Key Points
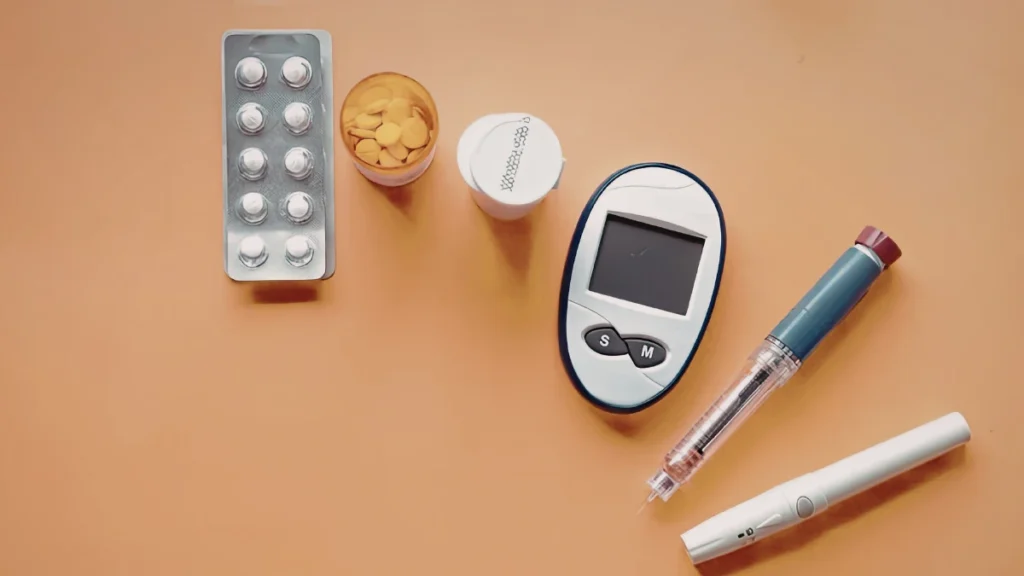
- Oral semaglutide (Rybelsus) is a tablet form of the same active ingredient found in Ozempic, offering patients with type 2 diabetes an injection-free alternative in the GLP-1 receptor agonist class.
- It must be taken on an empty stomach with a small amount of plain water at least 30 minutes before any food, drink, or other medicines. This strict requirement is essential for adequate absorption.
- Oral semaglutide has lower bioavailability than the injectable form, meaning a smaller proportion of the dose reaches the bloodstream. It is effective but somewhat less potent for weight loss than the weekly injection at equivalent doses.
- The SOUL trial demonstrated that oral semaglutide reduces major cardiovascular events by 14% in patients with type 2 diabetes at high cardiovascular risk, confirming meaningful heart protection beyond glucose control.
- Side effects, particularly nausea and gastrointestinal discomfort are common when starting, but generally improve over time with slow dose escalation.
- Like all semaglutide products, this is a medicine for specific patients with defined indications always prescribed and monitored in partnership with a doctor, not a general weight loss solution.
Ozempic has become one of the most discussed medicines of our time, but for many patients, the idea of a weekly injection is a significant barrier. Some have a fear of needles. Others find the logistics of self-injection difficult. For others still, the injectable form simply does not suit their lifestyle or preferences.
This is where oral semaglutide marketed as Rybelsus becomes relevant. It is the same active medicine as Ozempic, delivered in tablet form, and it represents a genuinely meaningful option for patients with type 2 diabetes who might otherwise not access this class of treatment.
This article focuses specifically on the oral version, how it differs from the injection, what the evidence shows, and what patients need to know about taking it correctly.
What Is Oral Semaglutide?
Semaglutide belongs to a class of medicines called GLP-1 receptor agonists. These medicines mimic a natural gut hormone, glucagon-like peptide-1, that is released after eating. GLP-1 stimulates insulin release in response to glucose, suppresses the hormone glucagon that raises blood sugar, slows gastric emptying, and reduces appetite by acting on hunger centres in the brain.
Delivering a peptide medicine as a tablet is technically challenging, peptides are proteins, and the digestive system is designed to break proteins down before they can be absorbed. Oral semaglutide overcomes this through a technology called SNAC (sodium N-[8-(2-hydroxybenzoyl)aminocaprylate]) a compound co-formulated with semaglutide that temporarily raises the local pH in the stomach lining and facilitates absorption directly through the gastric mucosa, bypassing the destructive environment of the small intestine.
It is an elegant solution to a genuinely difficult pharmaceutical problem, and understanding it explains why the taking instructions are so specific.
How to Take It, Why the Rules Matter
This is the most practically important section for patients starting Rybelsus. The absorption mechanism only works under very specific conditions, and not following them correctly significantly reduces the medicine’s effectiveness.
How to Take Oral Semaglutide Correctly
These instructions are not optional, they are essential for the medicine to work properly. Unlike most tablets, oral semaglutide requires a very specific routine.
- Take on a completely empty stomach first thing in the morning, before anything else. No coffee, no juice, no other medicines.
- Use no more than half a glass (approximately 120ml) of plain water not sparkling water, not juice, not tea. Plain water only. A larger volume of liquid dilutes the SNAC mechanism and reduces absorption.
- Wait at least 30 minutes before eating, drinking, or taking other medicines this allows adequate time for the tablet to be absorbed through the stomach lining before food or liquid alters the gastric environment.
- Swallow the tablet whole do not crush, chew, or split it.
- Take at the same time every morning consistency supports stable drug levels and makes the routine easier to maintain.
💡 Many patients find linking this routine to an existing morning habit, waking up, taking the tablet, then showering or getting ready before breakfast, makes the 30-minute wait easy to manage in practice.

Oral vs Injectable, How Do They Compare?
