Key points
- The choice between stents and bypass surgery depends on the complexity of your coronary disease, not just how blocked your arteries are
- The SYNTAX trial, a landmark collaboration between cardiologists and cardiac surgeons, created the evidence base that guides this decision today
- Your heart team uses several scoring tools to personalise the recommendation for you
- In most cases there is time. This decision is made carefully, with your full understanding and agreement
- No calculator replaces the Heart Team conversation. You are at the centre of this decision
I have spent more than fifty years in interventional cardiology. When I began my career, a blocked coronary artery was a life-altering diagnosis. The options were limited, the procedures crude by today’s standards, and the anxiety felt by patients and their families was, I suspect, not so different from what many of you reading this are feeling right now.
The field has changed beyond recognition. The early promise of pharmacotherapy: medications to slow the disease, relieve symptoms, reduce risk. The arrival of balloon angioplasty in the late 1970s, which felt revolutionary at the time: the idea that you could open a blocked artery from the inside, through a catheter no wider than a drinking straw, without a single incision on the chest. Then came the bare metal stent, a small metal scaffold that held the artery open after the balloon was deflated, which solved one problem and introduced another. Then drug-eluting stents, coated with medication to prevent the artery from narrowing again, and which changed everything.
Each of these advances was built on evidence: on clinical trials, on thousands of patients who gave their time, trusted their doctors, and allowed themselves to be part of something larger than their own treatment. If you have ever participated in a clinical trial, the advances that benefit cardiac patients today exist in part because of you. That debt is rarely acknowledged as clearly as it should be.
If you have just been told you need stents or bypass surgery
If you are reading this, you may have recently been told that you have significant coronary artery disease. Perhaps your angiogram has shown blockages in one or more of the arteries that supply blood to your heart. Perhaps your cardiologist has mentioned the words stents or bypass surgery, and perhaps, in that moment, the room felt a little smaller.
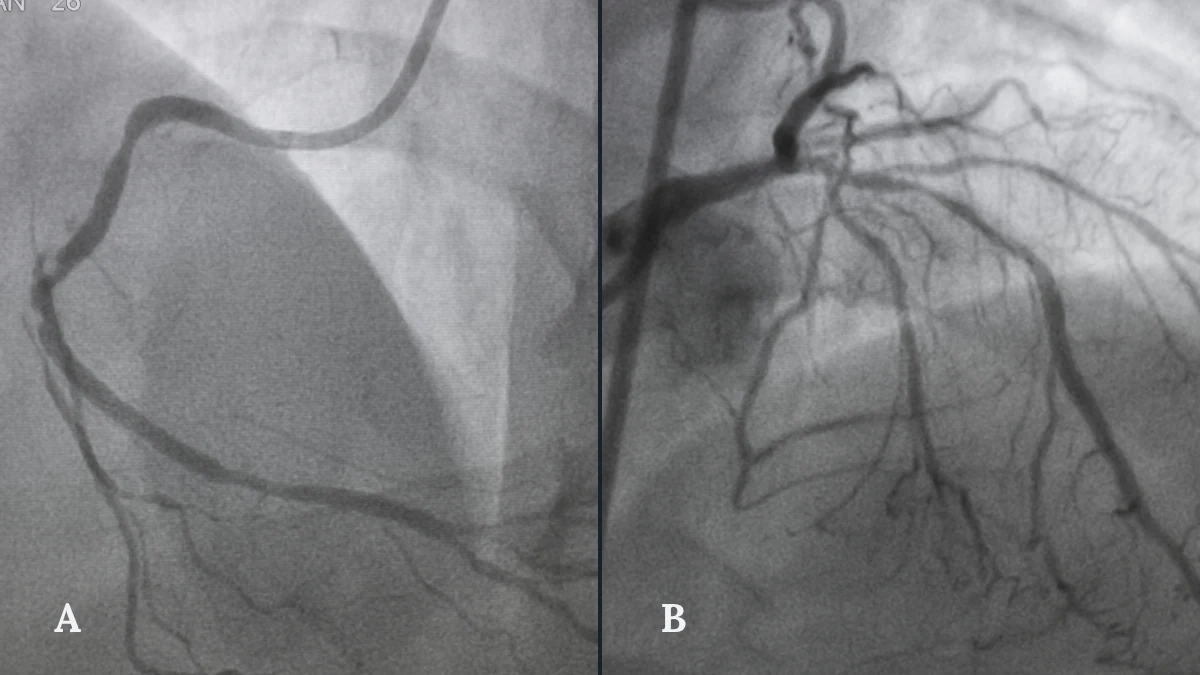
A coronary angiogram
During an angiogram, a thin flexible catheter is passed into the coronary arteries and a small amount of contrast dye is injected. The dye makes the arteries visible under X-ray, allowing your cardiologist to see exactly where plaque has built up and where blood flow is restricted. This is the investigation that forms the foundation of your Heart Team’s decision.
