- An ECG records the heart’s electrical activity through electrodes placed on the skin, it is quick, painless, and one of the most informative tests in cardiology.
- It can detect arrhythmias, evidence of a heart attack, conduction abnormalities, and changes that suggest the heart is under strain.
- A normal ECG does not rule out all cardiac conditions, some problems are intermittent and will not be captured on a resting trace.
- The ECG is the starting point for almost every cardiac investigation, understanding what it shows helps make sense of everything that follows.
If you have ever had a cardiac symptom investigated, you have almost certainly had an ECG. It is the most widely performed cardiac test in the world, done in emergency departments, GP surgeries, pre-operative assessments, and cardiology clinics millions of times every day.
Despite its ubiquity, most people who have an ECG have little idea what it is actually measuring, what the trace means, or what it can and cannot tell their doctor. Understanding the basics changes that, and makes every subsequent cardiac conversation more meaningful.
What to Expect
Duration
5–10 minutes from preparation to completion
Preparation
No special preparation required. Avoid lotions on the chest on the day.
Comfort
Completely painless. You will need to lie still briefly while the trace is recorded.
Radiation
None. The ECG only records electrical signals, it does not emit anything.
Results
Often reviewed immediately. A formal report is typically available within hours to days.
What Is an ECG?
The heart’s electrical system
Every heartbeat is triggered by an electrical impulse that originates in the sinus node, the heart’s natural pacemaker, and travels in a precise sequence through the heart muscle, coordinating the contraction of the upper chambers (atria) followed by the lower chambers (ventricles).
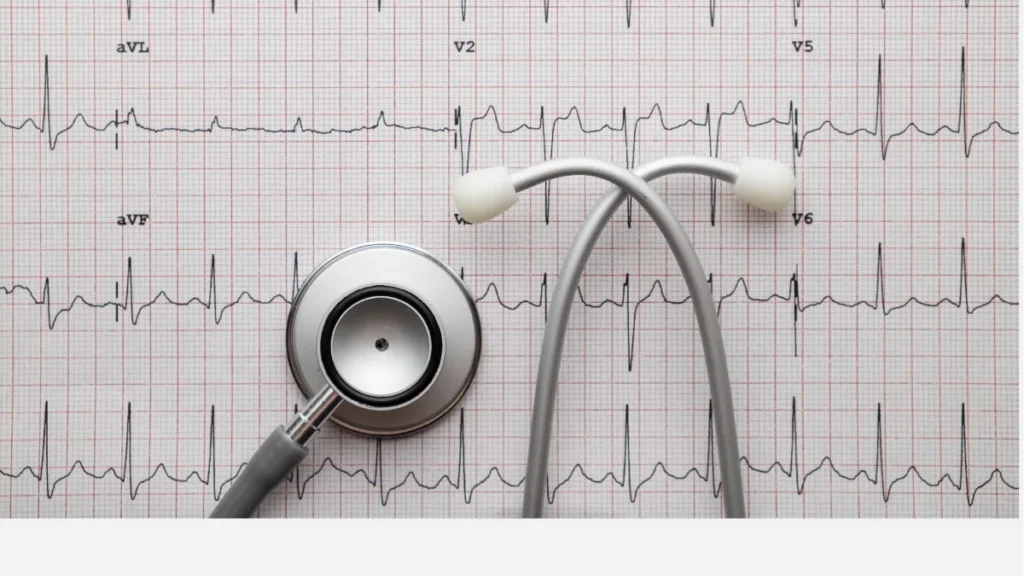
An ECG, electrocardiogram, detects and records these electrical signals through electrodes placed on the skin of the chest, arms, and legs. It does not emit any radiation or electricity. It simply listens, measuring the tiny electrical changes at the skin surface that correspond to the electrical activity within the heart.
What the trace shows
The ECG produces a characteristic waveform for each heartbeat. The main components each represent a specific electrical event.
| Wave | What it represents | What abnormalities can suggest |
|---|---|---|
| P wave | Electrical activation of the atria | Atrial enlargement, AF, conduction delay |
| PR interval | Conduction time from atria to ventricles through the AV node | Heart block, pre-excitation (WPW) |
| QRS complex | Electrical activation of the ventricles | Bundle branch block, ventricular hypertrophy, heart attack |
| ST segment | Period between ventricular activation and recovery | Acute heart attack, ischaemia, pericarditis |
| T wave | Electrical recovery of the ventricles | Ischaemia, electrolyte disturbance, Long QT |
| QT interval | Total ventricular electrical cycle time | Long QT syndrome, drug effects |
What an ECG Can Detect
Heart rhythm and rate
The ECG immediately reveals the heart rate and whether the rhythm is regular or irregular. Atrial fibrillation, SVT, heart block, and bradycardia are all immediately apparent on the trace. For many arrhythmias, the ECG is the definitive diagnostic test.