Patients often ask whether the tablet is as good as the injection. The honest answer is: it is effective, but there are meaningful differences worth understanding.
| Oral Semaglutide (Rybelsus) | Injectable Semaglutide (Ozempic) | |
|---|---|---|
| Route | Once daily tablet | Once weekly subcutaneous injection |
| Doses available | 3mg, 7mg, 14mg | 0.25mg, 0.5mg, 1mg, 2mg |
| Bioavailability | ~1%, very low, but sufficient at correct doses | ~89%, much higher |
| Blood glucose lowering | Effective, comparable HbA1c reduction at 14mg | Effective, slightly superior at higher injectable doses |
| Weight loss | Moderate, typically 3–5kg at 14mg | Greater, typically 5–7kg at 1–2mg doses |
| Cardiovascular evidence | Yes, SOUL trial (2025): 14% reduction in major CV events | Yes, SUSTAIN-6 and others: comparable CV protection |
| Convenience | Daily tablet, no needle required, but strict morning routine needed | Weekly injection, more flexibility but requires self-injection |
| Best suited to | Patients who prefer tablets, needle-averse patients, those with lower weight loss goals | Patients who can self-inject, those needing greater glucose or weight reduction |
Neither form is universally superior, the right choice depends on the individual patient’s preferences, clinical goals, and circumstances. For a broader overview of the full semaglutide class including Wegovy and the cardiovascular outcomes evidence in obesity, see our dedicated article: Semaglutide and Cardiovascular Prevention, What the Major Trials Show.
What Does the Evidence Show?
The pivotal cardiovascular trial for oral semaglutide is the SOUL trial published in the New England Journal of Medicine in 2025. This trial enrolled over 9,600 patients with type 2 diabetes and high cardiovascular risk, either established cardiovascular disease or chronic kidney disease, and compared oral semaglutide 14mg daily against placebo over approximately four years.
These results confirm that the cardiovascular protection seen with injectable GLP-1 agonists extends to the oral formulation, an important finding that strengthens the case for offering patients a choice of delivery method based on their preferences rather than effectiveness alone.
For glucose control, head-to-head trials have shown that oral semaglutide 14mg produces HbA1c reductions comparable to the injectable form at lower doses, making it a clinically meaningful option for many patients with type 2 diabetes whose primary goal is glucose management with cardiovascular protection.
Who Is Oral Semaglutide For?
Oral semaglutide is approved for the treatment of type 2 diabetes in adults whose blood sugar is not adequately controlled with other medicines. It is not currently approved as a weight loss medicine, that indication belongs to Wegovy at the higher 2.4mg injectable dose.
Most Likely to Benefit From the Oral Option
- Have type 2 diabetes with inadequate glucose control on existing medicines
- Have established cardiovascular disease or high cardiovascular risk where the SOUL trial evidence directly applies
- Have a preference against injections needle phobia, dexterity issues, or simply a strong preference for tablets
- Have modest weight loss goals the oral form produces meaningful but more moderate weight reduction than higher-dose injectables
- Can reliably maintain the strict morning fasting routine patients whose mornings are very variable may find the once-weekly injectable more practical
- Are being considered for injectable GLP-1 therapy but want to trial the class first oral semaglutide can be a useful introduction
Side Effects
The side effect profile of oral semaglutide is similar to the injectable form, gastrointestinal symptoms are the most common experience, particularly in the early weeks of treatment.
Common Side Effects
- Nausea the most frequently reported side effect, typically most pronounced in the first 4–8 weeks and after dose increases. Eating smaller, lower-fat meals helps. Starting at the lowest dose (3mg) and escalating slowly is essential.
- Diarrhoea or constipation both can occur as the gut adjusts to slowed gastric emptying. Usually settles within a few weeks.
- Vomiting less common than nausea but can occur. If persistent and significant, contact your doctor.
- Reduced appetite a therapeutic effect, but ensuring adequate nutrition and protein intake during treatment is important.
- Fatigue commonly reported in early weeks, usually transient.
- Hypoglycaemia oral semaglutide alone does not typically cause low blood sugar, but if combined with insulin or sulphonylureas, hypoglycaemia risk increases and dose adjustments of the other medicines may be needed.
A Word on Cost and Access
Cost is a real and legitimate part of this conversation. Oral semaglutide is an expensive medicine, without subsidy, the annual cost is significant and out of reach for many patients. Subsidised access varies by country and indication.
In Australia, Rybelsus is PBS-listed for type 2 diabetes in patients who meet specific eligibility criteria, making it accessible at the standard prescription co-payment for qualifying patients. If you are unsure whether you qualify for subsidised access, your GP or endocrinologist can advise. Eligibility criteria do evolve as new evidence is incorporated into guidelines, so it is worth revisiting even if you were told previously that you did not qualify.
It is also worth noting that SGLT2 inhibitors another class of medicines with powerful cardiovascular and kidney benefits, are often used alongside or as an alternative to GLP-1 agonists in patients with type 2 diabetes and heart disease. For more on this complementary class, see our article on SGLT2 inhibitors and heart protection.
Conclusion
Oral semaglutide is a genuine and meaningful addition to the management of type 2 diabetes, particularly for patients who have strong reasons to avoid injections. The cardiovascular evidence from the SOUL trial is reassuring and places it firmly alongside injectable GLP-1 agonists as a cardioprotective option in high-risk patients with diabetes.
It requires more discipline in administration than a standard tablet, the empty stomach rule, the plain water, the 30-minute wait, but for patients who can build this into their morning routine reliably, it is highly manageable and highly effective.
As with all medicines in this class, it is not appropriate for everyone, and the decision to start should be made carefully with your doctor, taking into account your full clinical picture, other medicines, and individual goals. Used in the right patient, with the right expectations and the right support, it is a valuable and evidence-based option for improving both metabolic and cardiovascular health.