Key Points
- Furosemide is a powerful diuretic, a water or fluid tablet, used to remove excess fluid from the body in conditions such as heart failure, kidney disease and liver disease.
- It works quickly and effectively, and is one of the most widely prescribed medications in cardiovascular medicine.
- The most noticeable effect is a significant increase in urine output, which is the intended action of the medication.
- Furosemide is typically taken in the morning, and sometimes again at midday if a second dose is needed. Taking it too late in the day can cause disruptive overnight urination.
- The dose varies considerably between individuals. Some people need small doses while others require much larger amounts to achieve the same effect.
- Regular monitoring of kidney function and electrolytes is an important part of long term furosemide use.
If you have been prescribed furosemide, you are in very good company. It is one of the most commonly used medications in cardiology and general medicine, and for good reason. It is highly effective at doing something that is genuinely important for many heart conditions: removing excess fluid from the body.
This article explains what furosemide is, why it is prescribed, what to expect when taking it, and what patients often find most surprising about this medication.
What Is Furosemide?
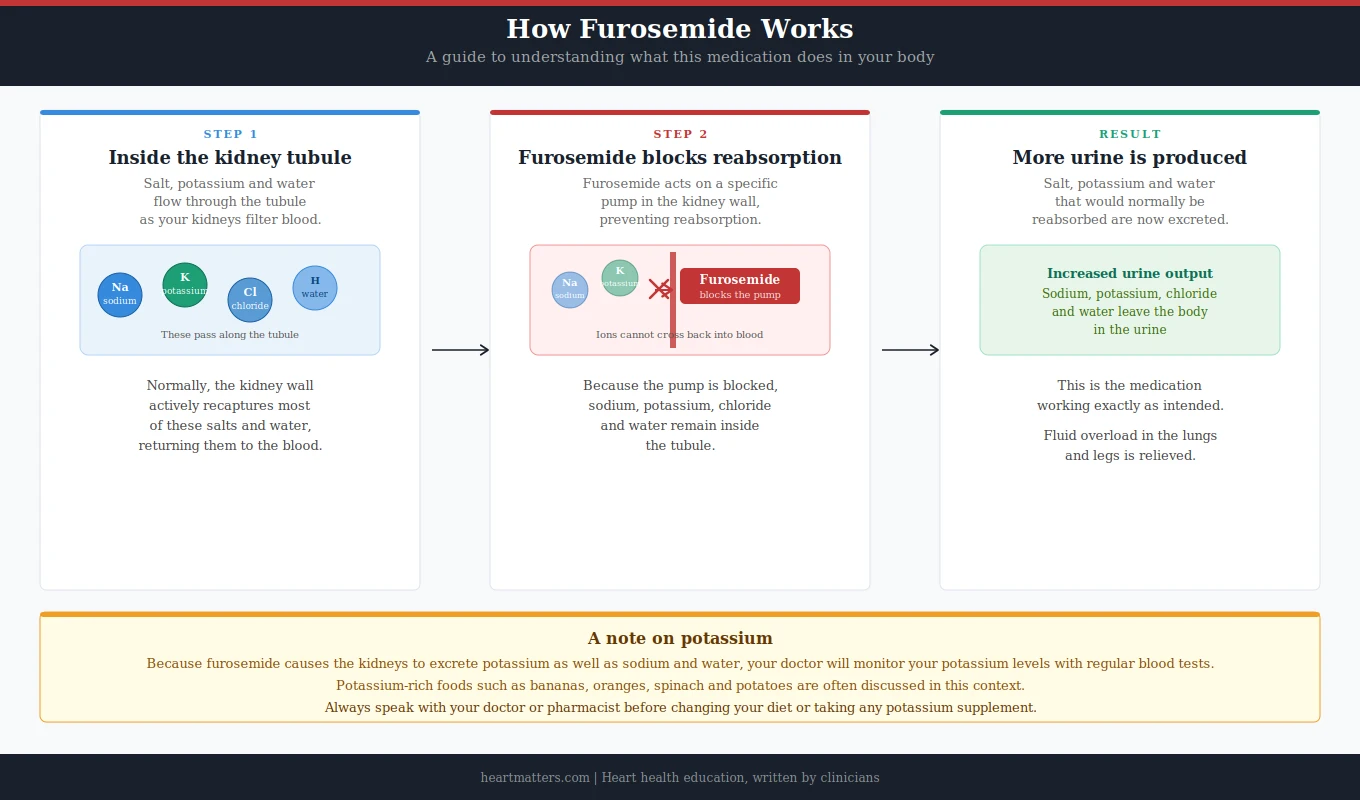
Furosemide is a diuretic, commonly known as a water or fluid tablet. It works by acting on the kidneys, specifically on a part of the kidney called the loop of Henle, which is why furosemide and medications like it are also called loop diuretics.
