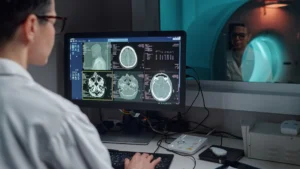
- Modern treatments have transformed heart attack care. What once required a week in hospital now often means two to three days, a reflection of how effective treatment has become, not a reason for concern.
- You will leave hospital on several new medications. Understanding what each one does, and why it matters, is one of the most important parts of recovery.
- Dual antiplatelet therapy (DAPT), typically aspirin combined with ticagrelor or clopidogrel, is critical after stenting and must not be stopped without medical advice.
- Cardiac rehabilitation is one of the most beneficial things you can do. It is structured, supervised, and designed specifically for where you are right now.
- Emotional recovery matters as much as physical recovery. Anxiety, fear, and low mood after a heart attack are common, expected, and treatable.
- A heart attack is not the end of an active life, it is the beginning of a better-managed one.
If you are reading this in the days after a heart attack, I want you to know something first: you are going to be okay.
I know that might be hard to believe right now. As an interventional cardiologist, I have sat with patients and families at every hour of the day and night, in the early hours of the morning, in the middle of family dinners, on weekends, on holidays, at the moment a heart attack changes everything. I have seen the fear on people’s faces. I have heard the questions that come tumbling out, and the ones that don’t come out at all because people are too shocked to ask them.
I understand what this feels like. And I want to tell you, genuinely, not just as a reassuring platitude, that the outlook after a heart attack treated with modern techniques is excellent. The procedures we use today, the medications we prescribe, the rehabilitation programmes available, they work. People go home. They return to work. They travel, they exercise, they live full and active lives. That is not the exception. That is what we see every day.
One of the things that surprises many patients is how quickly they are discharged from hospital. Where a heart attack once meant five to seven days in a monitored bed, modern treatment often means two to three days, sometimes less. That can feel confronting. It can feel like you are being sent home before you are ready, before you have had time to process what happened.
But that short stay is not a reflection of how serious your situation is, it is a reflection of how effective treatment has become. The critical work has been done. What comes next is your recovery, and that is where this article comes in.
Think of this as the conversation we would have if there were more time, the one that covers what happened, what your medications do, what to expect in the weeks ahead, and how to approach the rest of your life with confidence rather than fear. We are on this journey together.
What Happened, STEMI and NSTEMI
Heart attacks are classified into two main types based on what the ECG shows and the extent of the coronary artery blockage involved. Understanding which type you had helps make sense of what happened and why you received the treatment you did.
A STEMI ST-elevation myocardial infarction, occurs when a coronary artery becomes completely blocked. The blockage cuts off blood supply to a section of heart muscle entirely, producing characteristic changes on the ECG that are visible immediately. A STEMI is a time-critical emergency requiring the fastest possible restoration of blood flow, most commonly through emergency coronary angiogram and stenting, a procedure called primary PCI. You will have been quickly taken to a cardiac catheter lab, and the team will have opened up a blocked artery.
An NSTEMI non-ST-elevation myocardial infarction, involves a partial rather than complete blockage, producing less dramatic ECG changes but still can cause damage to the heart muscle. It is detected primarily through blood tests measuring troponin a protein released when heart cells are injured.
NSTEMI is no less serious than STEMI, it requires urgent assessment and typically proceeds to coronary angiogram and stenting. In both cases, the goal of treatment is the same: restore blood flow as quickly as possible, limit the extent of muscle damage, and begin protecting the heart against future events.
Regardless of which type of heart attack you experienced, the days and weeks that follow represent an equally important phase of treatment. What you do now, your medications, your rehabilitation, your lifestyle, directly influences your long-term outcome. And the good news is that all of this is within your control.
Your Medications, What They Are and Why They Matter
Most people leave the hospital after a heart attack on four or five new medications. If you were not on regular medication before, this can feel overwhelming. It is worth taking a moment to understand what each one does, because when you understand why a medication matters, it is much easier to take it consistently.
Dual antiplatelet therapy (DAPT) is the most critical medication combination in the early period after a heart attack and stenting. It consists of aspirin combined with a second antiplatelet agent, most commonly ticagrelor (Brilinta) or clopidogrel (Plavix).
