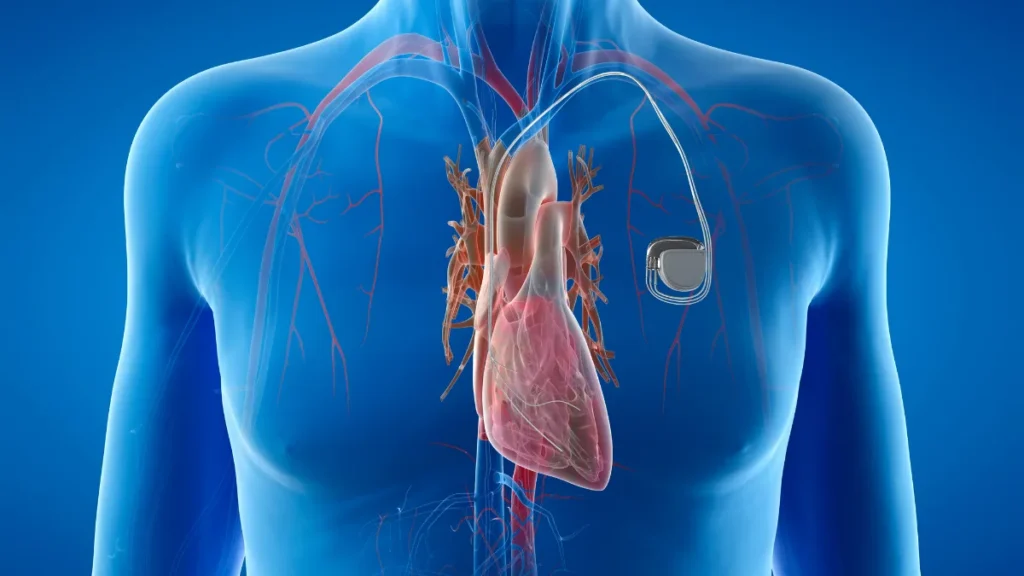
- A pacemaker is a small implantable device that monitors the heart’s rhythm and delivers electrical impulses when the heart rate falls below a set threshold, ensuring a reliable, safe minimum rate.
- Pacemakers are used primarily to treat symptomatic bradycardia caused by sinus node dysfunction or heart block.
- There are several types, single-chamber, dual-chamber, biventricular (CRT), and the newer leadless pacemaker, each suited to different clinical situations.
- Implantation is minimally invasive, performed under local anaesthesia and sedation, with most patients home the following day.
- Battery life typically lasts 8 to 15 years. Generator replacement is a straightforward procedure, the leads are usually kept.
- Life with a pacemaker is largely normal. Most activities, including exercise, travel, and everyday appliances, are safe with simple precautions.
Being told you need a pacemaker can feel significant, and understandably so. Having a device implanted in the chest, connected to the heart, is not a small thing conceptually.
But in practice, pacemaker implantation is one of the most reliable and well-established procedures in cardiology. For those who need one, it typically produces a dramatic improvement in quality of life, often almost immediately.
Fatigue, dizziness, breathlessness, and fainting, the symptoms of a heart beating too slowly, frequently resolve within days of implantation. Many patients tell us they didn’t realise just how much their slow heart rate had been affecting them until they felt better. That response, more than anything, reflects how much difference the right treatment makes.
How a Pacemaker Works
The two main components
A pacemaker has a pulse generator a small sealed metal case containing the battery and circuitry, implanted under the skin just below the collarbone. Leads are thin insulated wires threaded through a vein into the heart, anchored at their tips against the inner surface of one or more heart chambers.
The device continuously monitors the heart’s electrical activity. If the heart beats normally above the programmed minimum rate, the pacemaker does nothing, it simply observes. If the rate drops below the threshold or a pause is detected, it delivers a precisely timed electrical impulse to stimulate the heart to beat.
This happens in milliseconds, is entirely painless, and most people cannot feel it occurring.
Smart technology
Modern pacemakers are sophisticated devices. Rate response programming adjusts the pacing rate in response to physical activity. Remote monitoring allows the device’s performance and stored heart rhythm data to be reviewed by the clinical team without the patient attending hospital, any concerns are flagged automatically.
