Key Points
- Microplastics and nanoplastics, tiny plastic fragments from our environment, have been found inside cholesterol plaques in the arteries of some people.
- A landmark 2024 study in the New England Journal of Medicine found that people with plastics detected in their arterial plaques had a higher rate of heart attack, stroke, and death over the following years.
- This is an early but significant finding, it does not mean plastics will definitely cause a cardiovascular event, but it adds to the growing case that plastic pollution has consequences for human health beyond the environment.
- The main sources of exposure are contaminated food and water, air, and everyday plastic-containing products.
- Practical steps to reduce exposure are available and worth taking, particularly around food storage and packaging.
Most of us are aware that plastic pollution is an environmental problem. What is less well known is that tiny plastic particles, so small they are invisible to the naked eye, have been found inside the human body, including within the walls of our arteries.
A major study published in 2024 brought this issue into sharp focus, finding a connection between these particles and cardiovascular outcomes. It is a finding worth understanding, not to cause alarm, but because it adds an important dimension to how we think about heart health and the world we live in.
What are microplastics and nanoplastics?
As plastics degrade in the environment, broken down by sunlight, heat, and mechanical wear, they fragment into progressively smaller pieces. Microplastics are particles smaller than five millimetres. Nanoplastics are even smaller, measuring less than one thousandth of a millimetre. Both are now found widely in soil, water, air, and food.
These particles enter the human body primarily through what we eat and drink, through the air we breathe, and through contact with plastic-containing products. Once inside the body, they can travel through the bloodstream and, as this research shows, accumulate in unexpected places, including inside arterial plaques.
What is a carotid plaque?
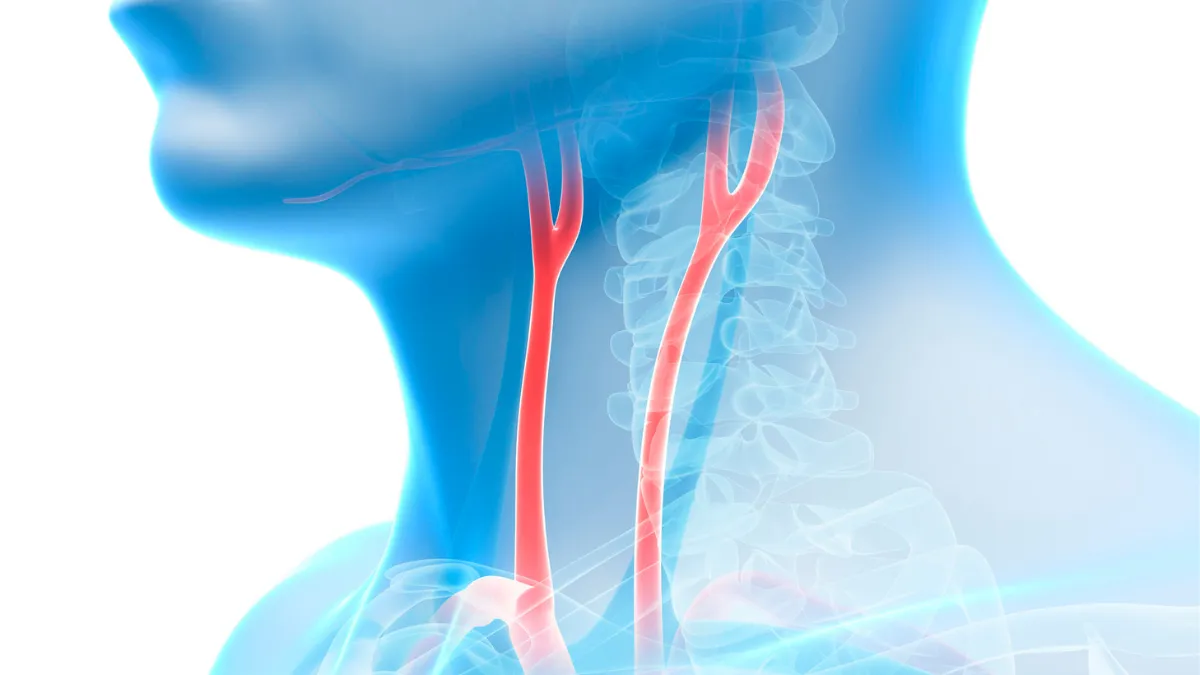
The carotid arteries are the two large blood vessels that run up either side of the neck, supplying blood to the brain. Like the coronary arteries of the heart, they can develop atherosclerosis, a gradual buildup of cholesterol, fat, calcium, and other material inside the artery wall, forming what is known as a plaque.
Over time, these plaques can narrow the artery, reducing blood flow to the brain. If a piece of plaque breaks away and blocks a smaller vessel, it can cause a stroke. Managing carotid artery disease, through medication, lifestyle, and in some cases surgery, is an important part of stroke prevention.
What did the study find?
