- Most coronary angiograms are now performed via the radial artery in the wrist, a much more comfortable approach than the older femoral (groin) route, with faster recovery and fewer bleeding complications.
- After the procedure, a small inflatable compression band, the TR band, is placed over the wrist puncture site for approximately 3–4 hours to allow the artery to seal safely.
- Most patients are up and moving within an hour of returning from the cath lab. Same-day discharge is common for straightforward diagnostic angiograms.
- The wrist may be sore and bruised for a few days, this is normal and expected. Avoid heavy lifting with that arm for about a week.
- Your cardiologist will discuss the results with you before you leave, this conversation is important and it is worth having someone with you to help process the information.
Having a coronary angiogram is a significant moment, and arriving on the other side of it, recovering in the ward with the procedure behind you, can feel like a relief mixed with a little uncertainty about what comes next.
The good news is that recovery from a radial artery angiogram is genuinely straightforward for most people. The wrist approach has transformed the patient experience, most people are sitting up, drinking tea, and ready to go home within a few hours. This article walks you through what to expect from the moment you return from the cath lab to your first few days at home.
What Just Happened, A Quick Recap
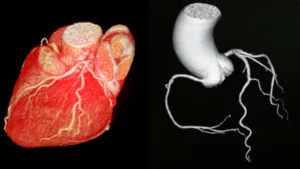
During a coronary angiogram, a thin flexible catheter is inserted into the radial artery at the wrist, threaded up through the arm and into the aorta, and positioned at the opening of each coronary artery. A contrast dye is injected and X-ray images are taken, showing the inside of the coronary arteries in detail.
The entire procedure typically takes 30 to 45 minutes. You are awake throughout, sedated and comfortable, but not under general anaesthetic. When it is over, the catheter is removed and the wrist compression band is applied. You are then transferred to a recovery area where the monitoring begins.
What to Expect, Coronary Angiogram Recovery
Immediately after
You will be moved to a recovery area. The TR band on your wrist will remain inflated. Nursing staff will check it regularly. You can eat and drink as soon as you feel ready.
TR band removal
The band is gradually deflated over 3–4 hours and then removed. Staff carefully check the site throughout this process for any signs of bleeding.
Going home
Most patients having a diagnostic angiogram go home the same day. If a stent was placed or other intervention performed, an overnight stay is more likely.
Driving
You cannot drive yourself home, arrange for someone to collect you. Most cardiologists recommend avoiding driving for 24–48 hours after an elective procedure.
Wrist care
Some bruising and soreness at the wrist is normal and expected. Avoid heavy lifting with that arm for approximately one week.
Results
Your cardiologist will discuss the findings with you before discharge. Have someone with you if possible, it helps to have a second pair of ears for this conversation.
The TR Band, What It Is and Why It Matters
The TR band (Trans-Radial band) is the small inflatable compression device placed over your wrist puncture site after the catheter is removed. It looks a little like a wide wristwatch with a clear plastic dome over the puncture site.
How it works
The band is inflated with a syringe immediately after catheter removal, applying gentle pressure directly over the puncture site to prevent bleeding while the small hole in the artery seals itself. It is not painful, occasionally it feels tight, but the pressure is carefully calibrated.
Nursing staff will check the band regularly throughout the monitoring period, gradually releasing small amounts of air, a process called patent haemostasis, to allow blood flow to continue through the artery while still preventing bleeding from the puncture site. This careful, staged deflation is the standard approach and takes approximately 3–4 hours in total.
What to watch for
While the band is in place, let the nursing staff know immediately if you notice any swelling, bleeding, or significant increase in discomfort at the wrist site. These are uncommon but important to report promptly. Once the band is removed, a small dressing is applied. Some bruising over the next few days is entirely normal.
The First Hours in Recovery
You will feel more alert than you expect
Because the angiogram is performed under sedation rather than general anaesthetic, most people feel relatively alert quite quickly after returning from the cath lab. You will be able to eat and drink as soon as you feel ready, and most people are ready fairly quickly.
You may feel a little tired from the procedure and the sedation. Some people feel relieved, some feel anxious about the results, many feel a mixture of both. All of this is entirely normal.
The results conversation
Your cardiologist will come to discuss the findings with you before you are discharged. This is one of the most important conversations of the day, and it is worth being as present and engaged as possible for it.
If you have someone with you, ask them to be there for this conversation. Two sets of ears are genuinely better than one. Write down questions in advance if you have them. And do not hesitate to ask for clarification, your cardiologist expects questions and welcomes them.
I always try to have the results conversation at the bedside before the patient leaves, not over the phone the following week. Understanding what we found and what it means is as important as the procedure itself. Come with questions. Leave with answers.
— Prof. Peter Barlis, Interventional Cardiologist
Going Home, What to Expect in the First Few Days
The wrist
Some bruising, tenderness, and swelling at the wrist puncture site is normal and expected over the first few days. The bruise may track up the forearm, this is also normal and not a cause for concern. Avoid heavy lifting, pushing, or gripping with that hand for approximately one week to allow the puncture site to heal fully.
If you notice a rapidly expanding lump at the wrist site, significant fresh bleeding through the dressing, or loss of sensation in the hand, contact the hospital or seek urgent assessment.
Activity and rest
Most people feel well enough to move around normally at home from the day of discharge. There is no need to stay in bed. Light activity, short walks, normal household tasks, is encouraged. Avoid strenuous exercise, swimming, and heavy manual work for approximately one week or as specifically advised by your team.
Medications
You may be sent home with new medications, particularly if a stent was placed or if changes to your existing treatment were made based on the results. Take all medications exactly as prescribed and do not stop any cardiac medication without discussing it with your cardiologist first.
Driving
You cannot drive yourself home on the day of the procedure, this is non-negotiable regardless of how well you feel. For an elective diagnostic angiogram, most cardiologists advise avoiding driving for 24–48 hours. If a stent was placed or if you have been prescribed new medications that may affect alertness, your team will advise specifically. Commercial or vocational licence holders have different requirements, discuss these with your cardiologist.
When to Seek Help
Most people recover smoothly and without any concerns. The following warrant prompt contact with the hospital or emergency services:
- A rapidly expanding or hard lump at the wrist puncture site
- Fresh bleeding through the dressing that does not stop with firm pressure
- Loss of sensation, tingling, or colour change in the hand or fingers
- Chest pain, breathlessness, or palpitations in the days following the procedure
- Fever, increasing redness or warmth at the puncture site (signs of infection, uncommon but worth knowing)
Your Follow-Up Appointment
Before you leave, your team will arrange or advise on follow-up. This is the appointment where the full implications of the results are discussed in a less pressured setting, with time for questions, discussion of any planned treatment, and review of medications and risk factors.
If you have not heard about a follow-up appointment within the timeframe given, contact the rooms to confirm. Do not assume everything is in hand if you have not been contacted.
Heart Matters Resource
When in Doubt, Get Checked Out
Any new chest pain, breathlessness, or wrist site concern after your angiogram deserves assessment, not a wait-and-see approach. Contact your hospital cardiac unit or present to emergency if you are uncertain.
Conclusion
Recovery from a radial artery coronary angiogram is, for most people, genuinely straightforward. The wrist approach has made what was once a more cumbersome recovery, flat on your back with groin pressure, into something most people navigate comfortably within a few hours.
The procedure itself is behind you. What comes next, the results conversation, the follow-up, any planned treatment, is the important part. You have taken a significant and proactive step toward understanding what is happening with your heart. That matters.
Rest, look after your wrist, attend your follow-up, and take your medications as prescribed. The team that looked after you during the procedure will continue to look after you through whatever comes next.