Key points
- The number of bypasses — single, double, triple, quadruple — describes how many coronary arteries were rerouted, not how serious or dangerous the operation is.
- A triple bypass on a fit, healthy patient is often a more straightforward operation than a single bypass on someone with poor heart function or multiple other medical conditions.
- The goal of bypass surgery is to restore blood flow to every area of the heart that needs it. More bypasses often reflects a more thorough job, not a worse one.
- The choice of vessel used for the bypass matters enormously for how long it lasts. The internal mammary artery is the gold standard — more than 9 out of 10 are still working well after 10 years. The radial artery comes a close second.
- Recovery depends far more on your age, fitness, and heart function than on the number of bypasses performed. Modern recovery practices help patients get home and back to normal life faster.
In more than three decades as a cardiac surgeon, there is one moment in the pre-operative consultation that I have come to recognise instantly. I tell a patient they need a triple bypass, and I watch the calculation begin behind their eyes.
Triple must mean three times worse than single. It must mean three separate problems, three separate operations, or simply that their heart disease is three times as serious as it might have been. It must mean a longer recovery, a bigger risk, a harder road.
Patients also often ask where the “veins” are taken from, presuming that veins are the material mostly used to bypass blocked coronary arteries. Two other common questions are “are you cracking open my chest?” and “it must be very painful”.
None of these assumptions are correct. Clearing them up — calmly, carefully, and completely — is one of the most important conversations I have with patients before we go to theatre.
Your coronary arteries — a brief map
To understand what the number of bypasses means, you first need a basic picture of the arteries we are talking about.
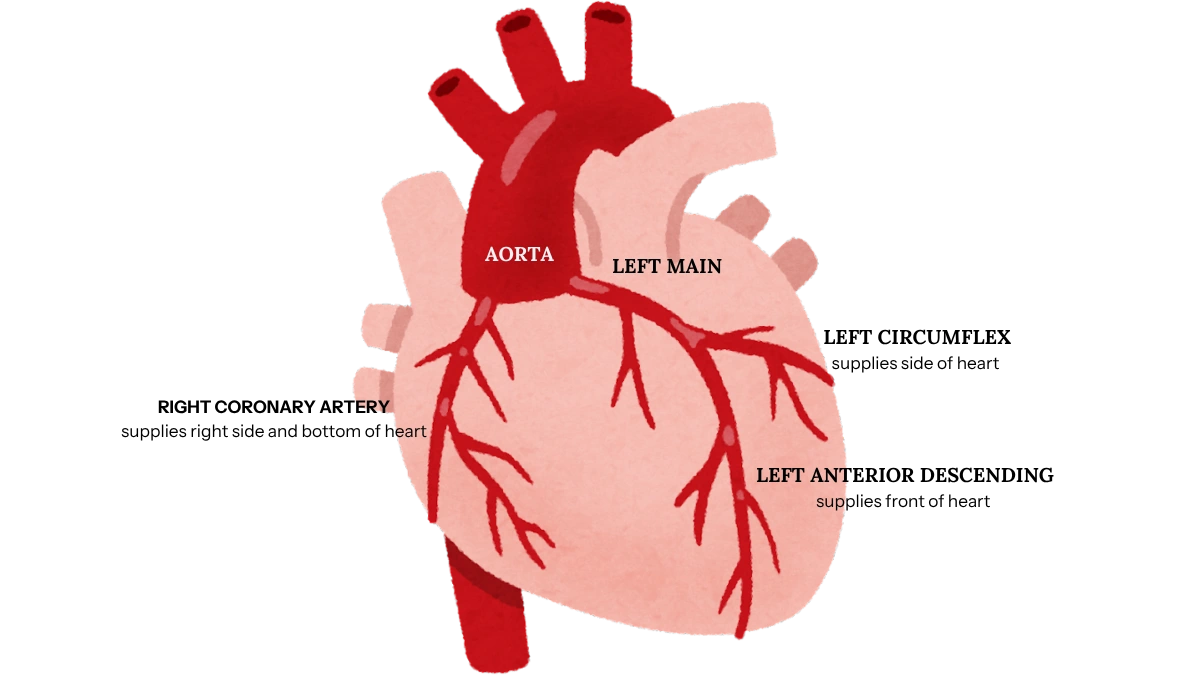
The heart has three main coronary arteries — the blood vessels that wrap around its surface and supply the heart muscle with the oxygen and nutrients it needs to keep beating. When one or more of these arteries becomes significantly narrowed or blocked, the heart muscle downstream is deprived of blood flow. That is coronary artery disease, and bypass surgery is one of the ways we restore that flow.
