- A coronary stent is a tiny expandable mesh tube, typically 8 to 48 mm long and 2 to 5 mm in diameter, made from medical-grade metal alloy, designed to hold a narrowed artery open permanently.
- Stents are delivered on a long, flexible catheter threaded from the wrist to the heart, then deployed by inflating a small balloon that presses the stent firmly against the artery wall.
- Most stents used today are drug-eluting stents (DES) coated with medication released slowly over weeks to reduce the risk of the artery re-narrowing.
- After stenting, dual antiplatelet therapy (DAPT) typically aspirin plus ticagrelor or clopidogrel, is essential while the stent heals safely into the artery wall.
- A stent treats the narrowing caused by atherosclerosis, but not the underlying disease. Ongoing medication and lifestyle management remain just as important.
Most people who have had a coronary stent placed have never actually seen one. They know something small was put in an artery near their heart, that it involved a tube at the wrist, and that it seemed to help, but the details tend to remain a mystery.
This article opens the box. Understanding what a stent is, how it is designed, and how it is delivered helps make sense of your recovery, your medications, and why your follow-up care matters as much as the procedure itself.
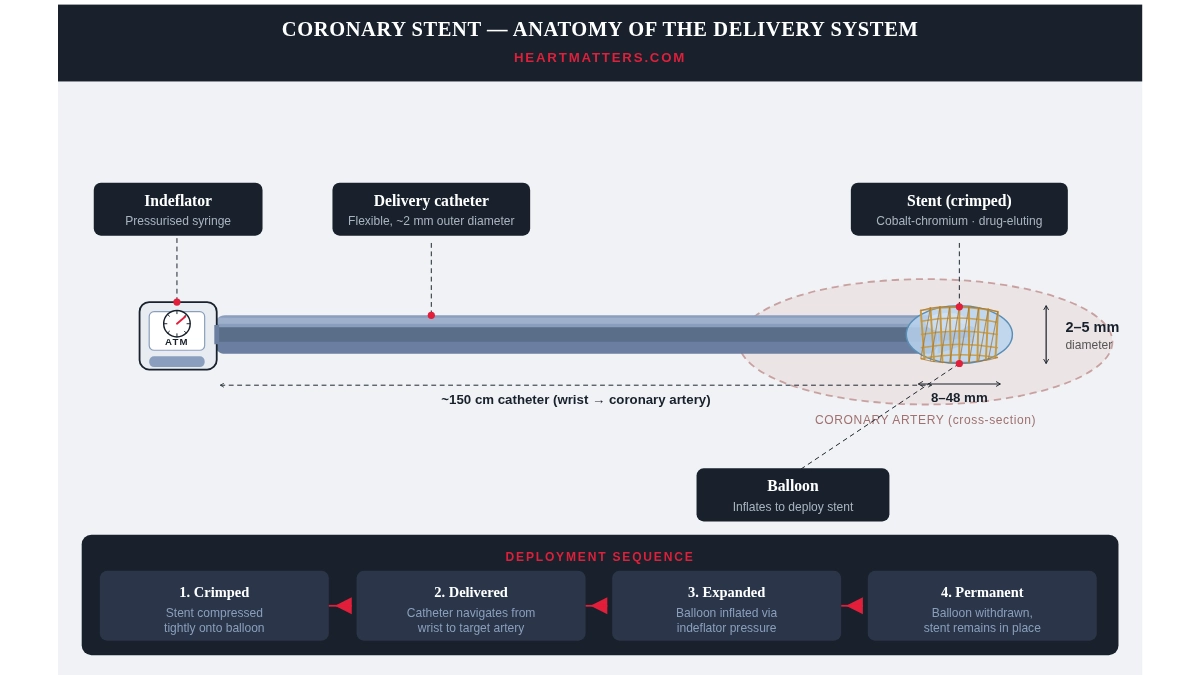
What Is a Coronary Stent?
A coronary stent is a small, expandable mesh tube made from medical-grade metal alloy, most commonly cobalt-chromium or platinum-chromium. These materials are chosen for their combination of strength, flexibility, radiopacity (visibility under X-ray), and biocompatibility, the ability to sit inside the body long-term without causing a reaction.
In terms of size, stents are remarkably small. They typically range from 8 to 48 millimetres in length and between 2 and 5 millimetres in diameter, with the exact dimensions chosen to match the specific artery being treated.
Despite their delicate appearance, they are engineered to withstand the continuous mechanical stress of a beating heart and pulsating blood flow for decades.
The purpose of the stent is to act as a permanent scaffold. When a coronary artery narrows due to the buildup of atherosclerotic plaque, blood flow to the heart muscle is reduced. During a procedure called percutaneous coronary intervention (PCI) a balloon compresses the plaque and widens the artery, and the stent is then deployed to hold it open permanently.