That feeling is entirely understandable. It is one of the more confronting conversations medicine asks patients to have. But I want to offer you something before we go any further: reassurance.
The decision about how best to treat your coronary disease is not arbitrary. It is not a coin toss. It is the product of decades of rigorous clinical research, including a landmark trial that I had the privilege of leading, and it is made by a team of specialists whose entire professional lives have been devoted to getting this decision right for patients exactly like you.
What follows is an attempt to explain how that decision is made, what your heart team is weighing up, and what you deserve to understand about your own care.
The question that needed an answer
By the early 2000s, interventional cardiology was at a crossroads.
Drug-eluting stents had arrived and the results were remarkable. For the first time, we could place a stent in a blocked coronary artery and dramatically reduce the chance of it narrowing again, the problem called restenosis that had plagued balloon angioplasty and bare metal stents for two decades. Cardiologists were understandably excited. The technology was advancing rapidly, and we were beginning to treat increasingly complex disease, multiple blocked arteries, blockages in critical locations, patterns of disease that had previously belonged almost exclusively to the cardiac surgeons.
But excitement is not evidence.
The honest truth was that we were pushing into territory where the data had not yet followed. Bypass surgery had decades of long-term outcome data behind it. It was proven, reproducible, and for patients with complex multivessel coronary disease, it had saved an enormous number of lives. The question that cardiologists and cardiac surgeons both knew needed answering was whether stents could match those outcomes in the most complex cases, or whether surgery remained the stronger choice.
What made this moment unusual in medicine was what happened next. Rather than cardiologists and surgeons arguing their respective corners, the two disciplines sat down together and agreed to find out.
A collaboration built on honest questions
The SYNTAX trial was conceived as a genuine partnership. On the cardiology side, I led the study design and execution. On the surgical side, Professor Friedrich Mohr of Leipzig brought the same rigour and the same commitment to finding the right answer, regardless of what that answer turned out to be.
We recruited 85 centres across Europe and the United States and enrolled 1,800 patients with either three-vessel coronary disease, significant blockages in all three of the main arteries supplying the heart, or left main disease, where the blockage sits at the origin of the coronary tree and carries particular weight in terms of risk. Every patient was assessed by both a cardiologist and a cardiac surgeon before randomisation. The Heart Team concept, the idea that complex coronary disease should never be decided by one specialty alone, was not an afterthought. It was built into the trial’s DNA from the very first protocol meeting.
Patients were randomised to receive either percutaneous coronary intervention with drug-eluting stents, the technical term for catheter-based stenting procedures, commonly abbreviated to PCI, or coronary artery bypass grafting, the surgical procedure commonly known as bypass surgery or CABG. We followed them for one year initially, then five years, then ten.
What the trial found, and why it mattered
The results, when they came, were nuanced in the way that the best science always is. They did not declare a single winner. They did something more valuable: they identified who benefited most from each approach.
Patients with less complex coronary disease did equally well with stents as with surgery at five and ten years. But patients with more complex disease, multiple blockages, difficult anatomy, involvement of critical vessel segments, did better with bypass surgery at five and ten years. The difference was meaningful, and it was consistent across multiple analyses.