The three arteries are the left anterior descending artery, known as the LAD, which runs down the front of the heart and supplies a large portion of the left ventricle (the heart’s main pumping chamber). The left circumflex artery, or LCx, which curves around the left side of the heart, supplying the back and left side of the left ventricle. And the right coronary artery, or RCA, which supplies the right side of the heart and, in most people, the bottom wall of the left ventricle.
The LAD is the most important of the three. Because it supplies such a large portion of the left ventricle, significant blockages here demand prompt attention, and it is almost always the most important artery that we bypass.
Each of these three main arteries also has significant branches that supply their own territories of heart muscle. The diagonal branches come off the LAD and supply the front and side wall of the left ventricle. The marginal branches come off the LCx and supply the side wall. When one of these branches is large and significantly diseased, it can benefit from its own bypass — and this is often where a fourth graft comes from.
What the number actually means
A single bypass means one artery has been bypassed. A double bypass means two. A triple bypass — the most common type — means three arteries have been bypassed, typically the three main coronary arteries. A quadruple bypass means four grafts have been placed, usually because one of the main arteries also has a large branch that is diseased and needs its own bypass.
That is it. The number describes how many new routes we created around blocked segments — nothing more, nothing less.
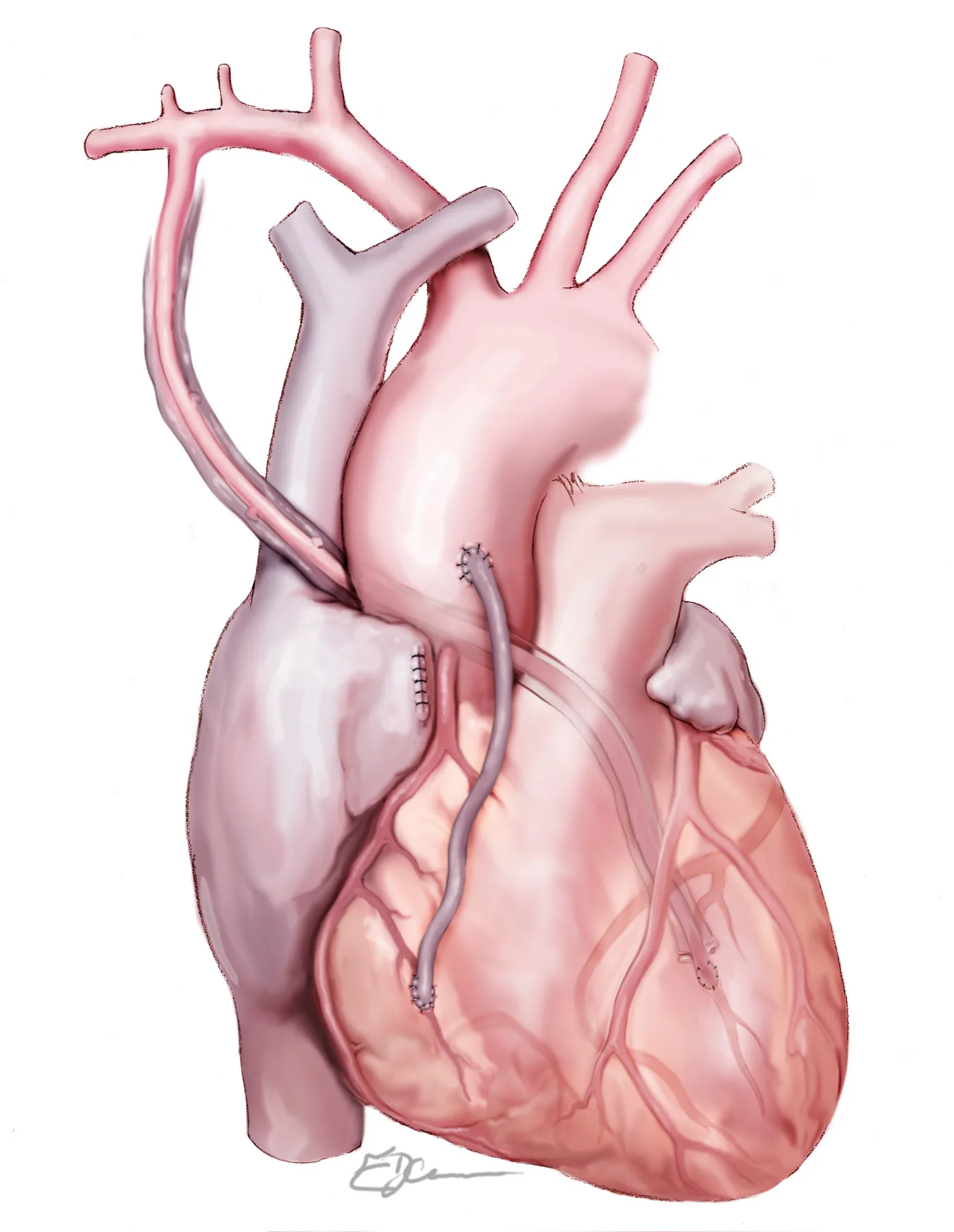
A traditional bypass arrangement
A bypass arrangement using the right internal mammary artery (RIMA), taken from inside the chest wall and crossed over to reach a coronary artery on the front of the heart, together with a saphenous vein graft from the leg.
Illustration: E. JeannesThe number does not tell you how blocked the arteries were. It does not tell you how long the operation took. It does not tell you how serious your heart disease is compared to someone with a different number. And it certainly does not predict your recovery in any simple way.
The number of bypasses is best understood as a description of thoroughness. A surgeon who performs three bypasses on a patient with disease in all three main arteries has done a complete job. A surgeon who performs only one bypass on the same patient has left significant disease untreated — and that carries its own consequences.
