Key Points
- Supraventricular tachycardia (SVT) is a common heart rhythm condition causing sudden episodes of very rapid heartbeat, distressing but rarely dangerous in an otherwise healthy heart.
- Until recently, managing an acute SVT episode outside hospital meant either waiting it out, trying breathing techniques, or calling an ambulance.
- A nasal spray called Cardamyst (etripamil) has now received FDA approval, the first self-administered treatment that can stop an SVT episode at home, without a trip to the emergency department.
- In clinical trials, nearly 60% of patients converted back to normal rhythm within 30 minutes of using the spray, with a median conversion time of around 18 minutes.
- Cardamyst is a prescription medication, speak with your cardiologist or electrophysiologist about whether it is appropriate for you.
If you have ever had an episode of SVT, you know exactly how it feels. One moment everything is normal; the next, your heart is racing at 150 or even 200 beats per minute, seemingly out of nowhere. The chest flutter, the breathlessness, the racing pulse that will not settle, and the anxiety of not knowing when or how it will stop.
For most people with SVT, the condition is not life-threatening. But that knowledge offers little comfort in the middle of an episode. And for years, the options for managing an acute attack outside a hospital setting have been limited, breathing techniques that sometimes work, waiting it out, or calling emergency services if the episode drags on.
That has now changed. A new treatment approved in late 2025 gives people with SVT something they have never had before, a prescription nasal spray they can use themselves, at home, to stop an episode when it starts.
What is SVT?
The heart has its own electrical system, a network of pathways that coordinate each heartbeat. In SVT, an abnormal electrical circuit in the upper chambers of the heart fires off a rapid series of signals, driving the heart rate to speeds that are far beyond what exercise or emotion would normally produce. Heart rates of 150 to 200 beats per minute during an episode are not unusual.
Episodes can begin and end abruptly. They may last seconds or stretch to minutes or even longer. SVT can strike at rest, during exercise, or apparently without any trigger at all, though caffeine, alcohol, stress, and fatigue are commonly reported precipitants.
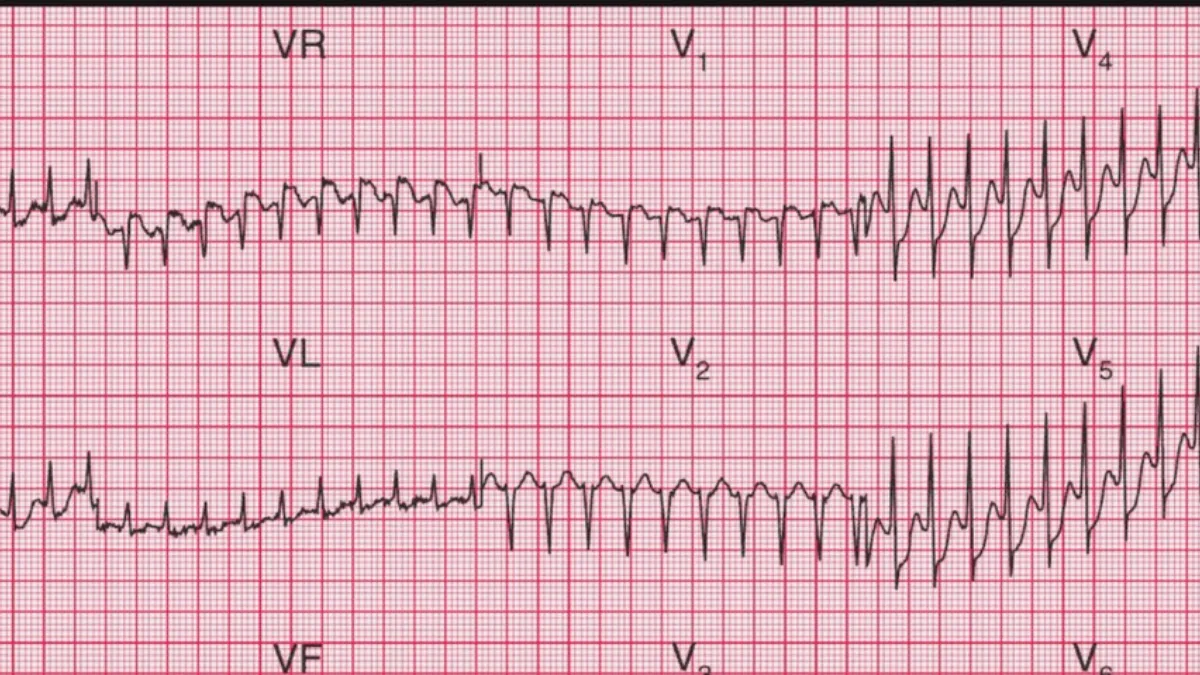
SVT affects people across all age groups and is more common than many people realise. It is diagnosed using an ECG recorded during an episode, or picked up on a Holter monitor if episodes are frequent enough to be captured. The good news is that in a structurally normal heart, SVT is almost never dangerous, though it is frequently frightening and disruptive.
