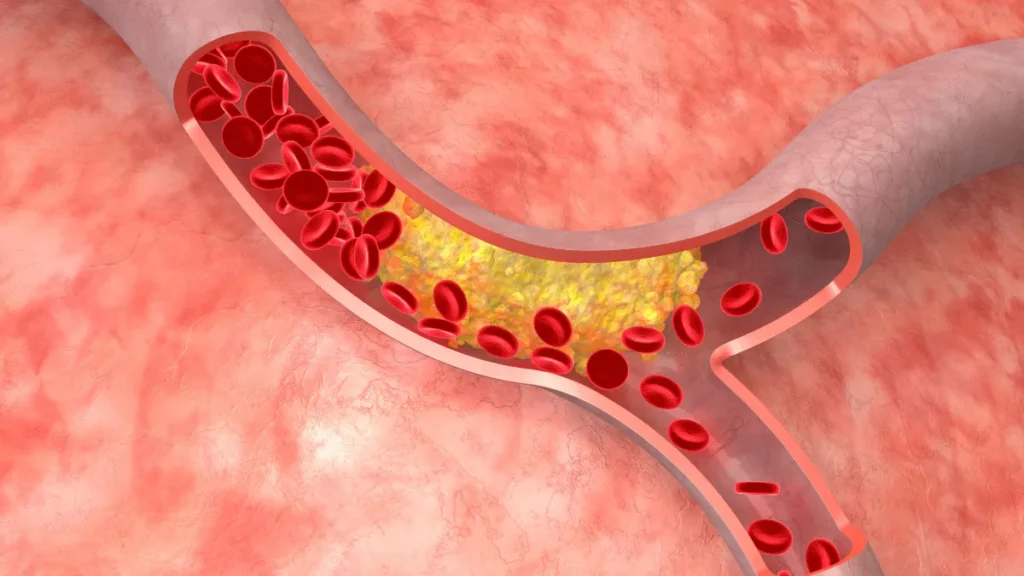
- Atherosclerosis is the gradual buildup of plaque inside the walls of arteries, a process that begins silently, often decades before any symptoms appear.
- It is the underlying cause of most heart attacks, strokes, and angina. Understanding it is central to understanding cardiovascular disease.
- The process is driven by a combination of inflammation, cholesterol, and damage to the artery wall all of which are influenced by risk factors many of us can modify.
- Atherosclerosis progresses slowly and silently, but it is neither inevitable nor untreatable. Lifestyle changes and medication can significantly slow or stabilise it.
- The earlier risk factors are identified and managed, the greater the opportunity to protect the arteries and reduce the likelihood of a cardiovascular event.
If there is one process that sits at the heart of most cardiovascular disease, it is atherosclerosis. It is the reason coronary arteries narrow. It is the reason plaques can rupture and trigger a heart attack. It is the reason strokes occur when the same process affects the arteries supplying the brain. And yet most people have never heard the word, or have only encountered it in passing, in a hospital letter, a discharge summary, or a conversation with a doctor who didn’t have quite enough time to explain it properly.
This article is an attempt to fill that gap. Atherosclerosis is not a mysterious or obscure condition, it is a well-understood biological process with well-established drivers, and one that responds meaningfully to the choices we make about how we live and how we manage our health.
What Is Atherosclerosis?
Atherosclerosis is a chronic disease of the arteries. It develops when fatty substances, cholesterol, inflammatory cells, calcium, and other debris accumulate within the walls of the arteries, forming deposits called plaques. Over time, these plaques grow and harden, causing the arteries to narrow and lose their normal flexibility. As the narrowing progresses, blood flow through the affected artery is gradually reduced.
The arteries most commonly affected include the coronary arteries which supply blood to the heart muscle, as well as the carotid arteries supplying the brain, and the arteries of the legs. The consequences depend on where the disease is most advanced: narrowing of the coronary arteries causes angina or, if a plaque ruptures suddenly, a heart attack. The same process in the carotid arteries raises the risk of stroke.
What makes atherosclerosis particularly insidious is its silence. The process begins as early as adolescence in some people, progresses over decades, and typically produces no symptoms at all until the narrowing is severe enough to restrict blood flow, or until a plaque ruptures and an artery becomes suddenly blocked.