Bare Metal vs Drug-Eluting Stents
Not all stents are identical. The most important distinction is between bare metal stents and drug-eluting stents, and understanding the difference helps explain why you receive the medications you do after the procedure.
| Feature | Bare Metal Stent (BMS) | Drug-Eluting Stent (DES) |
|---|---|---|
| Coating | Plain metal, no drug coating | Polymer coating containing antiproliferative medication |
| How it works | Holds artery open mechanically | Holds artery open and releases drug to prevent re-narrowing |
| Risk of restenosis | Higher, tissue overgrowth more likely | Lower, drug suppresses excessive tissue growth |
| DAPT duration | Typically 4 weeks minimum | Typically 6–12 months (longer after heart attack) |
| Current use | Rarely used, largely superseded by DES | Standard of care for the vast majority of cases |
The drug coating on a modern drug-eluting stent, typically an antiproliferative agent such as everolimus, zotarolimus, or sirolimus, is released gradually over several weeks to months. Its purpose is to suppress the natural healing response of the artery wall, which, if excessive, can cause tissue to grow back inside the stent and re-narrow it, a process called in-stent restenosis.
By inhibiting this overgrowth, drug-eluting stents have dramatically reduced restenosis rates compared to their bare metal predecessors. In most parts of the world, bare metal stents are no longer implanted.
What’s in the Box, The Delivery System
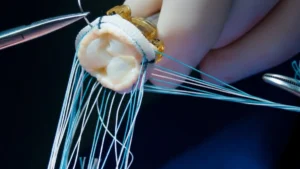
A stent does not arrive in the catheter laboratory as a standalone device. It comes as part of a carefully engineered delivery system, sterile-packaged and ready for single use. Opening that package reveals considerably more than the stent itself.
The stent is pre-mounted onto the tip of a long, flexible delivery catheter typically around 150 centimetres in length. This length is necessary so the catheter can travel from the access point at the wrist, through the arterial system, around the aortic arch, and into the coronary arteries near the heart.
Before packaging, the stent undergoes a process called crimping in which specialised equipment compresses it tightly onto a small balloon at the catheter tip. This reduces the stent’s profile enough to pass through the arterial system without disrupting blood flow.
The catheter itself is colour-coded and labelled, indicating the stent’s length, diameter, drug coating type, and expiry date. Every detail is checked before the package is opened in the catheter laboratory.
The Role of the Indeflator
One of the less glamorous but critically important components of the delivery system is a handheld device called an indeflator. This is a syringe with a built-in pressure gauge that allows the operator to inflate the balloon at the catheter tip with precise, measured pressure, expressed in atmospheres.
When the balloon is inflated, it expands outward, pressing the stent firmly against the artery wall and opening it to its full diameter. The pressure and duration of inflation are carefully controlled to ensure the stent is fully expanded and well-seated against the vessel wall.
Once expansion is confirmed under X-ray guidance, the balloon is deflated and withdrawn, leaving the stent permanently in place.
The stent itself weighs a fraction of a gram and is invisible to the naked eye when crimped onto the catheter. What surrounds it, the delivery system, the imaging technology, the indeflator, the sterile packaging, represents decades of engineering refinement designed to get this tiny device safely from a wrist puncture to a coronary artery a metre and a half away.
After Deployment, What Happens Next
Once deployed, the stent becomes a permanent part of the artery. Over the following weeks, a thin layer of the body’s own tissue, called neointima grows over the metal struts of the stent, incorporating it into the artery wall. This process is called endothelialisation.
During the weeks and months while this healing is occurring, the exposed metal surface of the stent is a potential site for platelet aggregation and clot formation. This is why dual antiplatelet therapy (DAPT) aspirin combined with ticagrelor or clopidogrel, is prescribed for a defined period after stenting.
These medications prevent platelets from sticking to the stent surface and forming a clot, a complication called stent thrombosis which, if it occurs, can cause a serious heart attack.
The duration of DAPT depends on the clinical situation, typically around 12 months after a heart attack, and potentially shorter in elective cases. It must never be stopped without first discussing it with your cardiologist. Even a brief interruption in the early weeks after stenting carries real risk.
- Your stent is permanent, it does not need to be replaced or removed.
- Do not stop your antiplatelet medications (aspirin, ticagrelor, or clopidogrel) without speaking to your cardiologist first, even if another doctor recommends it for a procedure.
- A stent treats the narrowing but not the underlying atherosclerosis. Continued medication and lifestyle management are essential to protect the rest of your arteries.
- Modern stents are MRI-compatible, you can safely have an MRI scan. Always inform the radiologist that you have a stent.
- You will receive a stent card with your device details, keep this with you, particularly when travelling.
Heart Matters Resource
Coronary Artery Disease, The Full Picture
Our dedicated CAD resource covers the coronary arteries in depth, including how blockages develop, what stents do, the medications used, and Prof. Barlis’s research into plaque using optical coherence tomography.
Heart Matters Resource
When in Doubt, Get Checked Out
If you have had a stent placed and experience any new chest discomfort, breathlessness, or symptoms that concern you, do not wait to see if they settle. Getting checked is always the right call.
Conclusion
Opening the box of a coronary stent reveals something remarkable, a device smaller than a fingernail, designed to last a lifetime inside one of the body’s most demanding mechanical environments.
The engineering behind every component, and the decades of clinical research that have refined the drug coatings, alloy compositions, and deployment techniques, are what make modern PCI so effective.
If you have had a stent placed, understanding what it is and what it is doing helps make sense of why your medications matter, why follow-up appointments are important, and why the lifestyle changes your team recommends are not optional extras, they are the long-term protection that the stent itself cannot provide.