Its job is to tell the kidneys to excrete more salt and water into the urine than they otherwise would. The result is a significant increase in urine output, which reduces the total amount of fluid in the body. This is not a side effect, it is the intended action of the medication.
Why Is It Prescribed?
Furosemide is prescribed whenever excess fluid has accumulated in the body and needs to be removed. This most commonly occurs in:
Heart failure. When the heart is not pumping as efficiently as it should, fluid can back up and accumulate in the lungs, the abdomen, and the legs. This congestion causes breathlessness, swollen ankles, and fatigue. Furosemide is a cornerstone of heart failure treatment because it directly addresses this fluid overload.
Kidney disease. Damaged kidneys do not excrete fluid as effectively, leading to fluid retention that furosemide can help manage.
Liver disease. Liver conditions such as cirrhosis can cause large amounts of fluid to accumulate in the abdomen, a condition called ascites. Furosemide is often used alongside another diuretic called spironolactone in this setting.
High blood pressure. Furosemide is occasionally used for blood pressure control, though other medications are more commonly chosen for this purpose.
Names Around the World
Furosemide is known by a number of different names depending on where you are and whether you are taking the generic or a branded version.
Generic name. Furosemide is the name used in Australia, the United Kingdom, the United States, Europe and most of the world. In some countries, and on older Australian and British prescriptions, it may be spelled frusemide. Both refer to exactly the same medication.
Common brand names include:
- Lasix, the most widely recognised brand globally, used in Australia, the United States, the United Kingdom and many other countries
- Frusid, used in Australia
- Uremide, available in Australia
- Frusehexal, available in Australia
- Diural, used in some European countries
- Seguril, used in Spain
- Lasilix, used in France
Furosemide or Frusemide? They Are the Same Medication
If your doctor says frusemide, your old prescription says frusemide, or you have always known it by that name, you are not mistaken. Frusemide was the official approved name in Australia, the United Kingdom and most Commonwealth countries when the medication was first introduced in the 1960s.
In 2003 the United Kingdom and Australia officially adopted the international name furosemide, in line with the World Health Organization. Changing what an entire generation of clinicians had been saying and writing for decades takes considerably longer than a regulatory update, and you will hear both names used interchangeably in hospitals and clinics to this day.
If you travel internationally and need to continue your medication, the generic name furosemide will be understood by pharmacists in most countries, even if the brand name differs.
Available Formulations and Doses
Furosemide is available in several different forms, each suited to different clinical situations.
Tablets are the most commonly prescribed form for ongoing outpatient treatment. The standard tablet strengths available in Australia include:
- 20mg, often used as a starting dose or for mild fluid retention
- 40mg, the most commonly prescribed strength for heart failure and fluid management
- 500mg, a high strength tablet sometimes known as Lasix 500. This strength is generally reserved for patients with advanced heart failure, significant diuretic resistance, or severe kidney disease, and is typically prescribed under the guidance of a cardiologist, heart failure specialist or nephrologist. It is not a first line dose and requires careful monitoring of kidney function and electrolytes.
Oral liquid preparations are available for patients who have difficulty swallowing tablets or who need a dose that falls between standard tablet strengths.
Intravenous and intramuscular injections are used in hospital settings when rapid or potent diuresis is needed. When someone is admitted with acute heart failure or severe fluid overload, furosemide given directly into a vein works within minutes and produces a much more immediate and powerful effect than the oral tablet. In hospital, furosemide can also be given as a continuous infusion through a drip when very large amounts of fluid need to be removed over a sustained period.
What to Expect When You Take It
The most immediate and noticeable effect of furosemide is a substantial increase in urination. This typically begins within 30 to 60 minutes of taking the medication and can produce a large volume of urine over several hours. For patients who are significantly fluid overloaded when they first start furosemide, the volume of urine produced can be quite striking.
This increase in urinary frequency and volume is not a problem. It is the medication working exactly as intended. The medical term for the passage of abnormally large volumes of urine is polyuria, and it is an expected feature of diuretic therapy, particularly in the early stages of treatment or after a dose increase.
As the excess fluid is removed from the body over days to weeks, the degree of diuresis typically settles to a more manageable level while the medication continues to prevent fluid from reaccumulating.
When to Take Furosemide
Timing matters with furosemide. Because the medication produces its diuretic effect within an hour of being taken, most doctors prescribe it to be taken in the morning. This way the period of increased urination occurs during waking hours rather than disrupting sleep.
When a larger total daily dose is needed, a second dose is typically prescribed at midday rather than in the afternoon or evening. Taking furosemide too late in the day means its peak diuretic effect will occur in the evening or overnight, which can significantly disrupt sleep with repeated trips to the bathroom.
