Key Points
- Statins are among the most prescribed medications in the world, and among the most stopped without anyone being told.
- Most of what circulates online about statins is negative. The clinical evidence tells a more balanced story.
- Statins do more than lower cholesterol, in people at genuine cardiac risk, research shows they stabilise vulnerable plaques and reduce the inflammatory process that triggers heart attacks.
- Side effects are real and should never be dismissed. Muscle aches, fatigue, and memory concerns deserve a proper conversation with your doctor, and there are options.
- Not everyone needs a statin. For those prescribed one after a cardiac event or because of genuinely high risk, the evidence for staying on it is strong.
I hear some version of this almost every week in clinic. A patient sits down, and somewhere in the conversation they mention, sometimes apologetically, that they have stopped their statin. Or they are thinking about stopping it. Or they started it and felt different, and nobody ever explained why they were on it in the first place.
I understand this completely. The conversation around statins in the lay media and on social media is overwhelmingly negative. Muscle pain, memory loss, fatigue, “I haven’t felt like myself since I started.” These are real experiences, and they deserve to be taken seriously, not brushed aside with a blanket reassurance that statins are safe.
What I want to do here is share the conversation I try to have in clinic: honest, balanced, and grounded in what the evidence actually shows.
What a Statin Actually Does
Most patients are told their statin lowers cholesterol. That is true, but it is a bit like saying a seatbelt stops you moving forward. Technically accurate, but it misses what matters.
The more important action of a statin, particularly for someone who has already had a heart attack or has significant coronary artery disease, is what it does to the plaques inside the artery wall.
Let me explain what I mean by that.
The Plaque Story, What Is Actually Happening Inside
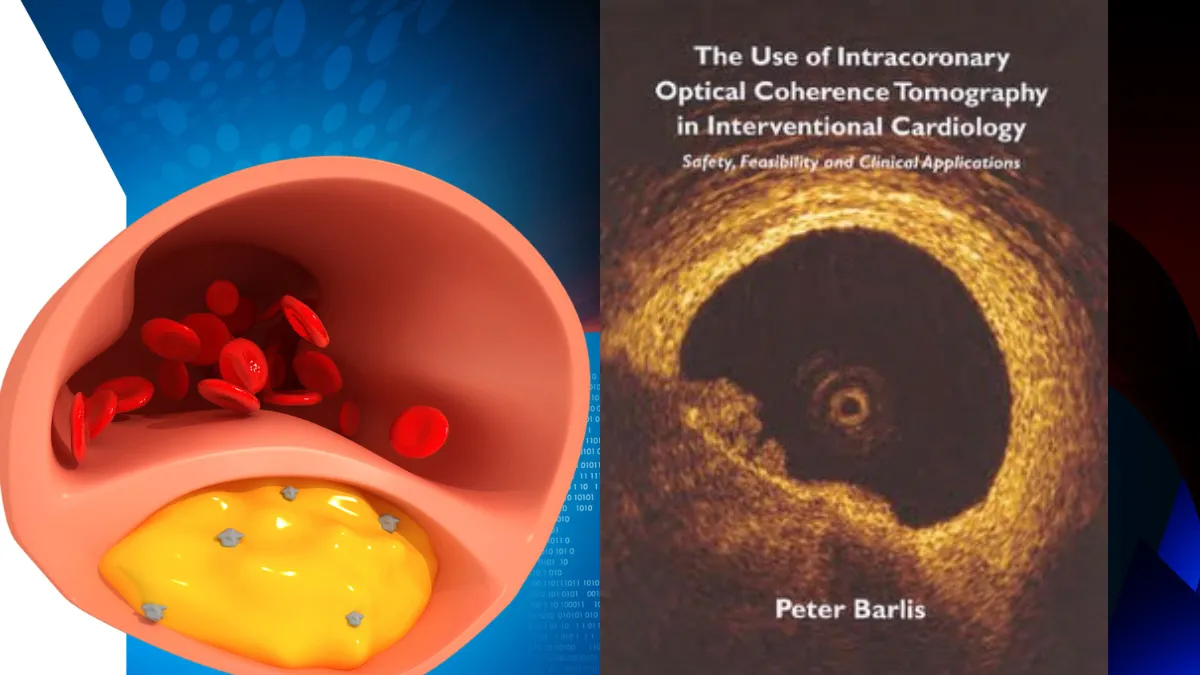
Left: an illustration of a coronary artery cross-section showing a lipid-rich plaque with inflammatory cells at the fibrous cap. Right: an actual OCT image from my PhD thesis, the view from inside a coronary artery, with the dark region indicating a lipid pool beneath the vessel wall.