The critical insight was this: it was not simply a question of stents versus surgery. It was a question of which patient, with which anatomy, benefits most from which treatment. And to answer that question properly, we needed a way to measure coronary complexity objectively. That tool became the SYNTAX score.
Research Spotlight
10 Years of SYNTAX: What a Decade of Research Taught Us About Your Heart
Most medical studies follow patients for a year or two. The SYNTAX trial followed 1,800 patients for a full decade, one of the longest and most detailed studies ever conducted in heart disease treatment.
What did ten years of follow-up reveal? That the decision between stents and bypass surgery is not just about your arteries, it is about you as a whole person. Factors including whether you have diabetes, how well your heart pumps, your kidney function, your body weight, and even your mental health before the procedure were all found to influence long-term outcomes. Patients who were on good medical therapy, cholesterol medication, blood pressure treatment, consistently did better regardless of which procedure they had.
The ten-year data also confirmed that for patients with blockages in all three main heart arteries, bypass surgery provided a meaningful survival advantage over stenting. For patients with disease at the critical left main junction, outcomes were more comparable, and the decision depends heavily on the individual.
Serruys PW et al. 10 Years of SYNTAX: Closing an Era of Clinical Research After Identifying New Outcome Determinants. JACC: Asia, 2023.
The SYNTAX score: measuring the complexity of your coronary disease
Not all coronary disease is equal. A single, straightforward blockage in one artery is a fundamentally different clinical problem from three heavily calcified blockages across multiple vessels, one of which sits at a critical branching point where two arteries divide. The SYNTAX score gave the field a standardised, reproducible way to measure coronary complexity from the angiogram, the X-ray map of your coronary arteries, and express it as a single number.
Each significant blockage is assessed for its location, severity, length, and features that make it more or less technically challenging to treat. The individual scores are added together to produce a total SYNTAX score. The higher the number, the more complex the coronary anatomy.
| Score band | What it means | General direction |
|---|---|---|
| Low, 22 or below | Fewer blockages, simpler anatomy | Stenting outcomes comparable to bypass surgery |
| Intermediate, 23 to 32 | Moderate complexity, careful assessment needed | Heart Team decision: both options weighed carefully |
| High, 33 or above | Multiple blockages, complex anatomy | Bypass surgery generally favoured for long-term outcomes |
Beyond the anatomy: the SYNTAX Score II
The SYNTAX Score II adds eight clinical variables, including age, kidney function, diabetes status, and lung function, to the anatomical score, producing two side-by-side estimates: predicted four-year mortality with PCI, and with CABG. It is a considerably more personalised tool, and increasingly the one your team will use when the decision is genuinely difficult. More recently it was updated using ten years of follow-up data from the full SYNTAX programme, producing more accurate long-term predictions.
What your heart team is actually looking at
The SYNTAX score captures the complexity of your coronary anatomy, but it is only one part of the picture. Before your heart team makes a recommendation, they are weighing up two distinct sets of information: what your arteries look like, and what you are like as a patient. Both matter enormously.
The patient
Age and frailty
Bypass surgery is a major operation. Frailty and other conditions influence whether its benefits outweigh its risks for you specifically.
Diabetes
Strong evidence favours bypass in diabetic patients with multivessel disease. The FREEDOM trial established this clearly.
Heart muscle function
The ejection fraction, how well your heart pumps, affects both the risk and likely benefit of each treatment option.
Kidney function
Kidney health is an important input into surgical risk scores and affects contrast dye management during procedures.
Prior heart surgery
A second operation on the chest carries significantly higher risk. Previous bypass often shifts the balance toward stenting.
Your preferences
Recovery time, lifestyle, and personal values matter. Where evidence supports either option, your informed preference shapes the decision.
Age and overall health. A fit 55-year-old and a frail 78-year-old with the same coronary anatomy may receive very different recommendations, and rightly so. For a patient with significant frailty, poor lung function, or multiple other medical conditions, the risks of surgery itself may outweigh its benefits, even when the anatomy would otherwise favour it.
