- Ventricular ectopic beats, also called premature ventricular contractions (PVCs) are extra heartbeats originating in the lower chambers of the heart, and are extremely common in the general population.
- In people with a structurally normal heart ventricular ectopics are almost always benign, even when frequent. Reassurance after proper assessment is often the only treatment needed.
- The characteristic sensation is a “missed beat” or thump caused by the ectopic firing early, a brief pause, and then a stronger-than-normal beat that follows.
- Common triggers include caffeine, alcohol, stress, poor sleep, and hormonal changes all of which are addressable with lifestyle adjustment.
- Assessment typically involves an ECG, blood tests, Holter monitor, and echocardiogram, the last of which is particularly important in determining the significance of any ectopic burden.
The heart relies on a precise electrical system to maintain its rhythm, a system that works silently and reliably in the background for most of our lives. Occasionally, however, an extra electrical impulse fires from an unexpected location in the lower chambers, producing a beat that is slightly out of sequence with the normal rhythm. This is a ventricular ectopic beat, and while the sensation it produces can be alarming, it is one of the most common and most frequently benign findings in cardiology.
Patients often arrive having already spent considerable time worrying about what they have been feeling. Part of my role as a cardiologist is to explain clearly what is happening, to assess it properly, and, in the majority of cases, to offer the reassurance that these beats, though noticeable and sometimes bothersome, do not reflect a dangerous heart condition. Understanding what a ventricular ectopic beat actually is goes a long way toward making that reassurance meaningful.
What Are Ventricular Ectopic Beats?
Ventricular ectopic beats sometimes called premature ventricular contractions (PVCs) or ventricular extrasystoles, are abnormal electrical impulses that originate in the ventricles, the heart’s lower chambers responsible for pumping blood to the lungs and the rest of the body. Rather than following the normal sequence, where the electrical signal travels from the sinus node through the atria and down into the ventricles in a coordinated fashion, ectopic beats arise spontaneously from a different location, causing the ventricles to contract prematurely and out of sync.
The result is a beat that feels distinctly different. What most people notice is not the ectopic beat itself but what happens immediately after it: the ectopic fires early, the ventricles contract before they have fully filled with blood, and this is followed by a compensatory pause while the heart resets. When the next normal beat arrives, the ventricles have had longer to fill than usual, and the subsequent contraction is noticeably stronger. It is this stronger beat after the pause that people feel most acutely, often described as a thump, a flip, or the heart “banging” in the chest.
Ventricular ectopics can occur in people with or without underlying heart conditions. They become more clinically significant in the presence of structural heart disease, but in an otherwise healthy heart, even frequent ectopics are rarely dangerous.
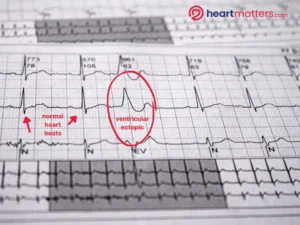
Stress and anxiety can release hormones like adrenaline that increase the likelihood of ventricular ectopics, and those ectopics can in turn worsen anxiety, forming a self-perpetuating cycle. It is important not to hastily attribute palpitations to anxiety alone. A thorough assessment is the right first step, both to identify the true cause and to provide meaningful reassurance.
What Causes Ventricular Ectopic Beats?
Ventricular ectopics have a wide range of triggers, many of which are entirely lifestyle-related and highly modifiable. Identifying which factors apply to you is one of the most practical things to come out of a cardiology assessment.
Stress and anxiety are among the most common contributors. The surge of adrenaline and cortisol that accompanies psychological stress directly lowers the electrical threshold in the heart muscle, making ectopic beats more likely. This creates the cycle described above, ectopics provoke anxiety, anxiety provokes more ectopics, which is one of the reasons that understanding the mechanism is itself therapeutic.
Caffeine is a significant and frequently underestimated trigger. Coffee, tea, energy drinks, and certain medications all contain stimulants that increase cardiac excitability. Many patients notice a clear relationship between their caffeine consumption and the frequency of their ectopics, and a reduction, even a modest one, often makes a meaningful difference. Alcohol is similarly important, particularly in larger quantities or the morning after drinking, when sympathetic nervous system rebound can provoke ectopic activity.