Stents are metallic devices, and in the weeks and months after implantation, the body needs time to grow a protective layer of tissue over the stent surface. During this period, DAPT prevents clots forming on the stent. Stopping DAPT early, even for a few days, even for a seemingly minor procedure, carries a risk of complications, especially stent thrombosis, which is fortunately now uncommon. Don’t stop these medications without first discussing it with your cardiologist even if another doctor recommends it.
Statins such as atorvastatin or rosuvastatin, are prescribed at high doses after a heart attack not only to lower LDL cholesterol but because they have direct stabilising effects on plaques within the arterial walls, reducing the risk of future events.
If you experience muscle aches or other symptoms you think might be related, discuss this with your doctor rather than stopping on your own there are often alternatives available.
Beta-blockers such as metoprolol or bisoprolol, protect the heart muscle after a heart attack by reducing its workload and lowering the risk of arrhythmias. They are typically continued long-term, particularly if heart function has been affected.
ACE inhibitors or ARBs such as ramipril or candesartan, help remodel the heart after injury, reducing the risk of the heart muscle stretching and weakening over time. They are particularly important if echocardiography shows that the heart’s pumping function has been reduced, but are routinely prescribed after most heart attacks regardless.
Your medications at a glance
|
Aspirin + ticagrelor or clopidogrel Dual antiplatelet therapy (DAPT) Prevents clots forming on your stent. Critical, never stop without advice from your cardiologist. |
Atorvastatin or rosuvastatin Statin Lowers LDL cholesterol and stabilises plaques in artery walls. Reduces risk of future events. |
|
Metoprolol or bisoprolol Beta-blocker Reduces the heart’s workload and lowers the risk of dangerous rhythm problems after a heart attack. |
Ramipril or candesartan ACE inhibitor or ARB Helps the heart remodel and recover after injury. Reduces risk of the heart weakening over time. |
|
Take all of these medications every day, as prescribed. Each one protects your heart in a different way. Together they make a real difference. |
|
Cardiac Rehabilitation, One of the Best Things You Can Do
Cardiac rehabilitation is a structured, supervised programme designed specifically for people recovering from heart attacks, heart surgery, or other cardiac events. It typically involves a series of group sessions over six to twelve weeks, combining supervised exercise, education about heart health and medications, dietary guidance, and psychological support.
The evidence for cardiac rehabilitation is robust it reduces the risk of a further cardiac event, improves exercise capacity, reduces anxiety and depression, and improves quality of life. Despite this, participation rates remain lower than they should be, often because people are unsure what it involves or assume it is not for them.
It is absolutely for you. Cardiac rehabilitation is designed to meet you exactly where you are. Sessions are supervised by cardiac nurses and physiotherapists who understand what your heart has been through. Exercise starts gently and progresses at your pace.
You will almost certainly feel more capable after it than you did before, and the confidence it builds is as valuable as the physical conditioning. Ask your cardiologist or general practitioner for a referral if one has not already been arranged.
Physical Recovery, What to Expect
The amount of heart muscle affected and how quickly blood flow was restored both influence how quickly you recover physically. Many people with a relatively contained heart attack and prompt treatment feel surprisingly well within days and weeks post discharge.
Others, particularly those with larger areas of reduced heart function, take longer and require a more gradual activity progression. Both are normal. Recovery is not a race and comparing your timeline to someone else’s is rarely helpful.
As a general guide, light activity, short walks, gentle household tasks, can typically begin within a day or two of returning home, and gradually increase over the following weeks. Driving restrictions vary by country and clinical situation, your treating team will advise specifically.
Return to work depends on the nature of your job and how your recovery proceeds. Sexual activity can generally resume when you feel comfortable walking briskly without symptoms, a reasonable functional benchmark.
What to watch for: any new or returning chest discomfort, breathlessness that is getting worse rather than better, palpitations, or dizziness should be reported to your doctor promptly. These are not inevitable parts of recovery and always warrant assessment.
The Thoughts That Come at Night
I want to speak honestly about something that does not always get enough attention in the clinical setting: the emotional weight of what you have just been through.
In the quiet moments, often at night, often when the house is still and there is nothing to distract you, your mind will go to difficult places. You will think about your family, and what this means for them. You will think about your work, your finances, your future plans. You will wonder whether things will ever feel normal again.
All of that is completely understandable. A heart attack forces a reckoning with mortality that most of us are not used to confronting. It shakes the assumption that the body is reliable. These are not irrational thoughts, they are honest human responses to something genuinely significant.
