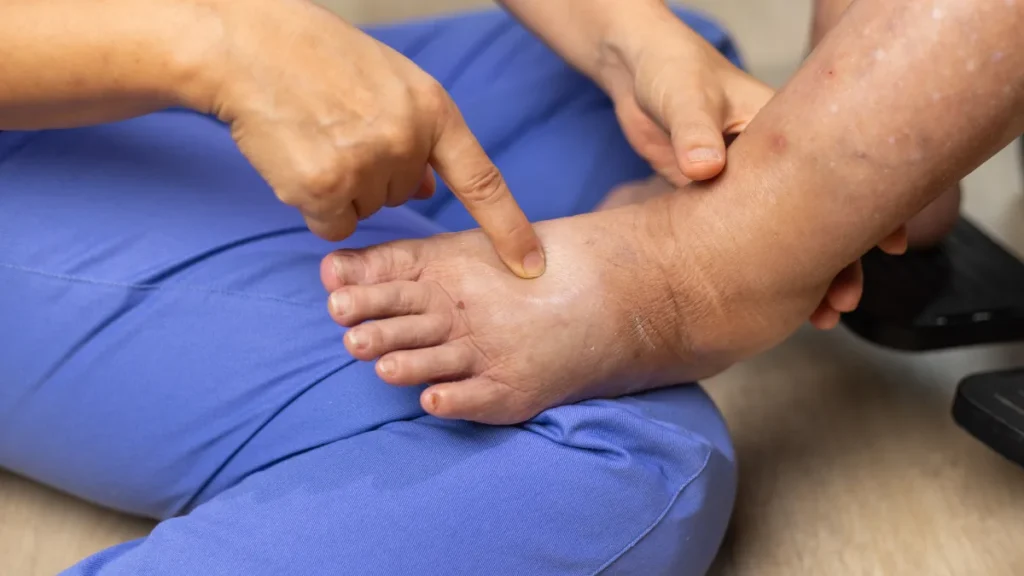
- Ankle swelling, or oedema has a wide range of causes, most of which are benign. Long periods of sitting or standing, heat, and pregnancy are among the most common.
- Calcium channel blockers including amlodipine, one of the most widely prescribed blood pressure medications, are a frequently overlooked and very common cause of ankle swelling that is often mistaken for a more serious condition.
- Heart failure sometimes called congestive cardiac failure or CCF, is an important cardiac cause of ankle swelling that should always be considered, particularly when swelling is bilateral, progressive, and accompanied by breathlessness or fatigue.
- Other causes include venous insufficiency, kidney disease, liver disease, thyroid dysfunction, and deep vein thrombosis, each requiring a different assessment approach.
- A medication review is one of the most valuable first steps in any assessment of ankle swelling, and often provides the answer without the need for extensive further investigation.
Ankle swelling is one of the most common symptoms people present with across medicine, and one of the most important to assess carefully, because the causes range from something as straightforward as a long day on your feet to something as significant as heart failure. Getting the distinction right matters enormously, both to avoid unnecessary anxiety about benign causes and to ensure that important ones are not missed.
As a cardiologist, I see patients referred for ankle swelling regularly, and in a significant proportion of cases, the answer is not cardiac at all. It is their amlodipine, or another calcium channel blocker, causing peripheral vasodilation and fluid redistribution into the tissues of the lower legs. This is a well-established, common side effect of an entirely effective and valuable medication, and yet it is frequently not recognised as the cause, leading to further investigations, unnecessary worry, and months of discomfort that could have been resolved with a straightforward medication adjustment.
Before embarking on a full investigation of ankle swelling, always review the medication list. Calcium channel blockers are one of the most common causes of bilateral ankle oedema in people on cardiovascular medications, and adjusting the dose or switching to an alternative often resolves it completely.
Understanding Oedema, What Is Actually Happening
Oedema the medical term for swelling caused by fluid accumulation in the tissues, occurs when the balance between fluid moving out of the blood vessels into the surrounding tissue and fluid being reabsorbed or drained by the lymphatic system is disrupted. Gravity plays a significant role: fluid naturally pools in the lowest part of the body, which is why the ankles and lower legs are almost always the first and most prominently affected area.
The swelling is typically described as pitting oedema meaning that pressing firmly on the swollen area leaves a temporary indentation, or pit, that slowly fills back in. This pitting quality is a useful clinical sign that distinguishes true oedema from other causes of leg swelling such as lipedema (abnormal fat deposition) or lymphoedema (lymphatic obstruction), which tend to be non-pitting.