Electrolyte imbalances particularly low potassium, magnesium, or calcium, directly affect the electrical stability of heart muscle cells and are a well-established cause of ectopic beats. These are checked as part of routine blood tests in any assessment of palpitations. Iron deficiency is another commonly overlooked contributor; it increases sympathetic drive and has been associated with higher ectopic frequency, and is easily identified and treated.
Medications deserve specific mention. Salbutamol inhalers used for asthma, decongestants, certain over-the-counter cold remedies, and some antiarrhythmic drugs can all increase ectopic activity as a side effect. If you are on any of these and experiencing frequent ectopics, it is worth discussing with your prescribing doctor whether alternatives might be appropriate.
Hormonal changes particularly during perimenopause, are a frequently underappreciated cause of ventricular ectopics in women. The fluctuation in oestrogen levels affects autonomic nervous system tone and can produce a significant increase in ectopic frequency. These are generally benign but can be very symptomatic, and it is important they are assessed properly rather than dismissed.
Underlying medical conditions including thyroid overactivity chronic lung disease obstructive sleep apnoea and structural heart conditions such as coronary artery disease or cardiomyopathy can all increase ectopic burden. When these are present, managing the underlying condition is the primary focus.
How Ventricular Ectopics Are Assessed
The assessment of ventricular ectopics follows the same careful, systematic approach used for any palpitation complaint, beginning with a detailed history and building toward the investigations most likely to provide useful answers.
I want to understand the full picture: how long you have been noticing the ectopics, how frequently they occur, whether there are identifiable triggers, and crucially, whether they are accompanied by dizziness, chest discomfort, breathlessness, or near-fainting. Those associated symptoms change the clinical urgency of the assessment considerably. A physical examination checks the heart, lungs, and blood pressure, and listens specifically for any murmur or structural abnormality that might be relevant.
An ECG is the first investigation, it takes only a few minutes and can confirm the characteristic appearance of ventricular ectopics, identify their likely origin within the ventricle, and screen for any other electrical abnormalities. Blood tests assess electrolytes, thyroid function, a full blood count including iron studies, and kidney function. A Holter monitor worn over 24 to 48 hours provides a continuous rhythm recording that quantifies the ectopic burden, how many ectopics per day, what patterns they follow, and whether any more sustained arrhythmias are present. For less frequent symptoms, an extended event monitor worn over weeks or months may be arranged instead.
The echocardiogram is particularly important in the assessment of ventricular ectopics. This ultrasound of the heart assesses its structure and pumping function, and the finding of a structurally normal heart with preserved function is one of the most reassuring things I can tell a patient with frequent ectopics. In contrast, ectopics occurring in the context of structural heart disease carry different implications and require more careful management. In selected cases where ectopic burden is very high, generally defined as more than 10–15% of all beats over a 24-hour period, an echocardiogram also provides baseline information about left ventricular function that helps guide the decision about whether any intervention is warranted.
| Investigation | What It Shows | Why It Matters for Ectopics |
|---|---|---|
| ECG | Confirms ectopic morphology and origin | First-line, identifies PVC pattern and screens for other abnormalities |
| Blood tests | Electrolytes, thyroid, iron, kidney function | Identifies treatable triggers |
| Holter monitor | 24–48 hour continuous rhythm recording | Quantifies ectopic burden and identifies patterns |
| Echocardiogram | Heart structure and pumping function | Most important determinant of clinical significance |
| Exercise stress test | Rhythm behaviour during exertion | Useful if ectopics are exercise-related or suppressed by activity |
| Cardiac MRI | Detailed myocardial tissue characterisation | Selected cases, identifies scarring or cardiomyopathy |
| Electrophysiology study (EPS) | Invasive electrical mapping of the heart | Reserved for complex or high-burden cases being considered for ablation |
Reassurance following a thorough clinical assessment and initial investigations plays a crucial role in managing ventricular ectopics. Confirming that the heart is structurally normal and functions well, and explaining that these symptoms frequently resolve without intervention, offers considerable comfort and peace of mind. For many patients, this understanding is itself the most effective treatment.
Management, Starting with Reassurance and Lifestyle
For the majority of patients with ventricular ectopics in a structurally normal heart, the most important management step is proper reassurance, and that reassurance only carries weight when it follows a thorough assessment. Telling someone their ectopics are benign before ruling out structural disease is not reassurance; it is dismissal. Telling them after a normal echocardiogram, a normal Holter result, and normal blood tests is clinically meaningful and genuinely therapeutic.