Types of Pacemaker
The right type depends on the underlying condition and the individual patient’s needs.
Single-chamber
One lead, placed in the right ventricle or right atrium. Used where pacing in only one chamber is needed, such as AF with a slow ventricular response.
Dual-chamber
Two leads, right atrium and right ventricle. Coordinates timing between chambers, mimicking the heart’s natural sequence. Preferred for most patients with complete heart block or sinus node dysfunction.
Biventricular (CRT)
Three leads, paces both ventricles simultaneously. Designed for heart failure patients with electrical dyssynchrony. Resynchronises contraction and improves pumping function.
Leadless pacemaker
No generator pocket, no leads. A miniaturised device implanted directly into the right ventricle via catheter. Eliminates lead-related complications. Increasingly used for appropriate patients.
The Implantation Procedure
What to expect
Conventional pacemaker implantation is performed under local anaesthesia and sedation, you will be comfortable and relaxed but not under general anaesthesia. The procedure typically takes 60 to 90 minutes.
A small incision is made just below the collarbone, a vein is accessed, and the leads are threaded under X-ray guidance into the correct heart chambers and tested. The pulse generator is connected and placed in a small pocket under the skin. The incision is closed with dissolvable sutures.
Recovery
Most patients stay in hospital overnight and go home the following day. The arm on the side of the implant is rested for a few weeks to allow the lead tips to embed securely.
A follow-up wound check and device interrogation are arranged within a few weeks. After that, routine pacemaker checks, typically every 6 to 12 months, continue for the life of the device.
Battery Life and Generator Replacement
Pacemaker batteries typically last between 8 and 15 years, depending on device type and how much pacing is actually required. When the battery nears end of life, the entire generator is replaced, the leads are left in place and reconnected through the same pocket. Most patients go home the same day or the following morning.
Battery status is monitored at every follow-up appointment and tracked continuously via remote monitoring where available. There is no sudden cliff edge, replacement is planned well in advance.
Living With a Pacemaker
Daily life
Life with a pacemaker is, for the vast majority of people, essentially normal. The device is not felt, does not restrict movement, and has no visible external presence under clothing.
Exercise is encouraged and safe, the pacemaker adjusts its pacing rate in response to activity. Driving restrictions apply for a period after implantation, varying by country and clinical situation, your team will advise specifically. Flying is safe and airport security will not affect pacemaker function, though the device will be detected by metal detectors. Always carry your device identification card.
Electrical appliances and MRI
Everyday household appliances, including microwaves and most domestic devices, are safe. Maintaining a distance of around 60cm from induction hobs while in use is a simple precaution. Strong industrial electromagnetic fields should be avoided.
Most pacemakers implanted in the past decade are MRI-conditional, meaning MRI is possible with appropriate precautions. Always inform the radiology team of your pacemaker before any MRI, and confirm with your device clinic in advance.
- Carry your pacemaker identification card at all times, it lists your device details and device clinic contact information.
- Attend your regular device checks, these monitor battery life, lead function, and stored heart rhythm data.
- Inform every doctor, dentist, or healthcare professional you see that you have a pacemaker, particularly before any surgical or procedural intervention.
- MRI is often possible, but always confirm with your device clinic and inform the radiology team in advance.
- Report any return of your original symptoms, dizziness, breathlessness, or fainting, to your device clinic promptly.
Heart Matters Resource
When in Doubt, Get Checked Out
If you have a pacemaker and your original symptoms return, or if you experience any new symptoms you’re uncertain about, contact your device clinic or seek assessment. Your device stores data that can help answer questions quickly.
Conclusion
For those who need one, a pacemaker is one of the most reliably effective interventions in cardiology. The technology is mature, the procedure is well-established, and the improvement in symptoms is typically substantial and immediate.
The prospect of having a device implanted is understandably daunting before it happens. After it does, most patients wonder why they waited so long.
Understanding your device, attending your follow-up appointments, and knowing what to watch for are your responsibilities in the partnership. The device does the rest.