- Aortic stenosis is a narrowing of the heart’s aortic valve, one of the most common valve conditions, particularly in older adults.
- Many people have no symptoms for years. When symptoms do appear, they signal that the heart is under significant strain and intervention is usually needed.
- Treatment has been transformed by TAVR, a minimally invasive procedure that has expanded options for patients previously considered too high-risk for surgery.
- Once symptoms develop in severe aortic stenosis, timely intervention is essential. Delay carries real risk.
- Recent trial evidence and updated 2025 guidelines now support intervening earlier, sometimes before symptoms appear, in carefully selected patients.
The aortic valve is the heart’s gateway to the body. With every heartbeat, it opens to let oxygen-rich blood surge out through the aorta to every organ and tissue, then snaps shut to prevent any from flowing back. It does this roughly 100,000 times a day, every day, for a lifetime.
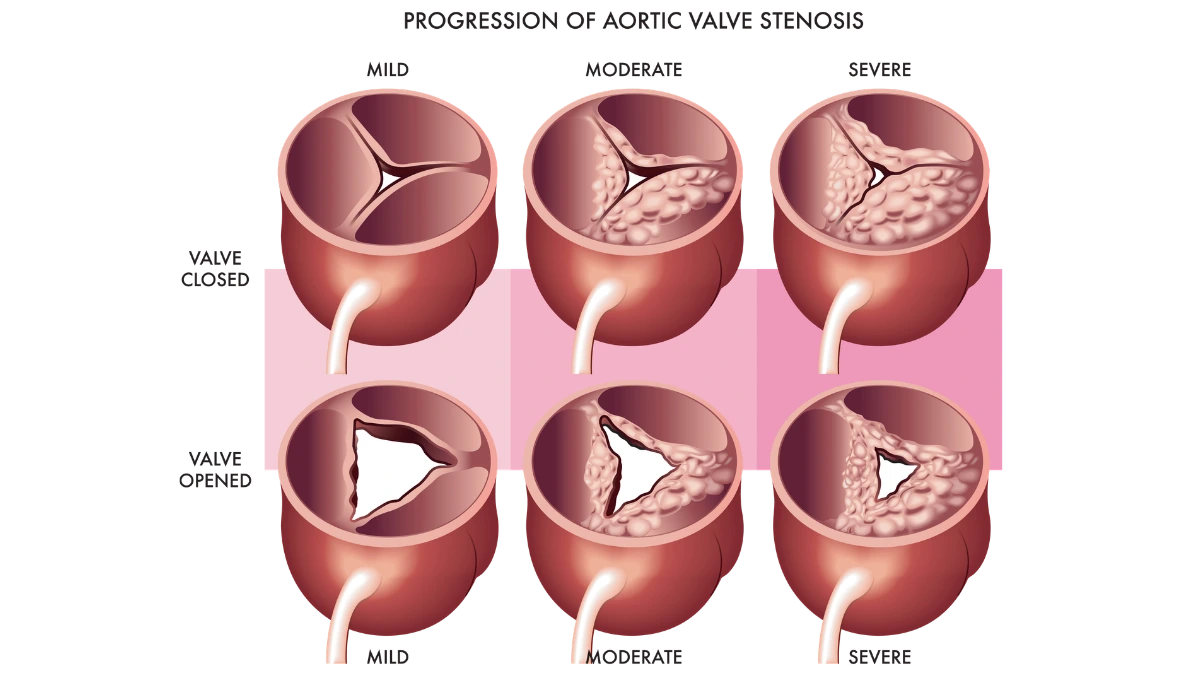
Aortic stenosis is what happens when that gateway begins to narrow. The valve leaflets, normally thin and supple, gradually thicken, stiffen, and calcify, forcing the heart to work increasingly hard to push blood through a shrinking opening. Over time, that extra strain takes its toll. Aortic stenosis is one of the most common valve conditions affecting adults, estimated to affect around 9 million people worldwide, and its consequences, left untreated, can be severe.
The good news is that our understanding and treatment of this condition have advanced dramatically. From open-heart surgery to catheter-based valve replacement performed without a single surgical incision, patients today have options that simply did not exist a generation ago.
The Aortic Valve: How It Works
The aortic valve sits between the left ventricle, the heart’s main pumping chamber, and the aorta, the body’s largest artery. In most people it has three thin, flexible leaflets (a tricuspid valve) that work like a one-way door: open during systole (when the heart contracts) to allow blood to be ejected, then closed tightly during diastole (when the heart relaxes) to prevent any blood flowing back.