Beyond reassurance, lifestyle modification is the foundation of management. Reducing caffeine is often the single most impactful change, many patients see a dramatic reduction in ectopic frequency within days of cutting back. Moderating or eliminating alcohol is similarly effective for those in whom alcohol is a clear trigger. Improving sleep quality including investigation for obstructive sleep apnoea if it is suspected, reduces overnight sympathetic tone and can significantly reduce ectopic burden. Stress reduction through regular exercise, mindfulness, and where appropriate psychological support, addresses the adrenaline-driven component of the cycle.
Correcting any identified nutritional deficiencies, particularly low magnesium, potassium, or iron, is straightforward and often effective. Under medical guidance, magnesium supplementation has been found helpful by a number of patients with frequent ectopics, and is generally well tolerated.
When Medication Is Considered
Medication is not routinely required for ventricular ectopics in a structurally normal heart, but it has a role when symptoms are significantly affecting quality of life and lifestyle measures have been insufficient.
Beta blockers are the most commonly used agent, they blunt the adrenaline response, reduce heart rate, and diminish the perceived intensity of ectopic beats. Many patients find that even a low dose makes the ectopics considerably less noticeable, even if it does not eliminate them entirely. Calcium channel blockers such as verapamil or diltiazem offer an alternative for those who cannot tolerate beta blockers. In selected patients with a high ectopic burden that is causing symptoms or affecting cardiac function, antiarrhythmic medications may be considered under specialist guidance.
Catheter Ablation for Ventricular Ectopics
For patients with a very high ectopic burden, typically greater than 10–15% of all beats, particularly where this is causing symptoms or beginning to affect left ventricular function, catheter ablation is an increasingly used and highly effective option. The procedure uses radiofrequency energy or cryotherapy delivered via a catheter to identify and eliminate the specific focus in the ventricle responsible for generating the ectopic beats.
Success rates for ablation of ventricular ectopics are high when the focus is clearly identified and accessible, and the procedure can be curative in many cases. It is typically performed under sedation, requires a short hospital stay, and recovery is generally quick. The decision to proceed with ablation is made on an individual basis weighing symptom burden, ectopic frequency, and patient preference, it is not routinely offered for occasional or mildly symptomatic ectopics.
- Very high ectopic burden more than 10–15% of beats on a Holter monitor, may warrant closer monitoring of cardiac function over time.
- Ectopics with structural heart disease coronary artery disease, cardiomyopathy, or valve disease, carry different implications and require specialist assessment.
- Ectopics with associated symptoms dizziness, near-fainting, chest pain, or breathlessness during episodes, should always be assessed promptly.
- Runs of ectopics three or more consecutive ventricular beats, may represent a short run of ventricular tachycardia and require prompt evaluation.
Heart Matters Resource
When in Doubt, Get Checked Out
If your symptoms are new, changing, or accompanied by anything that concerns you, please do not hesitate to seek assessment. Heart Matters has a dedicated resource covering the symptoms that should never be ignored and why getting checked is always the right call.
Conclusion
Ventricular ectopic beats are among the most common findings in cardiology, and among the most reassuring, once properly assessed. The vast majority of people with frequent ectopics and a structurally normal heart can be offered clear, evidence-based reassurance that their symptoms, while real and sometimes bothersome, do not reflect a dangerous condition.
What makes the difference is a thorough assessment rather than a dismissive one. An ECG, a Holter monitor, an echocardiogram, and a careful review of potential triggers gives both patient and cardiologist the information needed to make that reassurance meaningful, and to identify the small proportion of cases where closer monitoring or treatment is genuinely warranted.
If you have been told you have ventricular ectopics and have questions about what that means for you, please do speak with your doctor or cardiologist. Understanding what is happening in your heart is the first step toward feeling better about it.
More from Heart Matters
- Understanding Palpitations: A Cardiologist’s Approach
- The Electrocardiogram (ECG): What It Shows and Why It Matters
- Understanding the Holter Monitor Test
- Cardiac Monitoring Devices: From Holter Monitors to Loop Recorders
- Chest Pain: Causes, Symptoms, and When to Seek Help
- When in Doubt, Get Checked Out, Heart Matters Resource