The most common scenario
Triple bypass surgery is the most frequently performed type, because most patients who reach the point of needing surgery have significant disease in more than one artery. By the time coronary artery disease is severe enough to warrant surgery rather than stenting, it has often progressed throughout the coronary tree, affecting multiple vessels rather than a single isolated blockage.
This is not bad news. It is simply the nature of the disease, and it is exactly the scenario bypass surgery was designed to address.
Does more bypasses mean a more serious operation?
This is the question I am asked most often, and the honest answer is: not in the way most patients assume.
The duration and complexity of bypass surgery depends far more on the patient’s overall condition than on the number of grafts being placed. A triple bypass on a fit 58-year-old with good heart function, no diabetes, good lung function, and no prior cardiac surgery is a very different operation from a single bypass on a frail 75-year-old with a significantly weakened heart, impaired kidneys, and poor lung reserve. The first patient may be in theatre for three to four hours and home within five days. The second may face a considerably more complex course regardless of how many vessels were grafted.
What the surgical team is assessing before your operation is not primarily the number of bypasses required, it is you. Your age, your fitness, your heart muscle function, your other medical conditions, and whether you have had heart surgery before. These are the variables that shape the surgical risk, not the number written on the consent form.
The grafts — what we use and why
Bypass surgery works by using a healthy blood vessel from elsewhere in the body to create a new route around the blocked section of a coronary artery. The vessel we choose — the graft — matters enormously for how long the bypass lasts.
The internal mammary artery — the gold standard
The left internal mammary artery (also called the left internal thoracic artery, or LIMA) runs along the inside of the chest wall and is the graft of choice for bypassing the LAD. The evidence for its longevity is extraordinary: more than 9 out of 10 of these grafts are still working well after 10 years, and many remain open at 20 years and beyond.