Diabetes. Diabetes deserves special mention because the evidence here is particularly strong. The FREEDOM trial, a landmark study examining diabetic patients with multivessel coronary disease, found that bypass surgery produced meaningfully better long-term outcomes than stenting in this group. Diabetes accelerates disease progression throughout the coronary tree, and bypass surgery offers a degree of future-proofing that stents in individual lesions cannot replicate.
relative reduction in major cardiovascular events with bypass surgery vs stenting at 5 years, in diabetic patients with multivessel coronary disease
Source: FREEDOM Trial, Farkouh ME et al, New England Journal of Medicine, 2012
Heart muscle function. How well your heart is pumping, measured as the ejection fraction, influences both the risk of any procedure and the likely benefit. The ten-year SYNTAX data showed that patients with reduced heart pumping function had significantly higher rates of adverse outcomes regardless of treatment, underlining the importance of protecting heart function from the outset.
Kidney function. Contrast dye used during angiography and stenting can stress the kidneys, and kidney function is an important input into surgical risk scores.
Previous heart surgery. A second operation on the chest carries significantly higher technical risk. In this situation, stenting, even for complex disease, may be the preferred option.
What you want. A patient who understands their options and has strong preferences about recovery time, lifestyle, or risk tolerance deserves to have those preferences heard and incorporated into the decision. This is not a minor consideration.
The lesions: your blockages
Number of vessels involved. Single-vessel disease is almost always treated with stenting when intervention is needed. Three-vessel disease is where the stents-versus-bypass discussion most often begins.
The left main coronary artery. This short but critical vessel supplies the majority of the heart muscle in most people. A significant blockage here carries particular weight and is always discussed by the full Heart Team.
Bifurcation lesions. Blockages at branching points are technically demanding to treat with stents and carry additional weight in the SYNTAX score.
Chronic total occlusions. An artery completely blocked for three months or more. CTOs can be opened with specialised stenting techniques by experienced operators, but they represent some of the most technically demanding work in interventional cardiology.
Calcification. Heavily calcified arteries resist the expansion needed to deploy a stent optimally. Specialised techniques, including rotational atherectomy, which uses a tiny high-speed burr to modify the calcium before stenting, have improved outcomes considerably.
Diffuse versus focal disease. Long segments of disease spread throughout a vessel are harder to treat completely with stents, and incomplete treatment is associated with worse outcomes than complete revascularisation.
What might push your team towards one option or the other
Your heart team will use scoring tools and imaging to guide their recommendation, but what most patients really want to know is: given my situation, which way does this tend to go? The table below sets out the circumstances that most commonly influence that decision, in plain terms. No single factor is decisive on its own; your team is weighing all of them together.
Multiple blocked arteries with complex disease
Blockages in all three main coronary arteries, particularly with diffuse or complicated anatomy, can often be addressed more completely in a single bypass operation than through multiple stenting procedures.
Simpler or single-vessel disease
Where blockages are limited to one or two vessels, or the anatomy is straightforward, stenting achieves equivalent outcomes with far less recovery time. Surgery adds risk without adding benefit.
Diabetes
Diabetes tends to cause disease that is more widespread and progresses faster. Bypass surgery has shown consistently better long-term outcomes in this group, partly because it protects against future disease in vessels that appear normal today.
Chronic kidney disease
Significant kidney impairment increases the risk of complications from major surgery and general anaesthesia. When kidney disease is advanced, your team may judge that the risks of bypass outweigh its benefits, and stenting becomes the safer path.
Bleeding risk or inability to take blood thinners
Stenting requires two blood-thinning medications taken together for a period afterwards. If you have a significant bleeding history, need another operation soon, or cannot safely take these medicines, bypass surgery avoids this requirement entirely.
Significant lung disease or anaesthetic risk
Bypass requires a general anaesthetic and open-chest surgery. For patients with significant COPD, severe asthma, or other conditions affecting lung function, the anaesthetic risk alone may make bypass unsuitable. Stenting is performed under local anaesthetic and light sedation.
