- Blood clots are a normal and essential part of the body’s healing response. The problem arises when they form in the wrong place, at the wrong time, or grow too large.
- The two main types are venous clots, forming in veins, most commonly as DVT in the legs or pulmonary embolism in the lungs, and arterial clots, which cause heart attacks and strokes.
- DVT and pulmonary embolism together are called venous thromboembolism (VTE), common, treatable, and with excellent outcomes when identified promptly.
- Modern anticoagulant medications, particularly Direct Oral Anticoagulants (DOACs), are highly effective and have transformed how VTE is treated over the past decade.
- Knowing the symptoms of DVT and PE, and acting on them quickly, makes a significant difference to outcomes.
If you have just been told you have a blood clot, or you’re trying to understand what happened to someone you love, the word itself can feel alarming. “Clot” sounds sinister. It sounds like something has gone badly wrong.
The reassuring context is that clotting is something your body does deliberately, continuously, and correctly thousands of times throughout your life. It is the mechanism that stops a cut from becoming a catastrophe. The problem arises only when that mechanism fires in the wrong place, at the wrong time, or on a scale that obstructs rather than protects.
This article, written with A/Prof. Ali Bazargan, Haematology Consultant at St Vincent’s Hospital Melbourne, explains what blood clots are, why they form, what the symptoms are, and what treatment looks like today.
How Blood Clots Form
The normal process
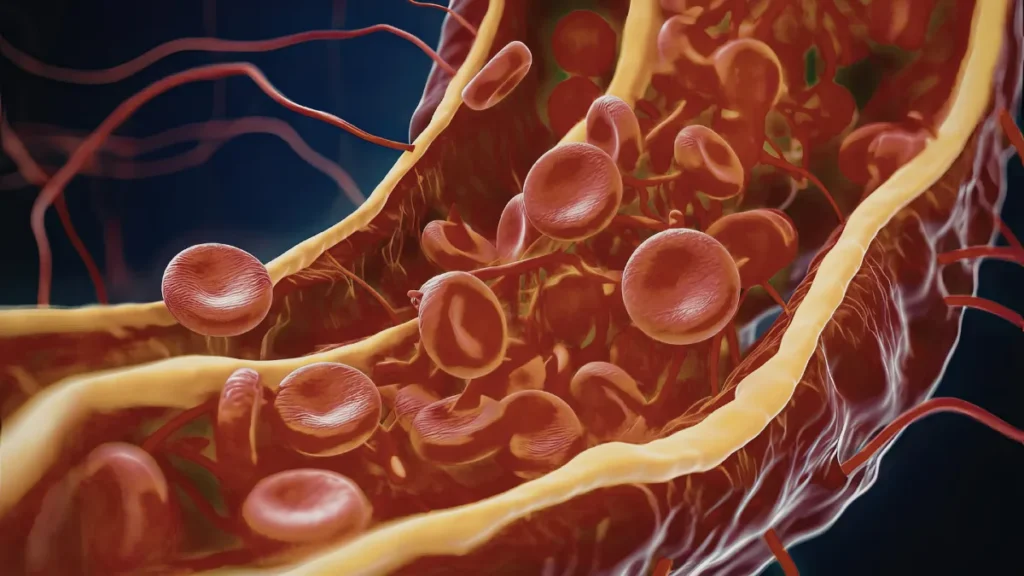
When a blood vessel is injured, the body responds immediately. Platelets, small cell fragments circulating in the bloodstream, rush to the injury site and clump together to form an initial seal. This triggers a cascade of chemical reactions involving proteins called clotting factors, culminating in the production of fibrin, a thread-like protein that weaves through the platelet plug and reinforces it into a stable, solid clot.
Once the vessel has healed, the body’s own clot-dissolving system gradually breaks the clot down. The whole process is a finely tuned balance, and it works remarkably well most of the time.
When it goes wrong
Problems arise when that balance tips. In the context of cardiovascular medicine, the concern is clots forming inside intact or diseased blood vessels, obstructing circulation, or breaking off and travelling to other sites in the body.
The Two Main Types
Blood clots divide into two fundamentally different categories, and the distinction matters because the causes, symptoms, and treatments differ considerably.
| Feature | Venous clot (VTE) | Arterial clot |
|---|---|---|
| Where it forms | Veins, legs, pelvis, lungs | Arteries, coronary, carotid, peripheral |
| Main cause | Slow blood flow, immobility, clotting disorders | Atherosclerotic plaque rupture |
| Key consequences | DVT, pulmonary embolism | Heart attack, stroke, limb ischaemia |
| Primary treatment | Anticoagulants, DOACs or warfarin | Antiplatelet agents, thrombolytics, intervention |
| Prevention focus | Mobility, hydration, anticoagulation in high-risk situations | Risk factor management, antiplatelet therapy, statins |
DVT, What It Feels Like
Recognising the symptoms
Deep vein thrombosis most commonly develops in the deep veins of the calf or thigh. The symptoms reflect the clot obstructing blood flow back toward the heart.