How Plaque Forms, The Role of Inflammation
Atherosclerosis is not simply a matter of cholesterol coating the inside of arteries like limescale in a pipe. The process is considerably more complex, and inflammation plays a central role at every stage.
The inner lining of every artery, called the endothelium is a remarkably active layer of cells that regulates blood flow, prevents clotting, and maintains the health of the vessel wall. When the endothelium is damaged or stressed, by high blood pressure, high cholesterol, cigarette smoke, or elevated blood sugar, it becomes inflamed and its protective function is compromised.
In response to this inflammation, LDL cholesterol (commonly referred to as “bad” cholesterol) begins to penetrate the artery wall and accumulate beneath the endothelium. The immune system responds by sending white blood cells, particularly a type called macrophages, to the site. These cells engulf the cholesterol deposits, but in doing so they become engorged and die, forming what are called foam cells. Over time, these foam cells accumulate into fatty streaks within the artery wall, which gradually evolve into more complex and structured plaques containing cholesterol, calcium, inflammatory cells, and fibrous tissue.
The resulting plaque does two harmful things. First, it narrows the artery, reducing blood flow. Second, and more dangerously, it can become unstable. If the fibrous cap covering the plaque ruptures, triggered by inflammation, stress, or other factors, the contents are exposed to the bloodstream. The body responds to this as it would to any injury: by forming a blood clot. In a coronary artery, that clot can block the vessel entirely within minutes, cutting off blood supply to the heart muscle. This is a heart attack.
Atherosclerosis is not just a plumbing problem of narrowing pipes. It is an inflammatory disease of the artery wall, which is why managing inflammation, alongside cholesterol and blood pressure, is central to modern cardiovascular care.
What Drives Atherosclerosis, The Risk Factors
Decades of research have identified a clear set of risk factors that accelerate the development of atherosclerosis. Some of these cannot be changed, age, biological sex, and family history all play a role. But the majority are modifiable, and addressing them meaningfully changes the trajectory of the disease.
| Risk Factor | How It Contributes | Modifiable? |
|---|---|---|
| High LDL cholesterol | Drives plaque formation by penetrating the artery wall and triggering inflammation | Yes, diet, exercise, statins, other medications |
| High blood pressure | Damages the endothelium, making it more susceptible to plaque buildup | Yes, lifestyle changes and medication |
| Smoking | Directly injures the endothelium and promotes inflammation and clot formation | Yes, cessation is one of the most impactful changes possible |
| Diabetes | Elevated blood sugar damages blood vessels and disrupts cholesterol metabolism | Yes, blood sugar control significantly reduces cardiovascular risk |
| Obesity | Promotes inflammation, raises blood pressure and cholesterol, impairs insulin sensitivity | Yes, even modest weight loss improves cardiovascular risk profile |
| Physical inactivity | Contributes to obesity, raises blood pressure, and worsens cholesterol levels | Yes, regular exercise has direct benefits on artery health |
| Family history | Genetic factors influence cholesterol metabolism and inflammatory responses | No, but makes management of other risk factors even more important |
| Age | Plaque accumulates over decades; risk increases with age | No, but earlier intervention has greater impact |
| Lipoprotein(a) | An inherited lipid particle that independently raises cardiovascular risk | Partially, emerging therapies are in development |
Does Atherosclerosis Cause Symptoms?
In its early and intermediate stages, atherosclerosis produces no symptoms at all. This is precisely why it is often described as a silent process, there is no pain, no warning sign, nothing to prompt concern. The artery can lose a significant proportion of its internal diameter before blood flow is meaningfully affected.
When symptoms do appear, they reflect the consequences of reduced blood flow to a particular organ. In the coronary arteries, reduced flow during exertion causes angina the chest tightness or pressure that comes on with physical activity and settles with rest. If the artery becomes suddenly blocked, the result is a heart attack. In the arteries supplying the brain, the equivalent events are a transient ischaemic attack (TIA) a temporary disruption of blood flow, or a full stroke. In the arteries of the legs, reduced flow causes peripheral arterial disease often felt as cramping or aching in the calves during walking.
For many people, the first indication that significant atherosclerosis is present is an investigation finding, an abnormal stress test, a calcium score, or an incidental finding on imaging, rather than a symptom. This is one of the arguments for proactive cardiovascular risk assessment, particularly in people with known risk factors.