If you are prescribed furosemide twice daily and find your sleep is being disrupted, it is worth discussing the timing of your second dose with your doctor. A simple adjustment in timing can make a considerable difference to quality of life without changing the total dose.
Why Doses Vary So Much Between Individuals
One of the things that surprises many patients is the wide range of doses that different people need. Furosemide doses can range from as little as 20 milligrams once daily to several hundred milligrams per day in some patients.
The range of daily furosemide doses used in clinical practice. The dose that is right for you depends on your kidney function, the severity of fluid overload, and how your body responds.
The reason for this variation is not simply about the severity of the underlying condition. Some people have what is called diuretic resistance, where the kidneys respond less efficiently to furosemide. This can occur in people with impaired kidney function, in those who have been on diuretics for a long time, and in some other clinical situations.
In these cases, larger doses are needed to achieve the same degree of fluid removal that a much smaller dose would produce in someone without resistance.
This is also why furosemide doses are sometimes changed over time. A dose that was very effective initially may need to be adjusted as circumstances change. Some patients find their dose increases during periods when their heart failure is less well controlled and then reduces again once things improve. This is entirely expected and is part of the way furosemide is used in clinical practice.
Monitoring While on Furosemide
Because furosemide affects the kidneys and the balance of electrolytes in the body, regular blood tests are an important part of long term treatment. The main things your doctor will monitor include:
Kidney function. Furosemide can sometimes reduce blood flow to the kidneys, particularly if the body becomes too dry from excessive diuresis. Regular checks ensure the kidneys are tolerating the medication well.
Potassium. Furosemide causes the kidneys to excrete potassium along with salt and water. Low potassium, called hypokalaemia, is one of the more common complications of long term furosemide use and can cause muscle cramps, weakness, and in more serious cases affect heart rhythm. Many patients on furosemide are also prescribed a potassium supplement or a potassium sparing diuretic such as spironolactone for this reason.
Sodium. Less commonly, furosemide can affect sodium levels, which your doctor will also keep an eye on.
What Patients Often Ask
Can I skip a dose if I am going out? This is one of the most common questions. Missing an occasional dose to manage a social commitment is understandable, but doing so regularly or skipping doses frequently can allow fluid to reaccumulate. It is worth having a conversation with your doctor about how to best manage furosemide around your lifestyle.
Will I always need it? This depends entirely on the underlying condition. Some patients take furosemide for a defined period and then stop. Others, particularly those with ongoing heart failure or chronic kidney disease, take it long term as part of their regular medication regimen.
What if I feel very thirsty or dizzy? These can be signs that the body has become too dry, sometimes called volume depletion. If you experience significant thirst, dizziness on standing, or a marked reduction in urine output, contact your doctor rather than simply drinking more fluid, as the dose may need adjustment.
The Importance of a Regular Medication Review
Furosemide does not work in isolation. Most people taking it are also prescribed several other medications for their heart, kidneys, or blood pressure, and many of these can interact with furosemide in ways that affect how the body responds.
A number of commonly prescribed medications can affect electrolyte levels, kidney function, or blood pressure when taken alongside furosemide. These include other blood pressure medications, certain pain relievers, some antibiotics, and a range of other cardiac medications. This is not a reason for concern, but it is a reason for awareness.
A regular medication review with your doctor and pharmacist is genuinely valuable for anyone taking furosemide long term. A pharmacist in particular is well placed to look across your entire medication list and identify any combinations that may warrant closer monitoring or a timing adjustment. This kind of review is not about finding problems, it is about making sure every medication you take is working as well as it possibly can.
It is also worth letting any new doctor, specialist or hospital team know that you are taking furosemide, particularly if you are prescribed a new medication, are unwell with vomiting or diarrhoea, or are preparing for a procedure. These are all situations where a temporary adjustment to your furosemide dose may be appropriate.
Heart Matters Resource
Ask About a Home Medicines Review
If you are taking furosemide alongside three or more other regular medications, you may be eligible for a Home Medicines Review with an accredited pharmacist, fully covered by Medicare. It is one of the most underused resources in Australian primary care and one of the most useful for people on long term cardiac medication.
Conclusion
Furosemide is one of the most important and widely used medications in cardiovascular and kidney medicine. For many people it makes an enormous difference to daily comfort and quality of life, removing the excess fluid that makes breathing difficult and legs heavy.
If you are taking furosemide, the most important things to stay on top of are your regular blood tests, the timing of your doses, and an open conversation with your doctor or pharmacist whenever something changes. A medication review is not something to put off.
You are not alone in managing this. The team looking after you has prescribed furosemide many times and knows how to adjust it as your needs change. If something does not feel right, ask.
This article provides general information only and is not medical advice. Any decisions about your medication, dose or monitoring should be made in conversation with your cardiologist, GP or pharmacist.