This monitoring is an essential part of treatment, not an optional extra.
Important Safety Considerations
Because Mavacamten reduces the force of heart muscle contraction, which is exactly what makes it effective, it also requires careful monitoring. In some patients, particularly those who develop intercurrent illness or an arrhythmia during treatment, there is a risk of heart function declining.

It is also important to tell your cardiologist and pharmacist about all other medications you are taking. Some drugs can affect how Mavacamten is metabolised in the body, which can alter its effect, so a full medication review before starting is important.
Conclusion
Mavacamten represents a genuinely new chapter in how we manage hypertrophic cardiomyopathy. For patients who have struggled with symptoms despite conventional treatment, it offers a meaningful alternative to more invasive procedures, and that is a significant step forward.
That said, it is not the right choice for everyone. The decision to use it should always be made carefully, in full consultation with a cardiologist who knows your complete clinical picture. If you have HCM and your symptoms are not well controlled, it is absolutely worth raising Mavacamten at your next appointment.
As always, the most important conversation is the one between you and your doctor.
When in Doubt
If you have HCM and your symptoms are not well controlled, please speak to your cardiologist.
New treatment options like Mavacamten are worth a conversation. You don’t need to simply accept persistent symptoms, there may be more that can be done. Learn more about knowing when to seek help →
More from Heart Matters
References
- Olivotto I, et al. Mavacamten for treatment of symptomatic obstructive hypertrophic cardiomyopathy (EXPLORER-HCM): a randomised, double-blind, placebo-controlled, phase 3 trial. The Lancet. 2020;396(10253):759-769. doi: 10.1016/S0140-6736(20)31859-1.