I often show patients this image in clinic. On the left is an illustration of what a vulnerable plaque looks like in cross-section, the open vessel with blood flowing through it, and beneath the surface, a pool of soft, lipid-rich material. You can see the grey star-shaped cells sitting right at the boundary between the plaque and the vessel lining. Those are macrophages, inflammatory cells that have migrated into the plaque and are, in a sense, destabilising it from within.
On the right is a real image, from my own PhD research using a technology called optical coherence tomography, or OCT, which involves threading a tiny light-based probe inside a living coronary artery. The bright golden ring is the artery wall. The dark shadow at the bottom is exactly what it looks like on the illustration: a lipid pool sitting just beneath the surface, visible in extraordinary detail from inside the vessel itself.
The thin layer of tissue covering that lipid pool is called the fibrous cap. In a vulnerable plaque, this cap is thin and fragile, and those inflammatory cells are actively weakening it further. When the cap ruptures, the lipid-rich contents spill into the bloodstream. A clot forms almost instantly. Depending on how large that clot is, and which artery is involved, the result is either a smaller heart attack, what we call an NSTEMI, or a complete blockage and a larger event, an STEMI.
This is what most heart attacks actually are. Not a gradual narrowing that finally closes off. A rupture. A sudden event triggered by a plaque that may not have been causing any symptoms at all.
Where Statins Come In
Here is what changes the conversation for me, and what I explain to every patient who asks why they need to stay on their statin.
Statins stabilise vulnerable plaques. They reduce the inflammatory cells infiltrating the cap, those macrophages that are weakening it from within. Over time, research shows they can thicken the fibrous cap itself, making it more resistant to rupture. They change the biology of the plaque, not just the number on a blood test.
This is why, in patients who have already had a heart attack or who have established coronary disease, the evidence for statins is so compelling. It is not primarily about the LDL number. It is about reducing the likelihood that a vulnerable plaque will rupture and cause another event. This is also the reason the relationship between statins and your calcium score is more nuanced than it first appears.
Reduction in major cardiovascular events with high-intensity statin therapy in high-risk patients, regardless of starting cholesterol level
Cholesterol Treatment Trialists’ (CTT) Collaboration meta-analyses
Who Actually Needs a Statin?
This is where I want to be direct: not everyone does.
There is a legitimate conversation to be had about patients who have been started on a statin primarily because a cholesterol number crossed a threshold, without a proper discussion of their individual cardiovascular risk, their age, their other risk factors, and what the medication is actually expected to achieve for them personally.
If you were prescribed a statin and never had a proper conversation about why, that is worth revisiting with your GP or cardiologist. Cardiovascular risk calculators, used by doctors worldwide, look at the full picture: age, blood pressure, smoking status, family history, and cholesterol together. The number on its own tells only part of the story. Emerging tools like the hs-CRP test and imaging such as the coronary calcium score can add further context in the right patient.
Where the evidence is clearest and most compelling is in people who have already had a cardiac event, those with established coronary artery disease, and those at genuinely high cardiovascular risk. For these patients, the benefit of staying on a statin is well established and significant.
Questions Patients Ask Me Most
These are the questions I hear most often in clinic, answered as honestly as I can. As always, these are for general information, and any decision about your own medication should be made in conversation with your doctor.
Will statins damage my muscles?
Muscle discomfort affects around 5–10% of people on statins. Serious muscle damage is genuinely rare. Significant pain, weakness, or dark urine should prompt a call to your doctor, but general aching is often manageable with a dose change or switch to a different statin, which your doctor can discuss with you.
Can statins affect my memory?
The overall evidence does not support a link between statins and dementia or significant cognitive decline. Some people notice a change in mental clarity, an experience that deserves investigation, not dismissal. This is worth raising with your doctor rather than simply stopping the medication.
Do I really need one if I feel fine?