The reason is biological. The mammary artery is a living conduit. It adapts to its new role, responds to the demands of the coronary circulation, and resists the process of re-narrowing that affects vein grafts over time. When we place a LIMA-to-LAD graft, we are not simply creating a bypass — we are creating a durable, long-term solution for the most important artery in the heart.
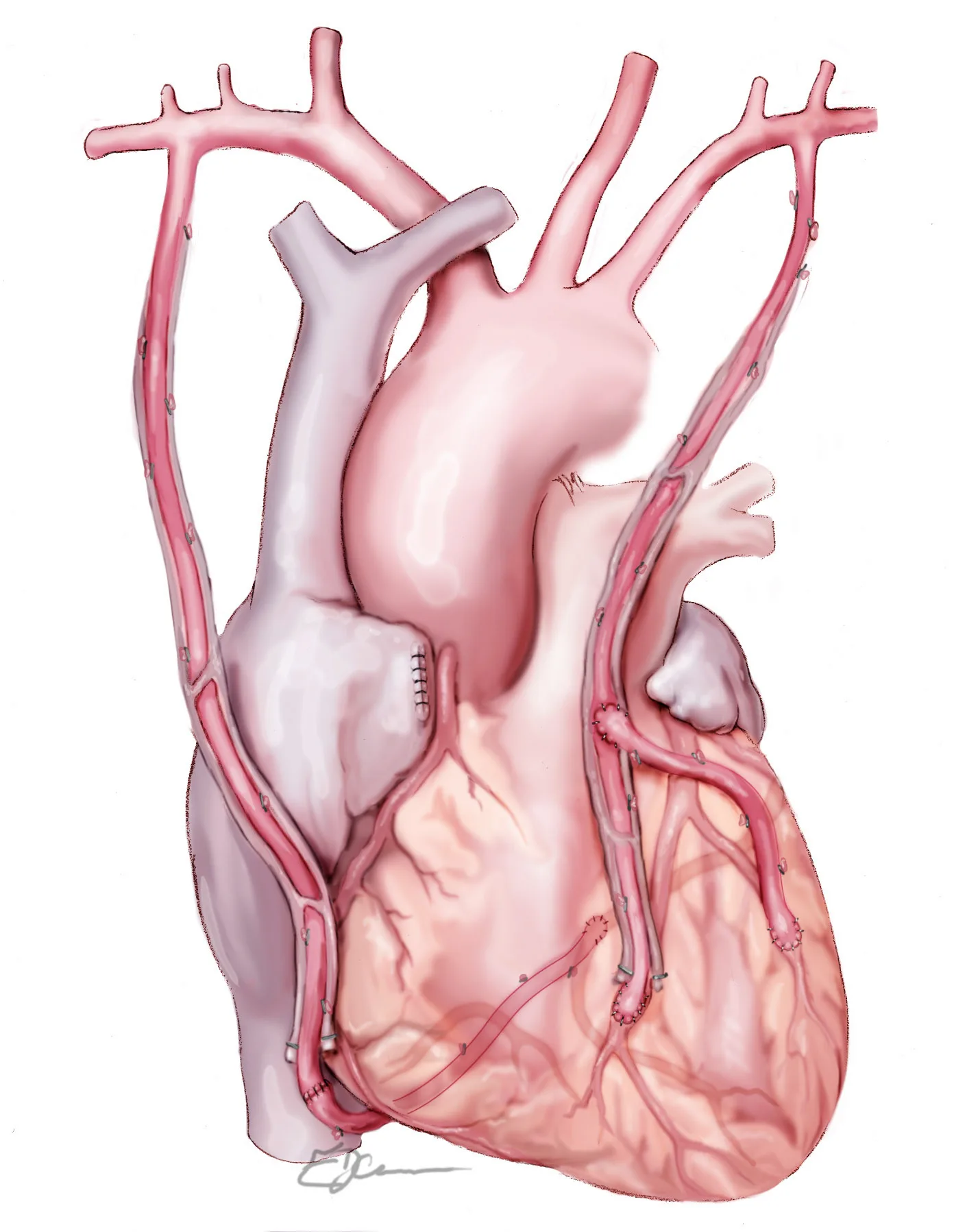
All arterial grafts
Both mammary arteries combined with a radial artery graft from the forearm. All three coronary territories bypassed using arterial grafts, offering the most durable long-term result in younger patients.