How Is It Managed?
There is no single treatment for atherosclerosis, management is about addressing the underlying drivers of the disease, stabilising existing plaques, and reducing the risk of future events. The good news is that the tools available to do this are highly effective.
Lifestyle changes remain the foundation. A diet that is low in saturated fat and rich in vegetables, whole grains, legumes, fish, and unsaturated fats, broadly in keeping with Mediterranean dietary principles, supports artery health and improves the cholesterol profile. Regular physical activity, ideally at least 150 minutes of moderate-intensity exercise per week, reduces blood pressure, improves cholesterol, and has direct anti-inflammatory effects on the vessel wall. Stopping smoking produces rapid and substantial cardiovascular benefits. Achieving and maintaining a healthy weight reduces the metabolic burden on the cardiovascular system across multiple dimensions.
Medications play an important complementary role, particularly for those with established disease or elevated risk. Statins are the most widely prescribed class, they reduce LDL cholesterol and have direct anti-inflammatory effects on plaques, helping to stabilise them and reduce the risk of rupture. Additional cholesterol-lowering agents such as ezetimibe and PCSK9 inhibitors are available for those who require further LDL reduction. Blood pressure medications, antiplatelet agents, and blood sugar management all form part of a comprehensive approach tailored to each individual.
In cases where atherosclerosis has caused a significant narrowing in a major artery, a procedure may be required to restore blood flow. In the coronary arteries, this typically means a coronary angiogram followed by balloon dilatation and stenting a minimally invasive procedure in which a small mesh tube is deployed to keep the artery open. For more complex disease involving multiple vessels, coronary artery bypass grafting (CABG) may be recommended. You can read more about both of these on the Heart Matters CAD resource page and in our dedicated CABG article.
- Know your numbers blood pressure, cholesterol, and blood sugar are the key figures. If you don’t know them, ask your doctor to check them.
- Move regularly even moderate daily activity has meaningful benefits for artery health.
- Eat well a Mediterranean-style diet is the best-evidenced dietary pattern for cardiovascular protection.
- Stop smoking no single change has a greater impact on cardiovascular risk than quitting.
- Take prescribed medications consistently statins and other cardiovascular medications work best when taken as directed. Discuss any concerns about side effects with your doctor rather than stopping them.
- Attend regular reviews atherosclerosis is a long-term condition that benefits from ongoing monitoring and adjustment of treatment as needed.
Free Downloads, Heart Matters
Two free tools to help you understand and track your own cardiovascular risk, developed by our cardiology team, free to download, print, and bring to your next appointment.
- Heart Health Risk Factor Checklist a 12-category self-assessment with a traffic light rating system, covering everything from cholesterol and blood pressure to Lp(a) and sleep apnoea
- Blood Pressure Tracking Chart a clean clinical chart for recording home readings, with target range guidance and space for notes to bring to your appointment
Heart Matters Resource
Coronary Artery Disease, The Full Picture
Atherosclerosis is the process, coronary artery disease is the consequence. Our dedicated CAD page covers the coronary arteries in depth, including symptoms, medications, stents, bypass surgery, and Prof. Barlis’s research into plaque using optical coherence tomography.
Heart Matters Resource
When in Doubt, Get Checked Out
Because atherosclerosis develops silently, symptoms, when they do appear, should never be dismissed. If you experience chest discomfort, unexplained breathlessness, or anything that gives you pause, it is always worth getting checked.
Conclusion
Atherosclerosis is the common thread running through most of the cardiovascular conditions we see and treat, heart attacks, angina, stroke, peripheral arterial disease. Understanding what it is, what drives it, and how it progresses puts you in a much stronger position to make sense of your own risk, your test results, and the treatment recommendations your doctor makes.
The most important thing to understand is that this process is not fixed or inevitable. The arteries respond to how we treat them. Risk factors that are identified and managed early have a real and measurable impact on the trajectory of the disease. And for those who already have established atherosclerosis, modern treatment, a combination of lifestyle, medication, and intervention where needed, offers very effective tools for stabilising the condition and reducing the risk of future events.
Understanding your risk is not cause for alarm. It is cause for action, and action, taken early, makes a genuine difference.