What I want you to know is this: those dark moments are part of the journey, and they do pass. The anxiety that feels overwhelming in week one is almost always quieter by week four. The fear that grips you at 3am becomes more manageable when you are exercising again, sleeping better, and regaining confidence in your body.
Depression after a heart attack affects a meaningful proportion of people and is associated with poorer outcomes if left unrecognised and untreated. Signs to watch for include persistent low mood, loss of interest in activities you normally enjoy, withdrawal from social contact, difficulty concentrating, or a sense of hopelessness about the future.
If you are experiencing any of these, please raise it with your doctor. Effective support is available, whether through psychological therapy, medication, or both. Getting help is not a sign of weakness. It is a clinical need, and treating it appropriately is part of recovering well.
Your family and close friends are also adjusting. Open conversations about what you need, and what you do not, help enormously. You do not have to carry this alone.
Lifestyle Going Forward
A heart attack is caused by atherosclerosis, the gradual buildup of plaque in the coronary arteries, and the risk factors that drive that process do not disappear after the event. Managing them actively is not a burden. It is an opportunity a chance to make changes that genuinely improve your health and reduce the risk of another event.
Managing your cardiovascular risk factors
|
Blood pressure Target below 130/80 mmHg. The most important modifiable risk factor. |
Cholesterol LDL target below 1.4 mmol/L after a heart attack. Targets vary by country, check with your doctor. |
Smoking Stopping produces cardiovascular benefits almost immediately, one of the most powerful changes. |
|
Diabetes Good blood sugar control reduces damage to blood vessels. HbA1c monitoring is key. |
Weight Even modest weight loss reduces blood pressure, cholesterol, and strain on the heart. |
Physical activity Regular, sustainable activity improves heart function, mood, and blood pressure. |
|
Diet A Mediterranean-style diet, vegetables, wholegrains, fish, and olive oil, is the best-evidenced pattern for cardiovascular protection. |
Stress and sleep Chronic stress and poor sleep raise blood pressure and worsen heart health. Both are worth actively managing. |
|
|
No single change has to be perfect. Small, consistent improvements add up and cardiac rehabilitation will help you work through each of these with expert guidance. |
||
Regular physical activity, built up gradually and guided by your rehabilitation programme, has direct benefits on heart muscle function, blood pressure, cholesterol, and mood. The goal is not to become an athlete, it is to be consistently, sustainably active. Simple walking is a great way to start.
Two resources on our site worth reading as you build your recovery: our guide to the Mediterranean diet, the best-evidenced dietary pattern for cardiovascular protection, and our article on smoking and the heart.
Your Recovery Toolkit, From Heart Matters
|
Healthy Living The Mediterranean Diet and Your Heart The best-evidenced dietary pattern for cardiovascular protection, practical, enjoyable, and well suited to recovery. |
Healthy Living Smoking and Cardiovascular Health Stopping smoking produces cardiovascular benefits almost immediately. Here is what the evidence shows and how to approach quitting. |
|
Healthy Living Walking and Your Heart One of the first exercises recommended after a cardiac event, and one of the most underrated. Why walking deserves more credit than it gets. |
Free Download Heart Health Risk Factor Checklist A practical checklist covering the key cardiovascular risk factors, with space for notes to bring to your next appointment. |
Free Download, Heart Matters
Our Heart Health Risk Factor Checklist helps you understand and track the key cardiovascular risk factors, with a traffic light system and space for questions to raise at your next appointment. Free to download, print, and bring with you.
Heart Matters Resource
When in Doubt, Get Checked Out
After a heart attack, you will become more attuned to how your body feels, and that awareness is valuable. If something does not feel right, trust that instinct and get it checked. That is not anxiety. That is good self-care.
A Final Word
Recovery after a heart attack is a journey that unfolds over weeks and months, not days. There will be moments of uncertainty, days when fatigue outpaces expectation, and questions that arise long after discharge. All of that is normal.
What matters is that you understand what happened, why your treatment is structured the way it is, and that you approach the process as an active participant rather than a passive observer. You have more control over your outcome than you might realise right now.
The heart has a remarkable capacity to adapt and recover, particularly when supported by the right medications, rehabilitation, and lifestyle. Most people who have had a heart attack go on to live full, active, and meaningful lives often with a greater awareness of their health and a clearer sense of what matters.
Take it one day at a time. Keep your appointments. Take your medications. Be patient with yourself. And know that the team looking after you, and the information in these pages, is here for every step of the way.