Illustration: E. JeannesWhere two mammary arteries are used — a technique known as bilateral internal mammary artery grafting — the evidence suggests even better long-term outcomes, particularly in younger patients. This is a more demanding approach and is not suitable for everyone, but in the right patient it represents the highest standard of surgical revascularisation.
The radial artery
The radial artery — the artery at the wrist used to take your pulse — can also be harvested and used as a graft in selected patients. Its long-term success rates fall between the mammary artery and the saphenous vein, and it is particularly useful in younger patients where durability is the priority.
The use of this artery was pioneered here in Melbourne by my mentor, Prof Buxton, in the late 1990s. Harvested from the forearm, it allows for a quick recovery and good outcomes. This graft has now been shown to have very good early and long-term results, staying open for over 15 years.
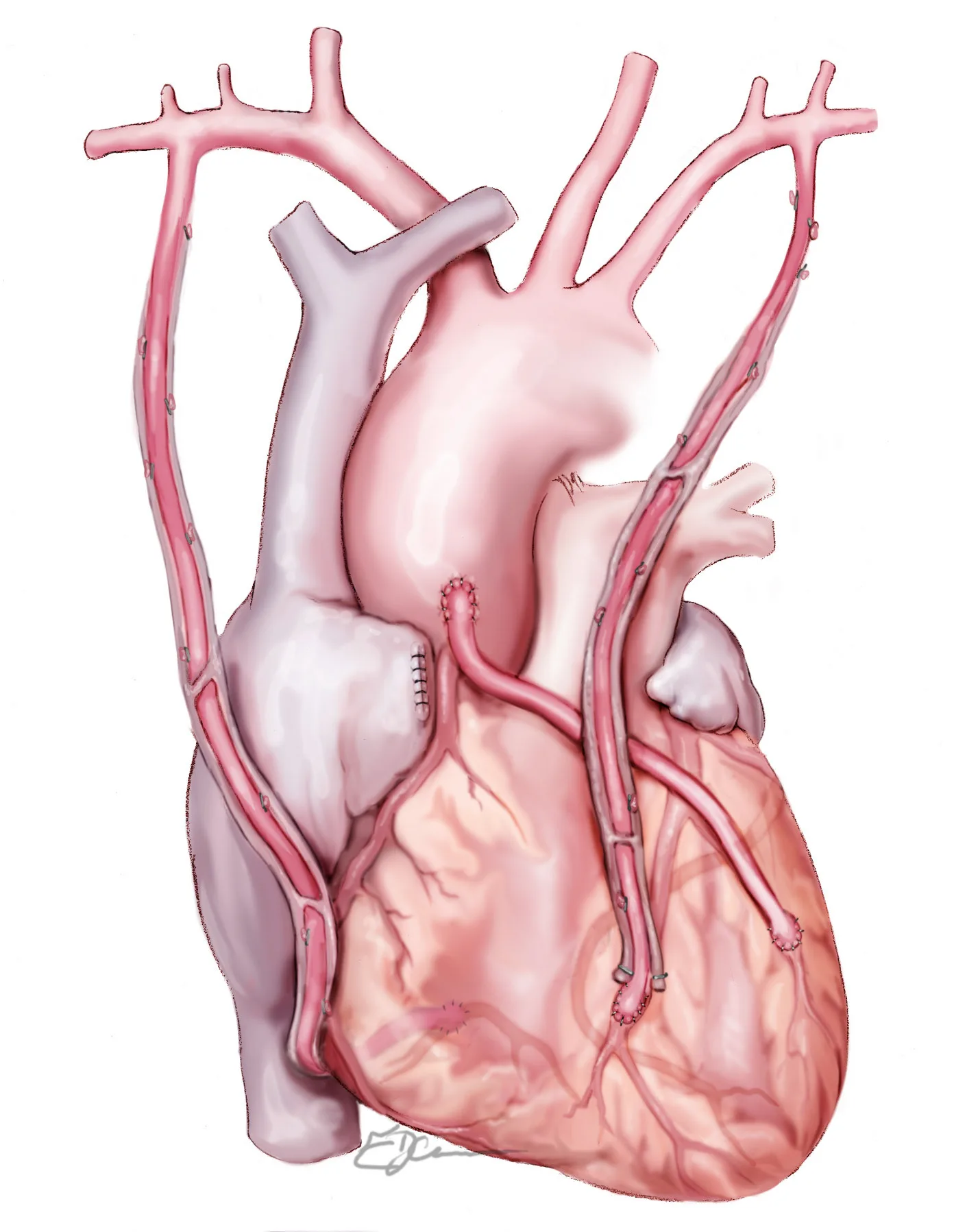
Using both mammary arteries
Both the left and right internal mammary arteries used as arterial grafts. Evidence suggests even better long-term outcomes in suitable patients, particularly younger ones. This approach is technically demanding and is not suitable for everyone.
