- Palpitations, the awareness of your own heartbeat, are one of the most common symptoms a cardiologist sees, and in the vast majority of cases the cause is benign.
- Common causes include ectopic beats sinus tachycardia from stress or caffeine, and anxiety all of which are manageable and rarely dangerous.
- Attributing palpitations to anxiety alone can be an oversimplification. A proper evaluation helps identify the true origin and offers meaningful reassurance.
- A small number of rhythm disorders do require treatment, including SVT atrial fibrillation and ventricular tachycardia which is why a clinical assessment is always worthwhile.
- Simple lifestyle adjustments, managing stress, moderating caffeine, improving sleep, make a substantial difference for most people with palpitations.
As a cardiologist, palpitations are one of the symptoms I encounter most often in the consulting room, and one of the most rewarding to assess. Patients arrive understandably anxious, convinced that something serious is happening with their heart. In the great majority of cases, a careful history, a physical examination, and a few straightforward tests provide clear answers, and with those answers comes genuine relief.
It is personally satisfying to offer that reassurance and to watch the tension leave someone’s face when they understand what their body has been doing and why. Palpitations can feel alarming, but they are rarely dangerous. The goal of this article is to help you understand what they are, what commonly causes them, and when it is worth seeking a closer look.
What Are Palpitations?
Palpitations are the conscious awareness of your own heartbeat, an experience most people never notice under normal circumstances. They may be described as a fluttering, pounding, racing, or thumping sensation in the chest, throat, or neck. Some people describe a feeling of the heart “skipping” or “missing” a beat, followed by a stronger thump. Others notice their heart suddenly beating very fast, or irregularly.
Palpitations can occur during activity or at rest, and many people notice them most acutely when lying down, particularly on their left side, when the heart is closer to the chest wall. They may come and go in seconds, or persist for minutes at a time. The pattern, duration, and associated symptoms all help guide the clinical assessment considerably.
What is important to understand from the outset is that the sensation of palpitations does not tell you, or your doctor, what is causing them. The same fluttering feeling can come from a completely benign extra heartbeat, from a period of sustained anxiety, or occasionally from a rhythm disorder that warrants attention. This is precisely why a proper evaluation matters, even when the cause turns out to be reassuring.
Attributing palpitations to anxiety alone can be dismissive and overly simplistic. While anxiety can certainly play a role, and can amplify underlying triggers, palpitations often have a distinct electrical or physiological origin that deserves evaluation in its own right.
The Most Common Causes
Ectopic Beats
The single most common cause of palpitations I see in practice is ectopic beats heartbeats that arise from an unexpected location in the heart’s electrical system, slightly out of sequence with the normal rhythm. They can originate in the upper chambers of the heart (atrial ectopics) or the lower chambers (ventricular ectopics), and both are extremely common in the general population.
The sensation people describe is typically a brief flutter or “missed beat”, what is actually happening is that the ectopic beat fires early, followed by a compensatory pause, and then the next normal beat arrives with more force than usual. It is that stronger beat after the pause that people feel most acutely. Ectopic beats are almost always benign in people with otherwise normal hearts, though they can be frequent and bothersome. They are covered in detail in our dedicated article on ventricular ectopic beats.
Sinus Tachycardia
Sinus tachycardia is simply a fast heart rate, defined as above 100 beats per minute, arising from the heart’s natural pacemaker, the sinus node. It is the normal response to exercise, emotional stress, fever, dehydration, or stimulants such as caffeine or nicotine. In this context it is entirely physiological, the heart is doing exactly what it is supposed to do. When it occurs at rest or in response to minimal exertion, it may reflect an underlying trigger worth addressing, such as anaemia, thyroid overactivity, or significant anxiety.
Stress, Anxiety, and the Adrenaline Effect
Stress and anxiety trigger a surge of adrenaline and other stress hormones that directly affect the heart, accelerating the rate, increasing the force of contraction, and heightening the body’s sensitivity to its own sensations. This can produce genuine palpitations, and it can also make existing ectopic beats feel far more prominent than they would otherwise. Many patients find themselves in a cycle: they notice a palpitation, become anxious about it, the anxiety produces more adrenaline, and the palpitations worsen. Understanding this cycle is itself part of breaking it.