Not everyone does. If a statin was started purely because a number crossed a threshold, with no discussion of individual risk, that conversation is worth revisiting with your GP. For people who have had a cardiac event or have established coronary disease, the evidence is strong regardless of how they feel.
Can I take a break from my statin?
This is a conversation to have with your doctor before making any change. Many people quietly stop and never mention it, but in those with coronary artery disease or a prior heart attack, statins are doing something important beyond lowering a number. There are almost always options if the current medication is not suiting you.
Are there alternatives if I can’t tolerate statins?
Every-other-day dosing works well for many people who experience daily side effects. Switching to a different statin often resolves muscle symptoms. Ezetimibe is a well-tolerated tablet that lowers cholesterol through a different mechanism and is often used alongside or instead of a statin. For high-risk patients who cannot tolerate statins at all, PCSK9 inhibitors are a highly effective option. All of these alternatives are best discussed with your doctor before making any changes.
Does it matter which statin I’m on?
Statins vary in potency and side effect profile. Rosuvastatin (Crestor) and atorvastatin (Lipitor) are the most potent. Some people tolerate one significantly better than another. If side effects are an issue, the answer is often a switch or dose adjustment, a discussion worth having with your doctor before considering stopping altogether.
Should I take my statin in the morning or at night?
There are some differences between statins, and timing can play a small role, but the most important factor is consistency. Taking it at the same time each day matters more than which hour is chosen. For a fuller explanation of the pharmacology behind this, see our article on the timing of cholesterol-lowering medications. Your doctor is best placed to advise on what suits your particular medication and routine.
Can I lower my cholesterol naturally?
Many products claim to lower cholesterol naturally, most have not been tested in proper clinical trials, and caution is warranted. Two approaches with reasonable evidence behind them are plant sterols and a generous fibre intake. A Mediterranean-style diet remains the most well-studied dietary pattern for cardiovascular risk. None of these replace a statin when one is clinically indicated, but they can be meaningful complements. Any supplement addition is worth discussing with your doctor first.
The Side Effects, Taking Them Seriously
Muscle aches and pains are the most commonly reported side effect, and they are real. Roughly 5–10% of people on statins experience some degree of muscle discomfort, though true muscle damage (myopathy) is considerably rarer.
What is also real is the nocebo effect, the phenomenon where knowing a medication might cause symptoms makes those symptoms more likely to be noticed and attributed to it. Large blinded trials have shown that many people who report muscle symptoms on statins experience the same symptoms on placebo. That does not mean the symptoms are not real, it means the relationship between statins and those symptoms is more complex than it first appears.
Memory and cognitive concerns are raised frequently, and understandably, given how much has been written about them. The overall evidence does not support a causal link between statins and dementia or significant cognitive decline. Some people do notice a change in mental clarity when starting a statin, and this deserves investigation rather than dismissal.
My strong view is this: side effects should never simply be accepted. There are several different statins, they vary in their potency and their side effect profiles, and some people tolerate one far better than another. Dose adjustments matter. Every-other-day dosing works well for some patients. And if a statin genuinely cannot be tolerated, there are alternative lipid-lowering options, including ezetimibe and PCSK9 inhibitors, that achieve excellent results. All of this is a conversation to have with your doctor.
If you are experiencing side effects on your statin, the conversation with your doctor is always worth having before stopping. There is almost always something that can be tried.
What I Tell My Patients
When a patient comes to me having stopped their statin because of something they read online, I don’t argue with them. I show them the image above, the plaque, the cap, the inflammatory cells, and I explain what the evidence shows about what these medications actually do inside the artery wall. Most of the time, that conversation changes things.
Conclusion
Statins are not perfect medications, and the decision to take one, or stay on one, deserves a proper, individual conversation. Not every person with a mildly elevated cholesterol needs a statin, and side effects should never be dismissed or simply tolerated.
But for those with established heart disease or genuinely high risk, the evidence is clear: statins do something that no other medication currently does as well. They get inside the artery wall and stabilise the plaques that cause heart attacks. That is worth understanding, and worth a conversation before making a decision either way.
If you have questions about your statin, or you have stopped taking it and haven’t told your doctor, please bring it up at your next appointment. There are options, and the conversation is always worth having.
This article provides general information only and is not medical advice. Any decisions about your medications should be made in conversation with your cardiologist, GP, or pharmacist.