Key Points
- High blood pressure affects around one in three adults worldwide, and despite many effective medications being available, a large proportion of people still do not achieve adequate control.
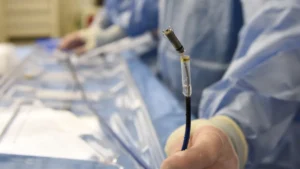
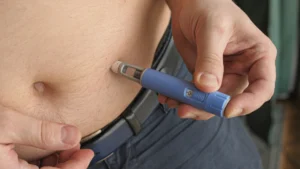
- A new treatment called zilebesiran uses RNA technology to switch off a key protein involved in raising blood pressure, delivered as a single injection every six months.
- Early clinical trials have shown meaningful reductions in blood pressure lasting up to six months from a single dose.
- Zilebesiran is not yet approved or available, it is still in clinical trials. A major international study enrolling around 11,000 patients is now underway to determine whether it can reduce heart attacks, strokes, and cardiovascular death.
- For now, the cornerstones of blood pressure management remain lifestyle modification and existing medications, but this technology represents a genuinely exciting direction for the future.
Managing high blood pressure is one of the most important things we can do for long-term heart health. It is also, for many people, one of the most frustrating. The medications work, the evidence behind them is excellent, but taking tablets every single day, sometimes multiple times a day, is genuinely difficult to sustain over years and decades. Many people forget doses, experience side effects, or simply find the routine hard to maintain.
That is the problem a new type of treatment is trying to solve. Instead of a daily tablet, a single injection every six months. And the science behind how it works is, frankly, remarkable.
Why is blood pressure so hard to control?
High blood pressure, hypertension, often causes no symptoms at all. It is genuinely possible to have dangerously elevated blood pressure for years without knowing it, which is why it is sometimes called the silent killer. Left unmanaged, it significantly increases the risk of heart attack, stroke, heart failure, and kidney disease.
The challenge is that blood pressure is regulated by multiple overlapping systems in the body, and the medications that work on one pathway do not always work well enough on their own. Many people end up on two, three, or even four different medications, each needing to be taken daily. And when life gets busy, doses get missed. Missed doses mean inadequate control. Inadequate control means ongoing risk.
This is not a criticism of patients, it is simply the reality of managing a chronic, symptomless condition with daily tablets over a lifetime. The system has real limitations, and researchers have been looking for better solutions.
What is RNA therapy and how does it work here?
Every cell in the body contains genetic instructions, DNA, that tell it which proteins to make. One of those proteins plays a key role in a chain reaction that ultimately raises blood pressure. The new treatment, called zilebesiran, works by intercepting the instructions before that protein can be made at all.
Think of it like this, rather than trying to block the protein once it has already been produced, zilebesiran switches off the instruction to make it in the first place. This is done using a technology called RNA interference, which essentially silences a specific gene in the liver, the gene responsible for producing a substance that sits right at the top of the blood pressure regulation chain.
The result is a sustained, prolonged reduction in blood pressure that lasts for months after a single injection, because the underlying signal driving blood pressure up has been turned down at its source.
of blood pressure control from a single injection, day and night, around the clock, without daily tablets
What do the clinical trials show?
Zilebesiran has now been through three large Phase 2 clinical trials, the carefully controlled studies that test whether a new treatment works and is safe before progressing to the larger trials needed for regulatory approval.
The results have been encouraging. In the first trial, zilebesiran used on its own produced meaningful reductions in blood pressure sustained over the full six months, day and night, consistently, without the peaks and troughs that can occur with daily oral medications when doses are missed.
A second trial tested zilebesiran added on top of an existing blood pressure medication, in patients who were not adequately controlled on their current treatment. Again, the combination produced significant additional blood pressure reductions that lasted for months.
A third, more recent trial focused specifically on patients with established heart disease or high cardiovascular risk, the people where controlling blood pressure matters most urgently. The results were more modest in this harder-to-treat population, but they helped define who is most likely to benefit and how the larger Phase 3 trial should be designed.
What excites me about this technology is not just the blood pressure reduction, it is the consistency. A treatment that works around the clock for six months, without depending on someone remembering a daily tablet, could make a real difference to the people who need it most.
What about side effects?
No treatment comes without potential side effects, and zilebesiran is no exception. The most commonly reported issue in the trials was mild reactions at the injection site, the skin where the injection is given, which is common with any subcutaneous injection and generally settles quickly. Some patients also showed a small rise in potassium levels in the blood, which is something doctors monitor for with some existing blood pressure medications too.
More serious adverse events were uncommon, and the overall safety profile from the Phase 2 programme was considered acceptable enough to proceed to the large Phase 3 study. That study, however, will be the real test, with 11,000 patients followed over several years, it will provide the comprehensive safety data needed before any regulatory approval could be considered.
Where does the programme stand now?
As of late 2025, zilebesiran has entered its pivotal Phase 3 trial, the large, definitive study that will determine whether it earns regulatory approval. This trial, named ZENITH, is enrolling around 11,000 patients across more than 30 countries. Its goal is not just to show that zilebesiran lowers blood pressure numbers, it aims to demonstrate that it actually reduces the risk of heart attack, stroke, cardiovascular death, and heart failure. That is the gold standard test for any new cardiovascular therapy.
Results from a trial of this size typically take several years to mature. If the outcomes are positive, zilebesiran could potentially become available in the latter part of this decade. If they are not, the scientific community will learn something equally important about the limits of this approach.
What does this mean for patients right now?
The honest answer is, not very much yet, in practical terms. Zilebesiran is not approved, not available, and not something your doctor can prescribe today. It is a promising investigational treatment that has cleared early hurdles but has a significant journey still ahead of it.
What it does represent is a genuine shift in how we might think about treating hypertension in the future. For patients who struggle with daily medication adherence, who have multiple side effects from existing treatments, or whose blood pressure remains difficult to control despite several medications, a twice-yearly injection could eventually offer a meaningful new option.
In the meantime, the best thing anyone with high blood pressure can do is work with their doctor on optimising their current management, whether that is reviewing medications, addressing lifestyle factors, or improving home monitoring. Those tools are available today and they work.
Conclusion
RNA therapy for high blood pressure represents one of the most scientifically interesting developments in cardiovascular medicine in recent years. The concept of turning down the body’s own blood pressure signal at its source, once every six months with a single injection, is genuinely novel, and the early trial results are encouraging enough to have justified a major global outcomes study.
We are watching this space closely. The results of the Phase 3 trial will be one of the most anticipated findings in hypertension research over the coming years, and we will update this article as the evidence develops.
For now, the message to anyone managing high blood pressure is straightforward, the treatments we have work, and using them consistently remains the most important thing you can do. The future may bring better options. But the present already has good ones.
Free Resources
Our Heart Glossary explains terms like hypertension, RNA therapy, angiotensinogen, and clinical trials in plain language.