Illustration: E. JeannesIt is worth remembering that arterial grafts are much better than the alternative — saphenous vein grafts, which start to block off at around five years.
Saphenous vein grafts
The saphenous vein — the long vein running along the inside of the leg — is the most commonly used graft after the mammary artery. It is harvested through a small incision or, increasingly, through minimally invasive techniques, and used to bypass the remaining vessels.
Vein grafts are reliable and effective, but they do not last as long as arterial grafts. About half of saphenous vein grafts are still fully open after 10 years, compared to more than 9 out of 10 for the LIMA. This is not a failure of the surgery; it is simply the biology of vein grafts placed into the high-pressure arterial circulation. It means that for younger patients, or those with a long life expectancy, using as many arterial grafts as possible is an important part of surgical planning.
| Graft | Source | Still open at 10 years | Best used for |
|---|---|---|---|
| Left internal mammary artery (LIMA) | Inside chest wall | More than 9 in 10 | LAD bypass — gold standard in almost all patients |
| Right internal mammary artery (RIMA) | Inside chest wall | More than 8 in 10 | Second arterial graft — particularly in younger patients |
| Radial artery | Forearm | About 8 in 10 | Additional arterial graft in suitable patients |
| Saphenous vein | Leg | About 5 in 10 | Additional vessels — reliable and widely used |
Quadruple bypass — and beyond
A quadruple bypass is less common than a triple, but far from rare. The fourth bypass almost always goes to one of the important branches of the three main arteries — most often a large diagonal branch off the LAD, or a significant marginal branch off the LCx — when that branch is diseased enough to be affecting heart muscle on its own.
So when your surgical team recommends a quadruple bypass, it does not usually mean you have a fourth main coronary artery that most people do not have. It means that one of the branches coming off your main arteries is large and important enough to warrant its own graft alongside the three main ones.
Quintuple bypass — five grafts — does occur, though it is uncommon. It typically involves the three main arteries plus two of their most significant branches, and is generally reserved for patients with very extensive coronary disease who are good surgical candidates.
I want to be clear about something important: the fact that a patient needs four grafts rather than three does not mean their operation is dramatically more dangerous or their recovery dramatically longer. It means their coronary disease was extensive enough to require four new routes, and that their surgical team was thorough enough to provide them.
Why a thorough job matters
One of the principles that guides every bypass operation I perform is the goal of restoring blood flow to every area of the heart that is at risk from significant disease. Surgeons call this complete revascularisation. In plain terms, it means leaving no important blockage behind.
The evidence is clear that leaving significant coronary disease untreated — because it is technically difficult or adds time to the operation — is associated with worse long-term outcomes. Patients whose disease is fully treated have lower rates of later heart attack, lower rates of repeat procedures, and better survival at five and ten years.