Lifestyle Triggers
A number of everyday factors can precipitate or worsen palpitations in susceptible individuals. Caffeine is one of the most common, present in coffee, tea, energy drinks, and certain medications, it stimulates the heart and lowers the threshold for ectopic beats. Alcohol is another significant trigger, particularly in larger quantities or the morning after heavy consumption, a phenomenon sometimes called “holiday heart.” Nicotine poor sleep, dehydration, and significant dietary changes can all play a role. Hormonal fluctuations during menstruation, pregnancy, and particularly perimenopause, are a frequently underappreciated cause of palpitations in women.
Medical Conditions Worth Considering
A number of underlying medical conditions can manifest with palpitations and are worth ruling out as part of a thorough assessment. Thyroid overactivity (hyperthyroidism) is one of the most important, the thyroid gland has a profound influence on heart rate and rhythm, and an overactive thyroid can cause persistent sinus tachycardia and increase the risk of atrial fibrillation. Anaemia causes the heart to work harder to deliver adequate oxygen, often resulting in a faster, more noticeable heartbeat. Obstructive sleep apnoea a sleep disorder characterised by repeated pauses in breathing, is a commonly overlooked contributor, as the oxygen dips it causes can trigger ectopic beats and arrhythmias overnight. Electrolyte imbalances particularly low potassium or magnesium, can also destabilise heart rhythm.
Rhythm Disorders That Can Cause Palpitations
While most palpitations have a benign explanation, a cardiologist’s assessment also looks specifically for rhythm disorders, abnormalities in the heart’s electrical system that produce sustained or recurrent arrhythmias. These are less common than ectopic beats or sinus tachycardia, but they matter because some require treatment.
Supraventricular tachycardia (SVT) is a family of rapid heart rhythms originating above the ventricles, typically caused by abnormal electrical pathways or circuits within the heart. Episodes usually begin and end abruptly, patients often describe a sudden “switching on” of a very fast heartbeat, sometimes with lightheadedness or breathlessness. SVT is generally not dangerous but can be very symptomatic and is highly treatable.
Atrial fibrillation (AF) is the most common sustained cardiac arrhythmia, characterised by chaotic, rapid electrical activity in the atria producing an irregularly irregular heartbeat. Patients may describe a fluttering or quivering sensation, sometimes with breathlessness or fatigue. AF is important to identify because, unlike most other causes of palpitations, it carries a stroke risk that requires management.
Atrial flutter produces a rapid but more regular rhythm than AF, often with a characteristic pattern on the ECG. Ventricular tachycardia (VT) a fast rhythm arising from the lower chambers, is less common but more serious, and always warrants prompt evaluation when identified. The presence or absence of structural heart disease is a critical factor in determining the significance of any ventricular arrhythmia.
- The vast majority of palpitations seen in cardiology practice have a benign cause most commonly ectopic beats or sinus tachycardia.
- Ectopic beats in a structurally normal heart confirmed by echocardiogram, are almost never dangerous, even when frequent.
- Many people find that once they understand what is happening the palpitations become far less distressing and often less frequent.
- Lifestyle changes alone, reducing caffeine, improving sleep, managing stress, resolve symptoms for a significant proportion of patients.
How Palpitations Are Assessed
The starting point for any assessment of palpitations is a careful and unhurried history. I want to understand exactly what you are feeling, how you would describe the sensation, when it started, how long episodes last, whether they begin and end abruptly or fade gradually, what you were doing when they occurred, and whether anything reliably triggers or relieves them. Associated symptoms matter greatly: dizziness or lightheadedness during palpitations suggests the heart rate or rhythm is significantly affected; chest pain or breathlessness adds urgency; fainting is always taken seriously.
A physical examination includes listening to the heart for murmurs or rhythm irregularities, checking the pulse, and assessing blood pressure. From there, a small number of targeted investigations are arranged.
An ECG (electrocardiogram) is always the first test, a quick, painless recording of the heart’s electrical activity that can identify structural patterns, pre-excitation syndromes, and any rhythm abnormality present at the time of recording. Blood tests check thyroid function, a full blood count for anaemia, and electrolytes. An echocardiogram an ultrasound of the heart, assesses structure and function, which is an important determinant of how significant any rhythm findings might be.