How has SVT been managed until now?
The first line of response for many people is a vagal manoeuvre, a technique that stimulates the vagus nerve and can sometimes interrupt the abnormal circuit driving the fast rhythm. The most evidence-based approach is the modified Valsalva manoeuvre, which involves straining as if bearing down and then lying back with legs raised. It works reasonably well for some people some of the time, but by no means always.
When vagal manoeuvres fail and an episode does not settle, the conventional response has been to call for medical help. In the ambulance or emergency department, an intravenous medication called adenosine is usually administered, it works rapidly and effectively but requires a cannula, cardiac monitoring, and a clinical setting. For people with frequent episodes, the cycle of episodes, emergency department visits, and recovery is exhausting and disruptive to daily life.
Longer-term, people with frequent or severely symptomatic SVT may be offered daily medications to reduce episode frequency, or a procedure called catheter ablation that can permanently disrupt the abnormal electrical pathway. Ablation has excellent success rates and is curative in most cases, our dedicated SVT article covers this in more detail.
Step 1, At Home
Vagal Manoeuvres
Bearing down (modified Valsalva) or cold water on the face stimulates the vagus nerve and can interrupt the SVT circuit. Works for some people, some of the time.
Step 2, New Option
Cardamyst Nasal Spray
Self-administered at home at the onset of an episode. FDA approved December 2025. Converts SVT to normal rhythm in approximately 18 minutes in most patients.
Step 3, Emergency
Adenosine (IV)
Administered intravenously in the ambulance or emergency department. Highly effective but requires clinical monitoring and a cannula.
Long Term, Prevention
Daily Medication
Beta-blockers or calcium channel blockers taken daily to reduce the frequency of SVT episodes. Not curative but can significantly reduce burden.
Long Term, Curative
Catheter Ablation
A minimally invasive procedure that permanently disrupts the abnormal electrical pathway causing SVT. Highly effective with excellent long-term success rates.
Always Helpful
Lifestyle Measures
Staying well hydrated, limiting caffeine and alcohol, avoiding smoking and recreational drugs, and managing stress and sleep can all reduce episode frequency.
The new nasal spray, what is it and how does it work?
Cardamyst, the brand name for etripamil, is a calcium channel blocker delivered as a nasal spray. It works by slowing conduction through the AV node, the electrical junction between the upper and lower chambers of the heart, which interrupts the abnormal circuit driving the SVT and allows the heart to reset to a normal rhythm.
What makes it different from existing treatments is how and where it can be used. Cardamyst is designed to be self-administered, by the patient, at the moment an episode begins, wherever they are. No hospital visit, no intravenous line, no waiting for an ambulance. Two sprays into the nostril, absorbed rapidly through the nasal lining, with an onset of action within minutes.
median time to conversion back to normal rhythm with Cardamyst in clinical trials, compared to 54 minutes with placebo
What did the clinical trials show?
