Discover how your heart works, one beat at a time — empowering you to better understand your condition and have more informed conversations with your doctor.
Clinically reviewed content for patients, families and carers.
Your heart muscle — the myocardium — works continuously, every minute of every day, without ever needing to rest.
When the heart contracts and pushes blood out to the body and lungs.
When the heart relaxes and refills with blood, ready for the next beat.
When doctors talk about your "heart function," they're usually referring to how well these two phases — squeeze and fill — are working. Both matter equally to your quality of life.
Heart contraction and relaxation
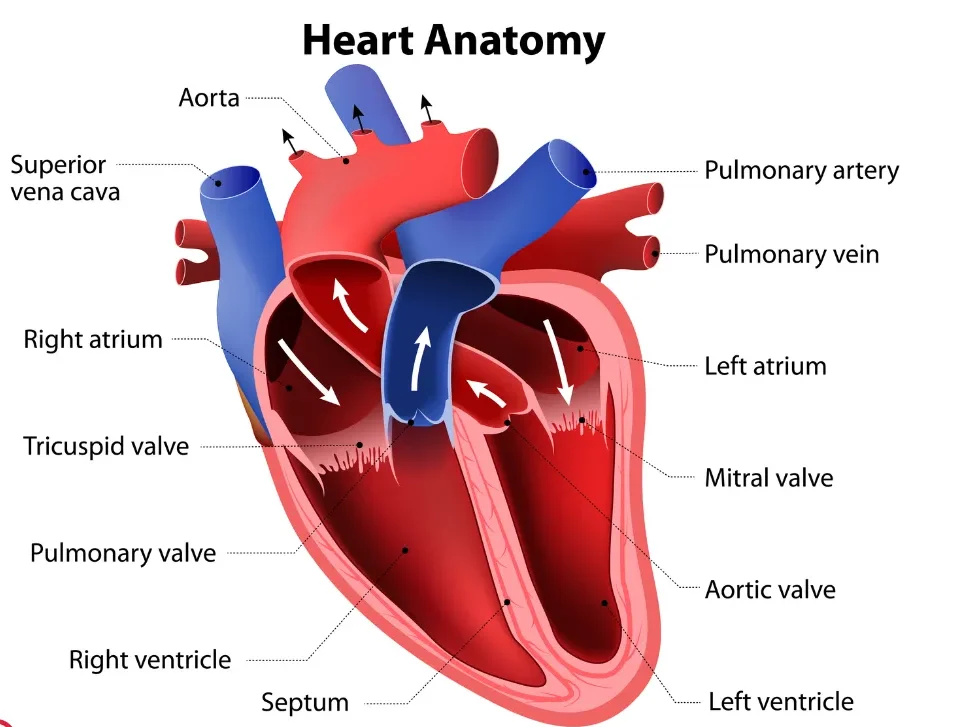
Think of your four heart valves as one-way doors — they open to let blood through, then snap shut to stop it flowing backwards.
Between the right atrium and right ventricle.
Between the right ventricle and the pulmonary artery (to the lungs).
Between the left atrium and left ventricle. Also called the bicuspid valve.
Between the left ventricle and the aorta — the main artery to the body.
If you've been told you have a valve problem, it usually means a valve has become narrowed (stenosis) or is leaking (regurgitation). Both affect how efficiently your heart pumps — but many cases are mild and need only monitoring.
Heart valve animation
That familiar "lub-dub" is the sound of your heart valves closing — and what doctors hear through a stethoscope tells them a great deal about how your heart is working.
Mitral & tricuspid valves close — start of systole.
Aortic & pulmonary valves close — start of diastole.
Being told you have a murmur can sound alarming — but most are harmless. Always ask your doctor whether it needs monitoring or further investigation.

Like any muscle, your heart needs its own blood supply — and that's exactly what the coronary arteries provide, wrapping around the outside of the heart.
Supplies the front of the heart. Often called the "widow maker" — blockage here is a leading cause of heart attack.
Wraps around the left side of the heart, supplying the side and back walls.
Supplies the right ventricle and part of the heart's electrical system.
If your doctor has mentioned a "blocked artery" or "stent," they are referring to one of these three vessels. The specific artery involved helps determine how the condition is managed.
Coronary artery anatomy
Every heartbeat starts as an electrical signal — a precisely timed spark that travels through the heart in a fraction of a second, triggering a coordinated contraction.
Fires the electrical impulse that starts each heartbeat. Located in the upper right atrium.
Introduces a brief, deliberate pause — giving the upper chambers time to empty before the ventricles contract.
Carry the signal to the ventricular walls, triggering a powerful, coordinated contraction.
An ECG records this electrical activity. Abnormal rhythms — called arrhythmias — occur when this pathway is disrupted. A pacemaker device can take over if the SA node isn't working properly.
Cardiac conduction system
The heart's four chambers form two pumps working in perfect sync — the right side sends blood to the lungs to collect oxygen, and the left side drives that oxygen-rich blood out to the rest of the body.
Receives oxygen-poor blood returning from the body.
Receives oxygen-rich blood returning from the lungs.
Pumps blood to the lungs via the pulmonary artery.
The main pump — drives blood through the aorta to the entire body.
The left ventricle does most of the work. When doctors measure your ejection fraction, they are assessing how strongly this chamber squeezes with each beat. A normal ejection fraction is 50% or above.
Surrounding the heart is a protective double-layered sac called the pericardium — think of it as the heart's shock absorber.
The tough outer layer that anchors the heart in place and prevents it from overfilling.
A thin inner layer that produces lubricating fluid, preventing friction as the heart beats continuously.
Conditions that can affect the pericardium:
Pericarditis causes sharp chest pain that often feels worse lying flat and better sitting forward. It is usually treatable with anti-inflammatory medication.

Now that you understand how the heart works, explore our conditions library, diagnostic tests section, and medications hub — all written in the same plain language.
The content on heartmatters.com is for general educational purposes only and is not a substitute for medical advice. Always consult your doctor or a qualified healthcare professional about any medical concerns.