Some people are born with only two leaflets, a bicuspid aortic valve. This congenital variation affects around 1 to 2% of the population and significantly increases the lifetime risk of developing aortic stenosis, often at a younger age than those with a normal tricuspid valve.
Symptoms of Aortic Stenosis
One of the most important things to understand about aortic stenosis is how quietly it can progress. For years, sometimes decades, the valve can narrow significantly with no symptoms at all. The heart, a remarkably adaptive organ, compensates by working harder. It is often only when that compensation begins to fail that symptoms emerge.
Many patients are completely unaware they have aortic stenosis until it is picked up incidentally, on a routine examination, or during an echocardiogram performed for another reason. This is why regular check-ups matter.
When symptoms do develop, they typically include some combination of the following:
- Chest pain or tightness, particularly during physical activity, as the heart struggles to meet increased demand through a narrowed valve.
- Shortness of breath, initially on exertion, but in advanced disease, at rest or when lying flat.
- Fatigue, a persistent tiredness that goes beyond what activity alone would explain.
- Dizziness or fainting: reduced blood flow to the brain, particularly during exertion, can cause lightheadedness or blackouts.
- Heart palpitations, sensations of a racing or irregular heartbeat.
The severity of symptoms closely mirrors the degree of valve narrowing. Mild stenosis may cause no symptoms at all; severe stenosis, particularly once it becomes symptomatic, requires prompt attention. If you experience any of these symptoms, especially chest pain, breathlessness, or fainting, seek medical evaluation without delay.
What Causes Aortic Stenosis?
Aortic stenosis develops through several distinct pathways, though the end result, progressive valve narrowing, is the same.
Age-related degeneration is by far the most common cause. Over decades, calcium deposits gradually accumulate on the valve leaflets, causing them to stiffen and lose their flexibility. This process is similar in some ways to atherosclerosis: the same risk factors that clog coronary arteries also accelerate valve calcification. Aortic stenosis from degenerative calcification is predominantly a condition of people over 65.
Bicuspid aortic valve is the leading cause in younger patients. A valve with only two leaflets is structurally less efficient, subjecting itself to abnormal mechanical stress with every heartbeat. Over time this accelerates the calcification process, often causing clinically significant stenosis in a patient’s 40s or 50s rather than their 70s.
Rheumatic fever, a complication of untreated streptococcal throat infection, can damage the valve leaflets, causing scarring and fusion that leads to stenosis. Rheumatic heart disease has become far less common in high-income countries but remains a significant cause of valve disease globally.
How Is Aortic Stenosis Diagnosed?
Aortic stenosis is often first suspected when a doctor hears a characteristic heart murmur through a stethoscope, a harsh, systolic sound caused by turbulent blood flow through the narrowed valve. From there, the key diagnostic tool is the echocardiogram.
Echocardiogram (cardiac ultrasound) is the cornerstone of diagnosis and severity assessment. It provides detailed images of the valve’s structure, measures the degree of narrowing (valve area), and calculates the pressure gradient across the valve, the difference in pressure between the left ventricle and the aorta, which reflects how hard the heart is working to push blood through.
Electrocardiogram (ECG) can identify changes in the heart’s electrical activity associated with the increased workload imposed by aortic stenosis, including signs of left ventricular hypertrophy (thickening of the heart muscle).
Cardiac catheterisation may be performed in selected cases to directly visualise the coronary arteries and assess the valve, particularly when surgical or catheter-based intervention is being planned.
Assessing Severity
Not all aortic stenosis is the same. The condition exists on a spectrum from mild to severe, and the treatment approach depends critically on where a patient sits on that spectrum. Two key measurements from the echocardiogram determine severity:
valve area indicating severe aortic stenosis
International valve disease guidelines
mean pressure gradient suggesting severe disease
normal aortic valve area for comparison
Valve area: a normal aortic valve is approximately 3 to 4 square centimetres. Severe stenosis is defined as a valve area below 1.0 square centimetre, less than a quarter of its original size. Pressure gradient: the higher the gradient, the harder the heart must work to eject blood through the obstruction. A mean gradient above 40 mmHg is generally consistent with severe disease. Together these measurements, combined with symptoms and cardiac function, guide the timing of intervention.
Treatment Options
There is no medication that reverses aortic stenosis or slows its progression. The only definitive treatment is replacing the diseased valve. The question is how, and when. Two main approaches exist, and the choice between them is one of the most important decisions made by the heart team.