This is why the number of bypasses is, in some respects, a reflection of the surgeon’s commitment to doing the job properly. A patient who needs three vessels bypassed and receives three grafts has had their disease fully treated. A patient who receives only two grafts because the third vessel was technically challenging has been left with residual disease, and the consequences of that decision may not become apparent for years.
How we access the heart — and close it again
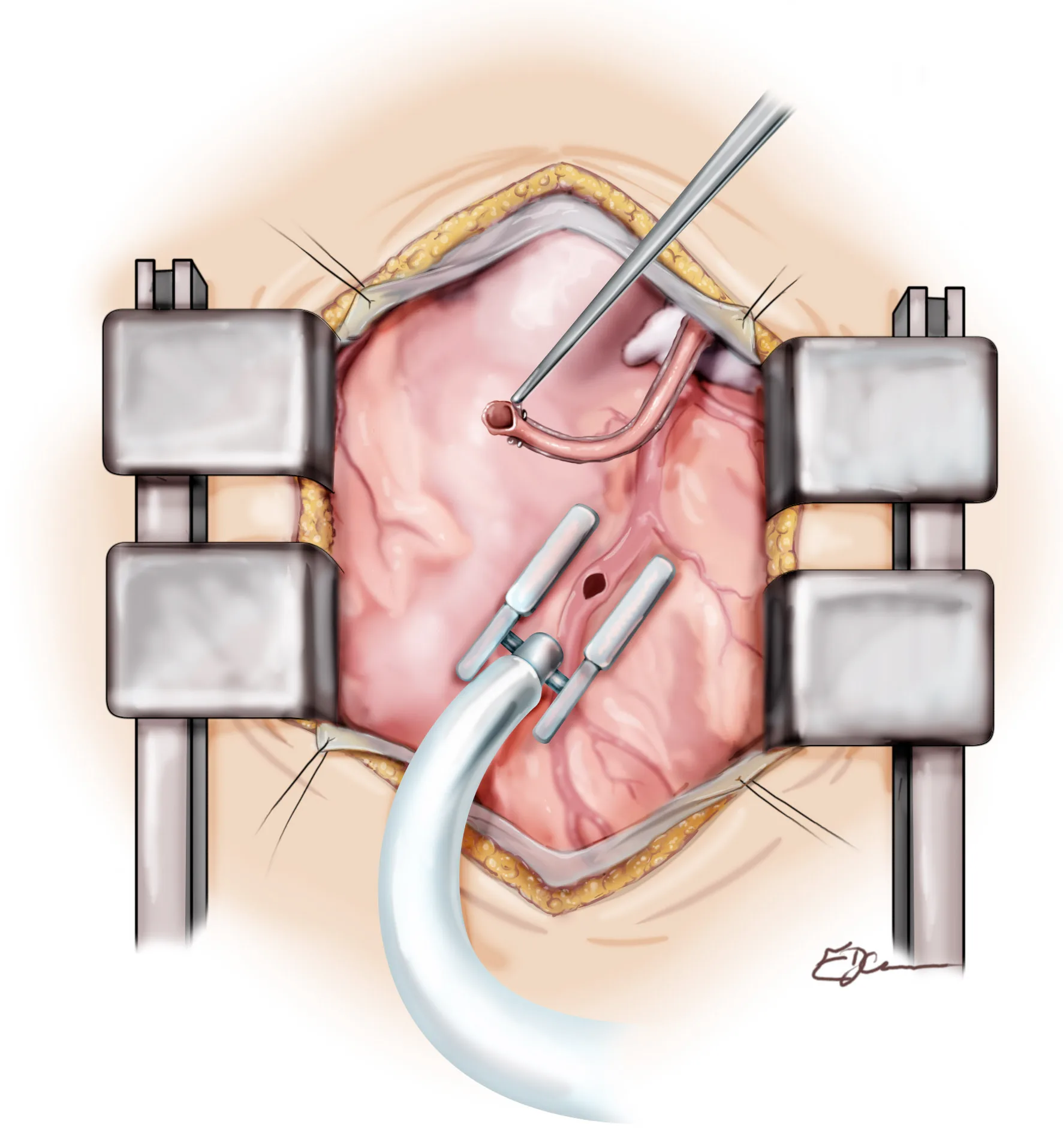
Inside the operative field
A view of the heart during bypass surgery, through the opening in the chest. The retractors on each side hold the chest open. The silver device in the middle gently holds a small area of the beating heart still while the graft is sewn on.