The evidence behind Cardamyst comes from a programme of clinical trials involving more than 1,800 patients and over 2,000 SVT episodes. The pivotal trial showed that nearly 60% of patients using the nasal spray converted back to normal rhythm within 30 minutes, compared to around 30% of those using a placebo spray. The median time to conversion was approximately 18 minutes with Cardamyst, compared to 54 minutes with placebo.
Importantly, the data also showed a meaningful reduction in emergency department visits, patients using Cardamyst were around 39% less likely to end up needing emergency care for their ongoing episode compared to those using placebo. For people whose SVT has previously meant repeated trips to hospital, that is a significant change in how the condition can be lived with.
If the first dose does not work within ten minutes, a second dose can be administered. The most common side effects were mild and local, nasal discomfort, congestion, and occasional nosebleed, and fewer than 2% of participants stopped using it due to side effects.
Who is it suitable for, and who should be cautious?
Cardamyst is a prescription medication, and not everyone with SVT will be a candidate. People with certain underlying heart conditions, including heart failure, Wolff-Parkinson-White syndrome, or other specific rhythm disorders, should not use it. It should be administered while seated, as it can occasionally cause dizziness.
It is also worth being clear that Cardamyst is an on-demand treatment for acute episodes, it does not prevent SVT from occurring, and it is not a replacement for ablation in people who are suitable candidates and want a more permanent solution. It is best thought of as an empowering additional tool, something that gives patients control over their episodes in the moment, while longer-term management is planned in partnership with their cardiologist.
Longer-term, people with frequent or severely symptomatic SVT may be offered daily medications to reduce episode frequency, or a procedure called catheter ablation that can permanently disrupt the abnormal electrical pathway. Ablation has excellent success rates and is curative in most cases.
For many people, SVT is not just a medical condition, it is a source of ongoing anxiety. The unpredictability of episodes, the fear of being in a situation where help is not easily available, the disruption to work, exercise, and social life, these are real and underappreciated dimensions of what it means to live with this condition.
A self-administered treatment that can terminate an episode at home is genuinely meaningful for this group. The knowledge that you have something effective in your pocket, that you do not have to wait and hope, or call an ambulance, changes the psychological relationship with the condition, not just the physiological one.
Cardamyst received FDA approval in December 2025 and was expected to become available in pharmacies in the United States in early 2026. Regulatory review in other regions including Australia and Europe is ongoing. If you have SVT and want to know whether this treatment might be appropriate for you, the conversation to have is with your cardiologist or electrophysiologist.
Questions to Ask Your Cardiologist
Questions worth asking
- Given my pattern of SVT episodes, frequency, duration, and how they respond to vagal manoeuvres, am I a suitable candidate for a self-administered nasal spray treatment?
- Is catheter ablation something I should be considering alongside or instead of on-demand medication?
- Are there any aspects of my medical history or other medications that would make Cardamyst unsuitable for me?
- What should I do if I use the nasal spray and my episode does not convert within 30 minutes?
- Should I still call emergency services in certain situations even if I have the nasal spray available?
Conclusion
SVT has long been one of those conditions that sits in an awkward space, disruptive and frightening enough to significantly affect quality of life, but often not serious enough to be prioritised in the way that more immediately dangerous rhythm disorders are. People with frequent episodes have sometimes felt that their options were limited to either tolerating the condition or undergoing a procedure.
The approval of a self-administered nasal spray that can terminate an acute episode changes that picture meaningfully. It does not cure SVT, and it is not right for everyone, but for the right patients, it offers something genuinely new: control, at the moment it is most needed.
If you have SVT and have been managing episodes by waiting them out or heading to the emergency department, this is a development worth discussing with your cardiologist.
Free Resources
Our Heart Glossary explains terms like SVT, AV node, catheter ablation, vagal manoeuvre, and calcium channel blocker in plain language.