The affected leg may become swollen, sometimes dramatically so, painful or tender along the course of the vein, warm to the touch, and red or discoloured over the skin. Not all DVTs produce all of these features. Some, particularly smaller calf clots, produce almost no symptoms at all.
When it travels to the lungs
Part of a DVT can break free, called an embolus, and travel through the circulation to the lungs, producing a pulmonary embolism. When this happens, the symptoms shift to the chest.
Sudden breathlessness, chest pain that worsens when breathing in, a dry cough, palpitations, and dizziness or lightheadedness are all warning signs. A large PE can cause sudden collapse and, if untreated, can be life-threatening.
Who Is at Higher Risk?
VTE risk comes from the interplay of personal factors and situational triggers. Several of the most important are worth knowing about.
Immobility
Long-haul travel, hospitalisation, post-operative recovery, blood pools in the leg veins and clot risk rises.
Major surgery
Hip and knee replacements carry high VTE risk, prophylactic anticoagulation is now routine after these procedures.
Active cancer
One of the strongest VTE risk factors, malignancy alters the clotting system, and treatments add further risk.
Inherited thrombophilia
Genetic variations such as Factor V Leiden amplify clot risk, particularly when combined with other triggers.
Pregnancy
VTE risk rises substantially in the third trimester and postpartum period, one of the most important risk windows.
Oestrogen medications
The combined pill and some forms of HRT raise VTE risk, particularly in combination with other risk factors.
Treatment, What Happens Next
Anticoagulation, the cornerstone of treatment
For most people with confirmed DVT or PE, anticoagulation is the primary treatment. An important point to understand: anticoagulants don’t dissolve the existing clot, the body’s own system does that over time. What they do is stop the clot from growing and prevent further clots from forming while healing occurs.
Direct Oral Anticoagulants, DOACs, including rivaroxaban, apixaban, and dabigatran, are now the preferred treatment for most patients with VTE. They are taken orally, require no routine blood test monitoring, and have been shown in large clinical trials to be at least as effective as warfarin with a better safety profile.
Warfarin, still the right choice for some
Warfarin remains appropriate for patients with certain conditions, antiphospholipid syndrome, some mechanical heart valves, or severe kidney impairment where DOACs aren’t suitable. It requires regular INR blood test monitoring and is more affected by diet and other medications, but for the right patients it remains highly effective.
How long do you take it?
Duration depends on whether the clot had a clear cause, such as surgery or immobility, or occurred without an obvious trigger. A provoked clot is typically treated for three to six months. An unprovoked or recurrent clot may require extended or indefinite anticoagulation, a decision made individually with your treating team based on your personal risk of recurrence and bleeding.
When more aggressive treatment is needed
A small proportion of patients with a massive pulmonary embolism causing haemodynamic collapse require more urgent intervention, clot-dissolving medications (thrombolytics) delivered intravenously, catheter-directed treatment directly into the clot, or in rare cases surgical removal. These carry higher bleeding risk and are reserved for situations where the PE is immediately life-threatening.
One of the most important things I tell patients starting anticoagulation is: don’t stop it without speaking to your doctor first, even if you feel completely well. The medication is doing its job precisely because you feel well. Stopping early significantly increases the risk of the clot extending or a new one forming.
- Was my clot provoked or unprovoked, and does that change how long I need anticoagulation?
- Which anticoagulant am I on, and are there any foods, medications or activities I need to be aware of?
- Should I be tested for an underlying clotting disorder?
- What symptoms should prompt me to seek urgent attention while on treatment?
- When will we review whether to continue or stop anticoagulation?
Heart Matters Resource
When in Doubt, Get Checked Out
A swollen, painful leg after a long journey or period of immobility, or unexplained breathlessness, should always be assessed promptly. DVT and PE need to be ruled out. Getting checked is always the right call.
Conclusion
Blood clots sound alarming, but the vast majority of people diagnosed with DVT or PE, treated promptly with modern anticoagulation, make a full recovery. The treatments available today are safer, simpler, and more effective than they were even a decade ago.
The most important things are recognising the symptoms early, getting assessed without delay, and understanding your treatment, why you are taking it, for how long, and what to watch for. That knowledge puts you in control of your recovery.
If you have questions about your specific situation, the type of clot, the duration of treatment, or whether you need testing for an underlying clotting disorder, the questions box above is a good starting point for your next conversation with your doctor or haematologist.