Surgical aortic valve replacement (SAVR)
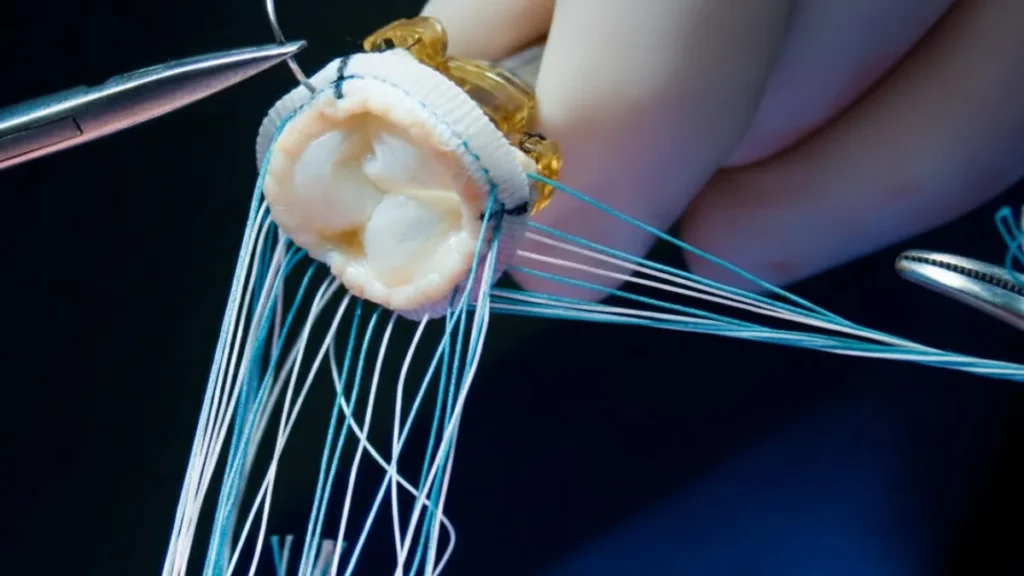
SAVR has been the gold standard treatment for severe aortic stenosis for over half a century. During the procedure, the diseased valve is completely removed and replaced with a prosthetic valve, either a mechanical valve made from synthetic materials, or a biological (tissue) valve derived from animal tissue. The operation is performed by opening the breastbone (a sternotomy) or, increasingly, through smaller, less invasive incisions.
The key advantage of SAVR is durability, particularly with mechanical valves, which can last well beyond 20 years. SAVR also allows for complete removal of the calcified native valve and the flexibility to address other cardiac conditions simultaneously, such as coronary artery disease requiring bypass surgery. For younger patients who need a valve that will outlast them, or those with concurrent conditions requiring open surgery, SAVR remains the preferred approach.
Transcatheter aortic valve replacement (TAVR)
TAVR, also known as TAVI (transcatheter aortic valve implantation) in Europe and Australia, represents one of the most significant advances in cardiovascular medicine of the past two decades. Rather than opening the chest, a collapsible replacement valve, typically made from specially treated cow or pig tissue mounted within a metal stent, is delivered to the heart through a catheter inserted via the femoral artery in the groin. Once positioned precisely at the site of the diseased valve, it is expanded, pushing the old valve leaflets aside and immediately taking over its function.
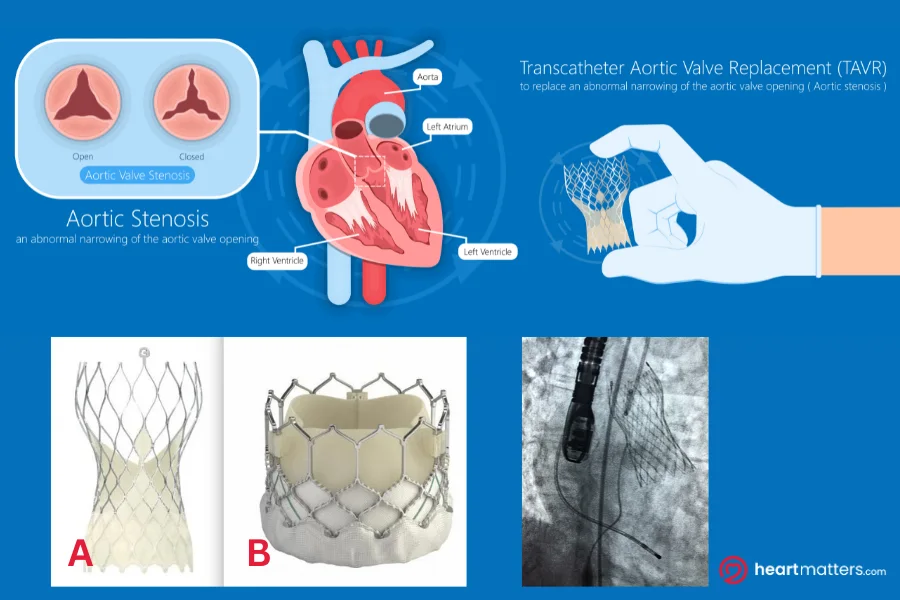
TAVR was initially reserved for patients considered too high-risk or too frail for open-heart surgery. As clinical experience accumulated and trial data matured, through landmark studies such as the PARTNER and SAPIEN trials, the evidence base expanded to include patients at intermediate and ultimately low surgical risk. FDA approval for low-risk patients followed in 2019, cementing TAVR as the dominant treatment approach for symptomatic severe aortic stenosis across the risk spectrum. The most recent European guidelines, updated in 2025, now recommend TAVR for most patients aged 70 and over, with surgery remaining the standard for younger patients at low surgical risk.