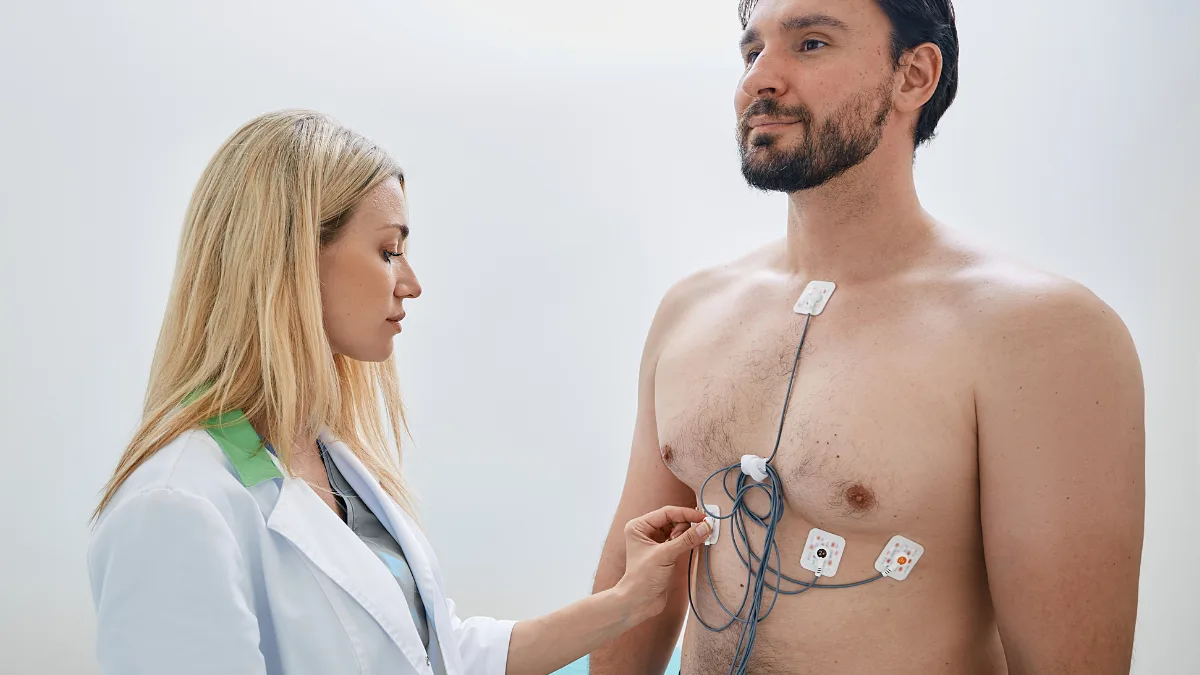
Because palpitations are often intermittent, the most valuable test is frequently a Holter monitor a small, wearable ECG device worn continuously for 24 to 48 hours that records every heartbeat during the monitoring period. If you experience palpitations while wearing it, the recording captures exactly what the heart was doing in that moment. For less frequent episodes, extended monitors worn over weeks or even months are available, including implantable loop recorders that sit just beneath the skin and can monitor continuously for up to three years. This is often the investigation that provides the clearest answer, and in many cases, that answer is genuinely reassuring.
| Investigation | What It Assesses | When It’s Most Useful |
|---|---|---|
| ECG | Heart rhythm, electrical conduction, WPW pattern | First-line for all palpitations |
| Blood tests | Thyroid function, anaemia, electrolytes | Identifying systemic triggers |
| Holter monitor | Continuous rhythm recording over 24–48 hours | Intermittent or frequent palpitations |
| Echocardiogram | Heart structure and function | Assessing significance of any arrhythmia found |
| Extended event monitor | Rhythm recording over weeks to months | Infrequent episodes not captured on Holter |
| Implantable loop recorder | Continuous monitoring for up to 3 years | Very infrequent episodes or unexplained symptoms |
| Exercise stress test | Rhythm behaviour during exertion | Palpitations triggered by exercise |
- How it feels: Fluttering, racing, thumping, skipping, irregular, be as specific as you can about the sensation.
- When it happens: At rest, during exercise, after meals, at night, or first thing in the morning.
- How long it lasts: Seconds, minutes, or longer, and whether it stops suddenly or fades gradually.