Good overall health and fitness for surgery
For a fit patient with complex multivessel disease, good heart and lung function, and no prior chest surgery, bypass offers highly durable revascularisation. The internal mammary artery graft has a patency rate exceeding 90% at ten years.
Advanced age or frailty
For older or frailer patients, the six to twelve week recovery from bypass, and the risks of major surgery, may outweigh the long-term advantage. A shorter procedure with a faster return to normal life is often the more appropriate choice.
Vessels suitable for graft attachment
Bypass works by attaching a graft vessel beyond the blockage. Where the artery beyond the blockage is of good calibre and accessible, grafts can be placed reliably and durably.
Disease in distal segments unsuitable for grafting
When disease affects the very end portions of coronary vessels, there may be no suitable landing point for a bypass graft. In this situation, stenting of accessible segments may be the only viable interventional option, even when the overall disease is complex.
Valve surgery also needed
If you need both coronary revascularisation and valve repair or replacement, bypass surgery and valve surgery can be performed together in a single operation. This avoids two separate procedures and is generally preferred when the surgical risk is acceptable. Your cardiac surgeon and cardiologist will weigh this carefully together.
High surgical risk with valve disease
Where surgery is considered too high risk, percutaneous options may be considered for both the coronary disease and the valve problem. For example, a patient with significant aortic valve disease and coronary artery disease who cannot safely undergo open-heart surgery may be considered for TAVI (transcatheter aortic valve implantation) alongside PCI. These decisions require particularly careful Heart Team discussion.
Good overall health and fitness for surgery
For a fit patient with complex multivessel disease, good heart and lung function, and no prior chest surgery, bypass offers highly durable revascularisation. The internal mammary artery graft has a patency rate exceeding 90% at ten years.
Previous open-heart surgery
A second operation on the chest carries significantly higher risk than a first. If you have had bypass surgery before, your team will almost always favour stenting for any subsequent coronary intervention, regardless of anatomy.
Remember
None of these factors is decisive on its own. Your heart team is weighing all of them together, alongside the precise detail of your coronary anatomy, to arrive at the recommendation that is right for you. If you are unsure why a particular approach has been recommended, ask. Understanding the reasoning will help you feel confident in the decision.
The scoring tools your heart team uses
No single score makes the decision. Together, the tools below help your team answer two distinct questions: how complex is this coronary disease to treat, and how much risk does this particular patient carry?
| Tool | What it measures | Used by | Output |
|---|---|---|---|
| SYNTAX score | Coronary anatomy complexity: blockage location, severity, and technical difficulty | Cardiologist and surgeon together | Number: low, intermediate, or high complexity |
| SYNTAX Score II 2020 | Anatomy plus clinical profile: age, kidney function, diabetes, lung disease, and more. Updated using 10-year follow-up data. | Heart Team for complex cases | Predicted outcomes with PCI vs CABG, side by side |
| EuroSCORE II | Surgical risk: patient factors influencing the risk of the operation itself | Cardiac surgeon | Estimated % risk of adverse outcomes from the surgical procedure |
| STS score | Surgical risk, complications, and likely hospital stay | Cardiac surgeon | Risk estimates for major complications and prolonged stay |
A word of caution, and of reassurance
If you have been reading this section and finding yourself reaching for a calculator, I understand the impulse. Some of these scoring tools are accessible online, and I have no doubt that some of you will find them. My advice, as someone who spent decades helping to build these tools, is this: please use them as a conversation starter with your cardiologist, not as a verdict.
A SYNTAX score is calculated from a detailed analysis of your coronary angiogram by a trained clinician. The inputs are precise, technical, and require direct interpretation of imaging that takes years of experience to read accurately. More importantly, the score is only ever one input into a much larger conversation.
“No calculator has ever treated a patient. The decision about your coronary disease belongs to you and your team, together.”
Prof. Patrick W. Serruys
There is time
One of the things I most want patients to understand is that in the vast majority of cases, there is time. A patient with a heart attack in progress may require immediate intervention, but most patients facing the stents-versus-bypass conversation are not in that situation. They have had their angiogram. Their disease has been documented. They are stable.