Illustration: E. JeannesFor a typical triple bypass, the chest is opened through a midline incision called a median sternotomy (a controlled split of the breast bone). This gives the surgical team full access to all parts of the heart and allows us to harvest the internal mammary artery or arteries as grafts.
Traditionally, the split breast bone is brought back together at the end of the operation and held with stainless steel wires. One of the important improvements in recent years has been the use of titanium plates and screws to close the chest — a technique I have helped to develop. It is now recommended as part of modern Enhanced Recovery After Surgery (ERAS) guidelines, which are a set of practices designed to get patients home and back to normal life faster. With plate closure, patients need less pain relief, opioid use can often be avoided entirely, and the breast bone heals more securely.
When you meet your cardiac surgeon before your operation, it is entirely reasonable to ask: will all my blocked arteries be bypassed? What vessels are being grafted, and why? Are there any vessels that cannot be bypassed, and what does that mean for my outcome? And how will you close my chest — will you use plates and screws to help the breast bone heal?
Recovery — what the number means for you
The most important thing I can tell you about recovery from bypass surgery is this: the number of bypasses is one of the least important variables in how you will recover.
What matters far more is your age and baseline fitness, your heart muscle function going into the operation, whether you have diabetes, kidney disease, or lung disease, and whether this is your first heart surgery or a second operation after a previous one. A fit, active 60-year-old recovering from a triple bypass will almost always have a smoother and faster recovery than a sedentary 72-year-old recovering from a single bypass.
| Recovery milestone | Typical timeframe |
|---|---|
| Breathing tube removed | Within hours of surgery in most patients |
| Out of intensive care | 24–48 hours |
| Home from hospital | 5–7 days in uncomplicated cases |
| Driving again | 4–6 weeks — check with your surgeon (as little as 2 weeks if the sternum is closed with plates) |
| Return to light activity | 4–6 weeks |
| Full recovery | 6–12 weeks for most patients |
| Cardiac rehabilitation | Begins 4–6 weeks after surgery — strongly recommended |
Cardiac rehabilitation — a structured program of supervised exercise, education, and psychological support — is one of the most important things you can do after bypass surgery, regardless of how many vessels were grafted. The evidence for its benefit in reducing repeat events, improving exercise capacity, and supporting return to a full life is overwhelming. I encourage every patient I operate on to attend.
A final word
Bypass surgery — whether single, double, triple, or quadruple — is one of the most studied and most successful operations in the history of medicine. More than a million procedures are performed worldwide each year, and the outcomes, for appropriately selected patients, are excellent.
The number of bypasses you need is determined by your anatomy — by the extent and location of your coronary disease, and by the surgical team’s commitment to treating it thoroughly. It is not a measure of how ill you are, how dangerous your operation will be, or how difficult your recovery will be. It is a description of thoroughness.
If you are facing bypass surgery, I hope this article has answered some of the questions that were forming in your mind when you first heard the number. The best thing you can do now is ask your cardiac surgeon to walk you through exactly what is planned — which vessels are being bypassed, what grafts will be used, and what treating all your disease thoroughly will mean for your long-term outlook. These are questions every cardiac surgeon expects to be asked, and they deserve a clear and complete answer.
Questions to ask your cardiac surgeon before bypass surgery
- How many bypasses are planned, and which arteries are being grafted?
- What grafts will be used — mammary artery, radial artery, or saphenous vein?
- Will all my blocked arteries be bypassed — are there any vessels that cannot be treated?
- What is my surgical risk based on my specific profile?
- Will you close my chest with plates and screws?
- What does recovery look like for someone with my age and health?
- When can I start cardiac rehabilitation, and where should I go?
- What medications will I need after surgery, and for how long?