Evidence of heart attack
Changes in the ST segment and T waves, and the development of abnormal Q waves, provide evidence of acute or previous heart attack. In a patient with chest pain, the ST segment of the ECG is one of the most important pieces of information available, because ST elevation in the right pattern indicates a STEMI, a type of heart attack requiring immediate intervention.
Conduction abnormalities
Bundle branch blocks, heart block of varying degrees, and pre-excitation patterns such as Wolff-Parkinson-White syndrome all have characteristic ECG appearances that allow identification without any further testing.
Structural clues
Voltage changes in the QRS complex can suggest left ventricular hypertrophy, thickening of the heart muscle from longstanding high blood pressure or aortic stenosis. The ECG cannot measure heart muscle thickness directly, that requires an echocardiogram, but it can raise the suspicion.
I often tell patients that the ECG is like a photograph of the heart’s electrical activity at one moment in time. It is extraordinarily useful, but if the arrhythmia or the problem is not happening at that moment, the trace will look normal. A normal ECG does not mean nothing is wrong. It means nothing was wrong at that particular moment.
What an ECG Cannot Tell You
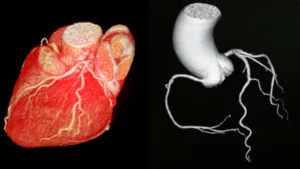
This is just as important to understand as what it can show. A normal resting ECG does not exclude an intermittent arrhythmia, SVT, paroxysmal AF, or VT will only appear on the trace when they are actively occurring. It does not provide information about coronary artery anatomy or the degree of stenosis, that requires angiography or CT coronary angiography. It does not measure ejection fraction or valve function, those require echocardiography.
The ECG is the starting point. What follows depends on what it shows, and what the clinical picture suggests.
Variants of the ECG
Holter monitor
A Holter monitor is a portable ECG device worn continuously for 24 to 48 hours, recording every heartbeat throughout the day and night. It is used to capture intermittent arrhythmias that are not present on a resting ECG, palpitations, dizziness, or unexplained fainting that occurs during daily activities.
Exercise stress ECG
The exercise stress test, also called an exercise tolerance test (ETT), records the ECG continuously while the patient exercises on a treadmill or exercise bike. The heart’s response to increasing workload can reveal ischaemia, arrhythmias provoked by exercise, and abnormal blood pressure responses that are not apparent at rest. We have a dedicated article on the exercise stress test on Heart Matters.
Event recorder and implantable loop recorder
For very infrequent symptoms, a longer-term event recorder worn for weeks allows the patient to press a button during an episode to transmit a recording. An implantable loop recorder, a small device inserted just under the skin, monitors heart rhythm continuously for up to three years, capturing events that would otherwise be impossible to document.
- Was my ECG normal, and if not, what specifically was abnormal?
- Does a normal ECG mean my palpitations or dizziness are definitely not cardiac?
- Should I have a Holter monitor to capture symptoms that occur intermittently?
- What does the ECG show about my heart rhythm specifically?
- Are there any findings that need further investigation, and what would that involve?
Heart Matters Resource
When in Doubt, Get Checked Out
If you have symptoms, palpitations, dizziness, chest discomfort, or unexplained breathlessness, that have not yet been investigated with an ECG, getting one is the right first step. It takes minutes and provides your doctor with immediate, valuable information.
Conclusion
The ECG is the cornerstone of cardiac investigation, fast, safe, informative, and available everywhere. Understanding what it measures and what it can and cannot show transforms it from a mysterious printout into a meaningful piece of clinical information you can discuss intelligently with your doctor.
If you have had an ECG and been told it is normal, that is genuinely reassuring, but it does not rule out every cardiac cause of your symptoms. If it is abnormal, understanding which component is abnormal and what that means is the right next conversation to have.
The ECG opens the door. What comes next depends on what it shows.