Your case will typically be discussed at a formal Heart Team meeting, a structured review where your cardiologist and cardiac surgeon examine your imaging and scoring together and reach a consensus recommendation. You will then meet with each of them in turn. That process unfolds over days, sometimes a couple of weeks. It is not rushed.
The Heart Team model was built into the SYNTAX trial protocol from the very first meeting. It has since become a cornerstone of international cardiology guidelines. It exists for you.
When bypass surgery is the stronger choice
Bypass surgery, formally known as coronary artery bypass grafting (CABG), involves a cardiac surgeon creating new routes for blood to flow around blocked sections of your coronary arteries, using blood vessels harvested from elsewhere in your body, most often the internal mammary artery from inside your chest wall or the saphenous vein from your leg. It is open-heart surgery, requiring a general anaesthetic and a period on a cardiopulmonary bypass machine. Recovery takes weeks, not days. For the right patient, with the right anatomy, it remains one of the most effective and durable interventions in all of medicine.
Three-vessel disease with high SYNTAX score. The SYNTAX trial’s most consistent finding, confirmed at ten years of follow-up, was that patients with three-vessel disease and a high SYNTAX score had meaningfully better outcomes with bypass surgery, driven primarily by lower rates of repeat procedures and heart attack.
Diabetes with multivessel disease. The FREEDOM trial established clearly that diabetic patients with multivessel coronary disease do better with bypass surgery than stenting over the long term. The mechanism relates to the biology of diabetic coronary disease, diffuse, aggressive, and progressive, and the ability of bypass surgery to protect against future events.
Significant left main disease with additional complexity. For patients with left main disease combined with additional complex coronary disease, bypass surgery has consistently shown favourable long-term outcomes in the major trials.
When the patient is a good surgical candidate. A relatively young, fit patient with good heart and lung function, no prior sternotomy, and high-complexity three-vessel disease: this is the patient for whom bypass surgery was designed.
When prolonged dual antiplatelet therapy is a concern. Stenting requires dual antiplatelet therapy (DAPT), typically aspirin combined with a second agent such as clopidogrel or ticagrelor, for a period after the procedure to prevent clot formation within the stent. For patients who cannot tolerate prolonged DAPT due to bleeding risk, a planned surgical procedure, or other medical reasons, bypass surgery avoids this requirement entirely. The internal mammary artery graft does not carry the same clotting risk as a freshly deployed stent, making CABG a more appropriate choice in these situations.
When stenting is the right answer
Percutaneous coronary intervention (PCI, or stenting) involves a cardiologist passing a thin, flexible catheter through an artery in the wrist or groin, navigating it to the blocked coronary artery under X-ray guidance, and deploying a small metal scaffold, the stent, to open the artery and hold it open. Modern drug-eluting stents release a medication that prevents the artery from narrowing again. For the right patient, stenting offers something bypass surgery cannot: a same-day or next-day procedure, performed under local anaesthetic and light sedation, with most patients home within 24 to 48 hours.
| Stenting (PCI) | Bypass surgery (CABG) | |
|---|---|---|
| How it works | Catheter through wrist or groin; stent opens blockage from inside | New routes around blockages using vessels from chest wall or leg |
| Anaesthetic | Local anaesthetic and light sedation | General anaesthetic |
| Hospital stay | 24-48 hours for most patients | 5-7 days typically |
| Recovery | Days to 1-2 weeks to normal activity | 6-12 weeks for full recovery |
| Best suited to | Low to intermediate complexity; single or double vessel disease; high surgical risk | High complexity; three-vessel disease; diabetes with multivessel disease; left main with complexity |
| Long-term durability | Excellent in suitable anatomy; repeat procedures more common in complex disease | Internal mammary artery graft patency exceeds 90% at 10 years |
| Repeat procedure risk | Higher in complex multivessel disease | Lower long-term repeat intervention rate in suitable patients |
| Antiplatelet therapy (DAPT) | Required for a period post-procedure; bleeding risk and compliance must be considered | No prolonged DAPT requirement; advantage in patients with bleeding concerns or planned surgery |
Low to intermediate SYNTAX score. The clearest indication for stenting over surgery is relatively straightforward coronary anatomy where the disease can be treated completely and safely. In this setting, the SYNTAX trial showed outcomes comparable to bypass at five and ten years.