The Calcium Channel Blocker Connection
Calcium channel blockers are among the most widely prescribed medications in cardiovascular medicine, used for high blood pressure, angina, and certain arrhythmias. They work by relaxing the smooth muscle in blood vessel walls, causing vasodilation, a widening of the vessels that reduces resistance and lowers blood pressure. This vasodilatory effect is what makes them effective, but it also has a direct consequence for fluid balance in the lower limbs.
When calcium channel blockers dilate the small arteries (arterioles) feeding the capillary beds in the legs, more fluid is pushed out of the capillaries into the surrounding tissue than the venous and lymphatic systems can efficiently drain. The result is bilateral ankle and lower leg swelling, typically worse at the end of the day, improved with elevation overnight, and not associated with breathlessness or other symptoms of heart failure.
The most commonly implicated agent is amlodipine one of the most prescribed medications in the world, but the effect is a class phenomenon seen with all dihydropyridine calcium channel blockers including felodipine, nifedipine, and lercanidipine. Non-dihydropyridine agents such as diltiazem and verapamil cause less peripheral oedema due to their different mechanism of action.
The management is straightforward once the cause is identified. Reducing the dose of the calcium channel blocker often reduces the oedema significantly. Switching to a different antihypertensive class, such as an ARB or ACE inhibitor, may resolve it entirely. In some cases, adding a low-dose diuretic or switching to lercanidipine (which causes less peripheral oedema than amlodipine at equivalent doses) is a practical solution. The key is not to stop the medication without discussion, calcium channel blockers are prescribed for good clinical reasons, but to raise it with your doctor so the options can be explored.
Cardiac Causes, When Ankle Swelling Signals Something More
While medication side effects and benign causes account for the majority of ankle swelling seen in clinical practice, cardiac causes are important to identify and should not be missed. The most significant is heart failure sometimes called congestive cardiac failure (CCF).
In heart failure, the heart’s pumping function is impaired, it cannot move blood forward efficiently, leading to a build-up of pressure in the venous system. This increased venous pressure forces fluid out of the capillaries and into the surrounding tissue, producing oedema that typically starts at the ankles but can progress up the legs and, in severe cases, into the abdomen. Heart failure oedema has a characteristic pattern: it is bilateral, symmetrical, progressive over days to weeks, and almost always accompanied by other symptoms, breathlessness on exertion or lying flat, fatigue, and reduced exercise tolerance.
The distinction between heart failure oedema and calcium channel blocker oedema is usually clear from the history alone, but targeted blood tests and an echocardiogram provide definitive confirmation when needed.
BNP (B-type natriuretic peptide) and its related marker NT-proBNP are proteins released by the heart muscle cells when the heart walls are under increased stress or stretch, which occurs when the heart is struggling to pump effectively. A raised BNP or NT-proBNP level in the blood is a strong indicator that heart failure may be contributing to the swelling, and provides a valuable first screen before arranging an echocardiogram. A normal result is highly reassuring and makes a cardiac cause much less likely. The test is a simple addition to routine blood work and takes no special preparation. Results are interpreted alongside the clinical picture, a mildly elevated level does not automatically mean heart failure, as other conditions including kidney disease, atrial fibrillation, and obesity can also affect the reading. A dedicated article on BNP and what the result means is available in our Diagnostic Tests section.
| Feature | Calcium Channel Blocker Oedema | Heart Failure Oedema |
|---|---|---|
| Distribution | Bilateral ankles and lower legs | Bilateral, may extend up legs; can involve abdomen |
| Pattern | Worse at end of day, improves overnight with elevation | Progressive over days/weeks, less responsive to elevation |
| Associated symptoms | None, no breathlessness, no fatigue | Breathlessness, fatigue, reduced exercise tolerance |
| Medication history | Calcium channel blocker on prescription | May or may not be on diuretics already |
| BNP blood test | Normal | Elevated |
| Echocardiogram | Normal structure and function | Reduced ejection fraction or diastolic dysfunction |
Other Important Causes
Venous insufficiency is one of the most common non-cardiac causes of ankle swelling, occurring when the valves in the leg veins that prevent blood from flowing backwards become damaged or incompetent. Blood pools in the lower legs, increasing venous pressure and causing oedema, skin discolouration, varicose veins, and in advanced cases, venous ulcers. It is typically worse with prolonged standing and improves with elevation and compression stockings.