The benefits are compelling: no sternotomy, no heart-lung machine, shorter hospital stays, and faster recovery. For older patients or those with other significant health conditions, TAVR has transformed what was previously a high-risk surgical undertaking into a procedure most patients recover from within days.
Balloon valvuloplasty
In selected patients who are not yet candidates for valve replacement, or as a bridge to a definitive procedure, balloon valvuloplasty may provide temporary relief. A balloon is inflated within the narrowed valve to widen the opening and improve flow. The effects are not durable and the stenosis typically recurs, but the procedure can stabilise a patient in the short term or help clarify how much the valve is contributing when symptoms are unclear.
In Memoriam: Professor Alain Cribier (1945–2024)
No article on aortic stenosis would be complete without acknowledging the man who changed everything. Professor Alain Cribier, a French interventional cardiologist, performed the first balloon aortic valvuloplasty in 1985, and then, dissatisfied with its lack of durability, spent the following decade developing the concept of replacing the valve entirely through a catheter.
On 16 April 2002, he performed the world’s first TAVR procedure in a patient too ill for surgery. It was a defining moment in cardiovascular medicine. Since then, millions of patients worldwide have benefitted from the technique he pioneered, many of whom would have had no treatment option without it.
Professor Cribier passed away in 2024. His legacy is measured in lives.
When to Intervene: The Importance of Timing
Aortic stenosis is a progressive condition. The valve does not improve on its own. It only narrows further over time. For many years, close surveillance with regular echocardiograms is entirely appropriate. But the picture changes the moment symptoms appear.
Once symptoms develop in severe aortic stenosis, the prognosis without intervention deteriorates rapidly. Timely valve replacement is not elective. It is essential.
Chest pain, breathlessness, and syncope (fainting) in the context of severe aortic stenosis are red flags that demand prompt assessment and typically urgent intervention. The heart team, comprising cardiologists, cardiac surgeons, imaging specialists, and anaesthesiologists, reviews each case collectively to determine the best approach and the right timing.
For patients with severe stenosis but no symptoms, the thinking has shifted significantly in recent years. The landmark EARLY TAVR trial, published in 2024, found that treating carefully selected patients before symptoms appeared roughly halved the combined risk of death, stroke, or unplanned cardiac hospitalisation compared with waiting under close surveillance. Reflecting this evidence, the 2025 European valve guidelines now support earlier intervention in severe aortic stenosis without symptoms when the procedural risk is low, a clear departure from the traditional watchful waiting approach.
That does not mean every patient without symptoms needs an immediate procedure. Features such as rapid progression on serial echocardiograms, very low valve area, or declining cardiac function strengthen the case for acting sooner, while others may still reasonably choose surveillance with regular review. The right timing remains an individual decision made with the heart team. This individualised approach, guided by multidisciplinary expertise, is at the heart of modern valve disease management.
Conclusion
Aortic stenosis is common, often silent in its early stages, and potentially serious when left untreated. The reassuring message is that the treatment options available today, both surgical and catheter-based, are safe, effective, and transformative. Patients who would once have been told they were too old or too sick for intervention now routinely undergo TAVR and leave hospital days later with a functioning new valve and dramatically improved symptoms.
The key is awareness and timely action. If you or someone you know experiences unexplained breathlessness, chest discomfort, or episodes of dizziness or fainting, particularly in the context of a known heart murmur or valve condition, do not wait. Seek evaluation. The gateway can be restored.