Single and double vessel disease. For patients with significant disease in one or two coronary arteries, stenting is almost universally the preferred approach when intervention is needed.
High surgical risk. Where the EuroSCORE II indicates surgical risk outweighs the anatomical benefit of bypass, stenting, even of complex disease, may be the right answer.
When DAPT can be safely maintained. Stenting requires a period of dual antiplatelet therapy after the procedure. Where a patient can reliably tolerate this without bleeding concerns or planned surgery, this is not a barrier. For patients where DAPT compliance is straightforward, stenting remains an excellent option in appropriate anatomy.
Left main disease in lower complexity settings. The EXCEL and NOBLE trials concluded that stenting is a reasonable option for left main disease when the overall SYNTAX score is low to intermediate and the anatomy is suitable for complete revascularisation with stents.
The technology has moved on. The stents available today are not the stents of the SYNTAX trial era. Current-generation ultrathin drug-eluting stents, deployed by experienced operators, produce results that were simply not achievable when the original trial was designed. The evidence base continues to evolve, and the decisions your heart team makes for you are grounded in the best of what we know today.
Conclusion
The science exists to serve the patient in front of you. Not the patient in a trial, not the average across a population, but the person in the room, with their particular anatomy, their history, and their hopes about what comes next. No score has ever accounted for that. Your Heart Team has.
To the question patients most often ask me, which is better, stents or bypass, the honest answer is: it depends, and that is not an evasion. For straightforward disease, stenting is an excellent treatment with outstanding outcomes and a far shorter recovery. For complex, multivessel disease, particularly with diabetes or a high SYNTAX score, bypass surgery has proven itself over decades of follow-up data. Both treatments, done well in the right patient, extend life and relieve symptoms. The goal of everything described in this article is to help your team identify which of those patients you are.
Ask questions. Ask your cardiologist to explain your SYNTAX score and what it means for you specifically. Ask the cardiac surgeon what recovery would look like. An informed patient is always a better partner in their own care.
Patrick W. Serruys
Questions to ask your heart team:
- What is my SYNTAX score, and what does it mean for my specific situation?
- Has my case been discussed at a Heart Team meeting with a cardiac surgeon?
- Which treatment does the team recommend, and why?
- What are the risks of each option for me specifically, not in general, but for my anatomy and my health?
- If I choose stenting, will intracoronary imaging be used to guide the procedure?
- What happens if I need a repeat procedure in the future?
- How long do I have to make this decision, and who can I speak to if I have more questions?
There are no unreasonable questions when it comes to your heart. Your team expects them and welcomes them.

Key trials and research referenced in this article
- SYNTAX trial: Serruys PW et al. Percutaneous coronary intervention versus coronary-artery bypass grafting for severe coronary artery disease. New England Journal of Medicine, 2009
- SYNTAXES, 10-year follow-up: Thuijs D, Serruys PW et al. Percutaneous coronary intervention versus coronary artery bypass grafting in patients with three-vessel or left main coronary artery disease: 10-year follow-up. The Lancet, 2019
- 10 Years of SYNTAX, state of the art review: Serruys PW et al. Closing an Era of Clinical Research After Identifying New Outcome Determinants. JACC: Asia, 2023
- FREEDOM trial: Farkouh ME et al. Strategies for multivessel revascularization in patients with diabetes. New England Journal of Medicine, 2012
- EXCEL trial: Stone GW et al. Everolimus-eluting stents or bypass surgery for left main coronary artery disease. New England Journal of Medicine, 2016
- NOBLE trial: Makikallio T et al. Percutaneous coronary angioplasty versus coronary artery bypass grafting in treatment of unprotected left main stenosis. The Lancet, 2016
This article is intended for patient education only and does not constitute individual medical advice. Please discuss your specific circumstances with your treating cardiologist.