Deep vein thrombosis (DVT) a blood clot in the deep veins of the leg, causes swelling that is typically unilateral (one leg only), often with warmth, redness, and pain in the affected calf. DVT requires urgent assessment because of the risk of the clot travelling to the lungs (pulmonary embolism). Any new, sudden, unilateral leg swelling, particularly after surgery, long-haul travel, or prolonged immobility, should be assessed promptly with a leg vein ultrasound.
Kidney disease reduces the kidneys’ ability to excrete sodium and water, leading to fluid retention throughout the body including the ankles. Liver disease particularly cirrhosis, reduces the production of albumin, the blood protein that maintains fluid within the vessels; low albumin allows fluid to leak into the tissues. Both conditions produce a more generalised oedema pattern and are identified through blood tests.
Thyroid dysfunction both underactivity (hypothyroidism) and, less commonly, overactivity, can cause ankle swelling through different mechanisms. Hypothyroidism in particular produces a characteristic non-pitting oedema called myxoedema, which affects the face and lower legs and is associated with other features of thyroid underactivity such as fatigue, cold intolerance, and weight gain. A simple TSH blood test identifies this.
Prolonged sitting or standing particularly in heat, causes dependent oedema through gravitational fluid pooling and is entirely benign, though uncomfortable. Air travel is a common precipitant. This type of swelling resolves reliably with elevation and movement, and requires no investigation if it is clearly situational and there are no associated symptoms.
How Ankle Swelling Is Assessed
The assessment begins with a careful history, how long the swelling has been present, whether it is one leg or both, what makes it better or worse, and crucially, what medications you are taking. A physical examination assesses the distribution and character of the swelling, checks for pitting, examines the skin for signs of venous insufficiency, and assesses the heart and lungs for any signs of cardiac decompensation.
Blood tests are the essential first investigation, checking kidney function, liver function, thyroid function, a full blood count, albumin, and BNP or NT-proBNP as a cardiac screen. An ECG is performed when a cardiac cause is suspected. An echocardiogram assesses heart structure and function definitively when heart failure is in the differential. A leg vein ultrasound is arranged when DVT is suspected, particularly for unilateral swelling with pain or a risk factor for clotting.
- Elevate your legs when resting, ideally above heart level, to reduce fluid pooling by gravity.
- Keep moving even simple ankle pump exercises when sitting for long periods help the calf muscle pump venous blood back up the legs.
- Reduce salt intake excess sodium promotes fluid retention and worsens oedema from any cause.
- Wear compression stockings if recommended by your doctor, they are particularly effective for venous insufficiency and dependent oedema.
- Review your medications check whether any contain “-dipine” in the name (amlodipine, felodipine, nifedipine) and raise the question with your doctor if so.
- Do not self-prescribe diuretics while diuretics reduce fluid, taking them without medical supervision can cause dehydration and electrolyte problems.
Heart Matters Resource
When in Doubt, Get Checked Out
If your ankle swelling is new, progressive, or accompanied by any other symptom that concerns you, please do not dismiss it. Heart Matters has a dedicated resource covering the symptoms that should never be ignored and why seeking help is always the right call.
Conclusion
Ankle swelling is common, and in the majority of cases the cause is benign, gravity, prolonged sitting, heat, or a medication side effect. The calcium channel blocker connection in particular is worth knowing about: if you are on amlodipine or a similar medication and have developed ankle swelling, raise it with your doctor. A simple dose adjustment or medication switch often resolves it completely, and you do not need to simply accept it as an inevitable consequence of your treatment.
Where ankle swelling is progressive, bilateral, and accompanied by breathlessness or fatigue, heart failure is an important diagnosis to exclude, and it is one that responds well to treatment when identified early. A BNP blood test and echocardiogram provide the answer quickly and definitively.
As with every symptom covered on Heart Matters, the goal is not to alarm, but to inform. Understanding what might be causing your ankle swelling, and knowing which features warrant prompt attention, puts you in a far better position to have a productive conversation with your doctor and get the right answer without unnecessary delay.
More from Heart Matters
- The ACE Inhibitor Cough: A Common Side Effect with a Simple Solution
- Chest Pain: Causes, Symptoms, and When to Seek Help
- Fainting and Syncope: What It Might Be Telling You
- The Importance of Monitoring Your Blood Pressure
- Diagnostic Tests: All Investigations Explained
- When in Doubt, Get Checked Out, Heart Matters Resource