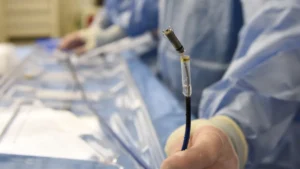
The study, published in the New England Journal of Medicine in March 2024, examined 312 patients who were undergoing a surgical procedure called carotid endarterectomy, an operation to remove plaque buildup from the carotid arteries. The researchers analysed the removed plaque samples to see whether microplastics or nanoplastics were present.
of patients had detectable microplastics or nanoplastics within their carotid artery plaque
The researchers then followed these patients over time, tracking rates of heart attack, stroke, and death. Those with plastics detected in their plaque had a rate of these events that was approximately twice as high as those without detectable plastics.
This is the kind of finding that makes you pause. We are still learning what it means, but the fact that plastics are turning up inside arterial plaque at all is a signal we need to take seriously.
Importantly, patients with detectable microplastics were also more likely to have diabetes, cardiovascular disease, elevated cholesterol, and a history of smoking, factors that independently raise cardiovascular risk. Unpicking the precise contribution of the plastics themselves from these other variables is something ongoing research will need to address.
What about carotid endarterectomy?
Carotid endarterectomy is a surgical procedure in which a vascular surgeon makes an incision in the neck to access the carotid artery and carefully removes the plaque buildup. It is considered when the artery is significantly narrowed, typically more than 70%, particularly if a person has already had symptoms such as a TIA or minor stroke.
The decision to proceed with surgery is always made on an individual basis, taking into account the degree of narrowing, the presence of symptoms, a person’s overall health, and a careful discussion between the patient, their neurologist, and vascular surgeon. It is not a decision made lightly, but for the right person, it meaningfully reduces the risk of future stroke.
How do plastics get into arterial plaque?
The pathway from plastic packaging to arterial wall involves several steps. Plastics in the environment degrade into microscopic fragments that contaminate food, drinking water, and air. These particles are ingested or inhaled, enter the bloodstream, and, because they are so small, can penetrate tissues and accumulate over time.
| Route of exposure | Common sources |
|---|---|
| Ingestion | Bottled water, seafood, food stored in plastic containers, processed foods |
| Inhalation | Indoor dust, synthetic textiles, outdoor air pollution |
| Skin contact | Plastic packaging, personal care products, synthetic clothing |
Once in the bloodstream, the particles appear able to become incorporated into the fatty material that makes up arterial plaques, and may trigger local inflammation that makes those plaques more unstable and more likely to cause events.
What can I do to reduce my exposure?
It is not possible to eliminate exposure to microplastics entirely, they are too widespread in the modern environment. But there are practical, evidence-informed steps worth taking, particularly around food and drink.
Using glass, stainless steel, or ceramic containers instead of plastic for food storage, especially for hot foods, reduces the amount of plastic that leaches into what you eat. Choosing tap water over bottled water where safe and appropriate does the same. Reducing highly processed foods, which tend to involve more plastic packaging and handling, also makes sense from a broader heart health perspective.
These are not dramatic changes, and they sit comfortably alongside everything else we know about protecting cardiovascular health. Think of them as sensible additions to an already sound approach, not a source of anxiety.
What does this mean for heart health research?
This study represents an important early chapter in understanding the cardiovascular impact of plastic pollution. As the accompanying editorial in the New England Journal of Medicine noted, the detection of microplastics within plaque tissue is itself a landmark finding, one that opens up a series of important scientific questions about mechanism, dose, and long-term effect.
Research in this area is moving quickly. What we can say now is that the cardiovascular system does not exist in isolation from the environment, and that the choices we make about plastics, both individually and collectively, may have consequences that extend well beyond ecology.
Conclusion
The detection of microplastics and nanoplastics within arterial plaque is a genuinely significant finding, one that adds a new dimension to how we understand cardiovascular risk and its relationship to the broader environment. The 2024 New England Journal of Medicine study is the most compelling evidence to date that plastic pollution is not only an ecological concern but a human health one.
What we cannot yet say with certainty is precisely how much of the increased cardiovascular risk is attributable to the plastics themselves, and how much reflects the complex mix of other risk factors present in the same patients. That question, along with the biological mechanisms by which plastics may destabilise arterial plaque, will be the focus of research in the years ahead.
What is clear is that this line of inquiry is important and moving quickly. Greater understanding of the dose, duration, and pathways of plastic exposure will help define what individual and policy-level responses are most effective. In the meantime, the most important message remains unchanged, managing the traditional cardiovascular risk factors we know make a real difference is still the single most effective thing any of us can do. Controlling blood pressure and cholesterol, not smoking, staying active, eating well, and adhering to prescribed medications all have decades of robust evidence behind them. Reducing plastic exposure is a sensible addition to that picture, not a replacement for it. Our article on understanding cardiovascular risk factors covers the fundamentals in detail.
Free Resources
Our Heart Glossary explains terms like atherosclerosis, carotid artery disease, microplastics, and stroke in plain language.