- How it starts and stops: Does it switch on and off abruptly, or come and go gradually? Abrupt onset and offset is a key feature of SVT.
- What comes with it: Dizziness, chest discomfort, breathlessness, or near-fainting during episodes are all important to mention.
- Your triggers: Coffee, alcohol, stress, poor sleep, exercise, anything you have noticed that reliably brings them on.
- How often: Daily, weekly, or occasional, and whether frequency has changed recently.
Managing Palpitations, Lifestyle First
For the majority of people whose palpitations have a benign cause, lifestyle adjustments make a meaningful and sometimes dramatic difference. This is not a consolation prize, it is genuinely effective management that addresses the underlying triggers rather than simply suppressing symptoms.
Caffeine is worth reviewing first. Many people are surprised by how much their palpitations improve when they reduce coffee, energy drinks, or strong tea, particularly if consumption has crept up over time. A gradual reduction is more comfortable than stopping abruptly. Alcohol is similarly worth moderating, even if you do not directly connect it to your symptoms, a period of reduction is a useful diagnostic trial in its own right. Sleep has a profound effect on heart rhythm; poor or fragmented sleep raises sympathetic nervous system activity and lowers the threshold for ectopic beats. Addressing sleep apnoea if it is suspected is particularly important.
Stress management deserves genuine attention rather than a passing mention. Regular exercise, mindfulness practice, and simply understanding what is happening physiologically during a palpitation episode, that it is not dangerous, that it will pass, can break the anxiety-adrenaline cycle that perpetuates symptoms for many people. Hydration and a balanced diet with adequate magnesium and potassium support normal electrical stability in the heart muscle. Under medical guidance, magnesium supplementation is sometimes helpful for people with frequent ectopic beats.
When Medication or Procedures Are Considered
Most people with palpitations do not need medication. For those who do, typically because a specific rhythm disorder has been identified, or because symptoms are significantly affecting quality of life, treatment is tailored to the underlying cause.
Beta blockers are the most commonly used medication for symptomatic palpitations. They work by blunting the effect of adrenaline on the heart, reducing heart rate and dampening the intensity of ectopic beats. They are well tolerated by most people and are a reasonable first step when lifestyle measures alone are insufficient. Calcium channel blockers such as verapamil or diltiazem serve a similar rate-controlling function and are sometimes preferred depending on the individual’s profile.
For specific rhythm disorders, more targeted treatment may be appropriate. SVT, atrial flutter, and some forms of AF are highly amenable to catheter ablation a minimally invasive procedure that identifies and eliminates the abnormal electrical pathway or trigger responsible for the arrhythmia. In experienced hands, ablation offers excellent long-term outcomes and can be curative for many patients with SVT. AF management involves a broader conversation about rhythm control, rate control, and anticoagulation that deserves its own dedicated article.
Heart Matters Resource
When in Doubt, Get Checked Out
If your palpitations are new, changing in character, or accompanied by any symptom that concerns you, please do not hesitate to get checked. Heart Matters has a dedicated resource covering the symptoms that should never be ignored and why seeking help is always the right call.
Conclusion
Palpitations are one of the most common symptoms in cardiology, and one of the most treatable. The vast majority of people who come to see me leave with a clear explanation and genuine reassurance. In most cases the cause is benign, the triggers are identifiable, and simple lifestyle adjustments make a real difference.
What matters is not suffering in silence or assuming the worst, but getting a proper assessment so you know exactly what you are dealing with. For most people, that assessment is the most therapeutic thing of all. Understanding what your heart is doing, and why, takes away the fear, and with the fear gone, the palpitations themselves often become far easier to live with or disappear entirely.
If your symptoms are new, persistent, or accompanied by anything that concerns you, please do speak with your doctor. You are not wasting anyone’s time, this is exactly what we are here for.
More from Heart Matters
- Ventricular Ectopic Beats: What They Are and What They Mean
- The Electrocardiogram (ECG): What It Shows and Why It Matters
- Understanding the Holter Monitor Test
- Cardiac Monitoring Devices: From Holter Monitors to Loop Recorders
- Watch: Implantable Loop Recorders Explained, Heart Matters YouTube
- Chest Pain: Causes, Symptoms, and When to Seek Help
- When in Doubt, Get Checked Out, Heart Matters Resource










