Key Points
- Mitral valve prolapse (MVP) is one of the most common valve findings, affecting around 2–3% of the population, and is usually picked up as an incidental finding during a routine check-up.
- For the vast majority of people, MVP is a benign condition that does not require treatment and does not shorten life expectancy.
- An echocardiogram (heart ultrasound) confirms the diagnosis and helps assess whether any blood is leaking backward through the valve.
- Regular monitoring is the mainstay of management, most people with MVP never need surgery or procedures.
- If you experience new symptoms such as palpitations, breathlessness, or dizziness, it is always worth mentioning these to your doctor.
Being told you have a heart murmur, or that your valve is “a bit floppy”, can feel alarming. But if the diagnosis is mitral valve prolapse, the reassurance you are likely to receive from your doctor is genuine, not just consoling. For the overwhelming majority of people, this is a condition you will live with, not be limited by.
Mitral valve prolapse is one of the most common valve findings in cardiology. It is often discovered during a routine examination, long before any symptoms appear, if they ever do. This article explains what MVP is, why it happens, and what it means for your daily life and long-term health.
What is the mitral valve?
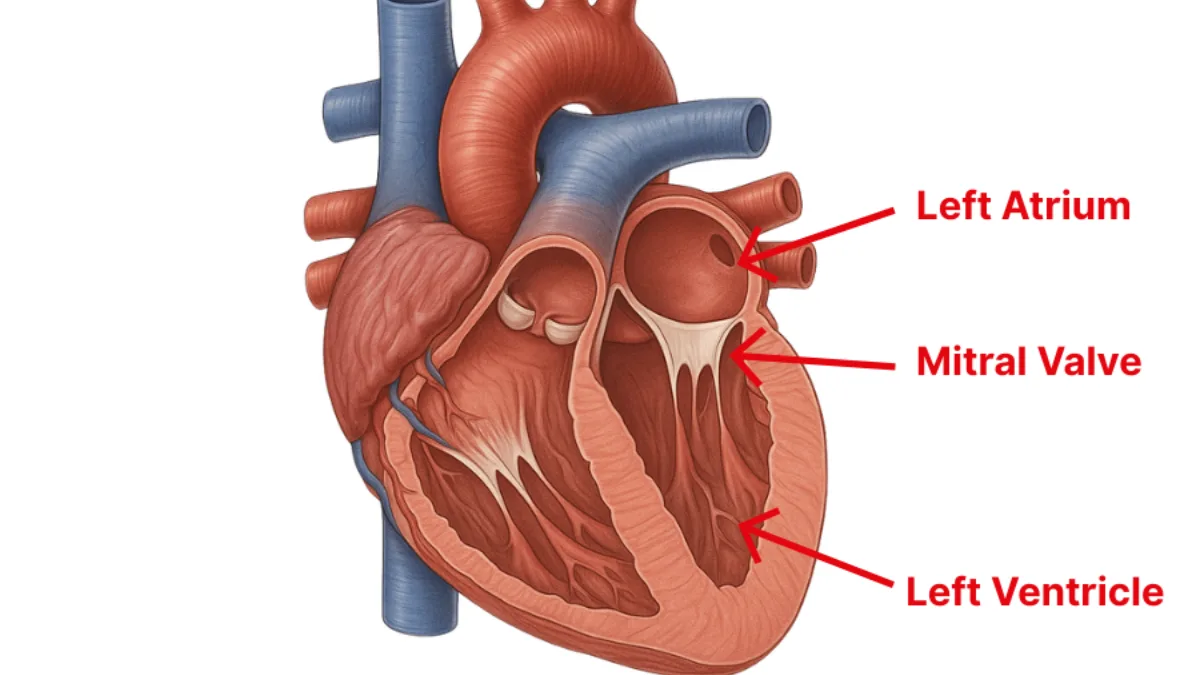
The mitral valve sits between two chambers on the left side of your heart, the left atrium above and the left ventricle below. Its job is straightforward: let blood flow in one direction and prevent it from leaking back. It does this with two thin, flexible flaps called leaflets, which open and close with every heartbeat.
In mitral valve prolapse, these leaflets are slightly too large or too floppy. Instead of closing flat and flush, they bow back toward the left atrium when the heart squeezes. Think of a door that doesn’t quite sit flat in its frame, it still closes, but with a slight bulge. In most cases, the seal is perfectly adequate and no blood leaks through.
What causes MVP?
The most common reason is simply how the valve was built. In many people, MVP is inherited, it tends to run in families and is usually related to subtle variations in the connective tissue that makes up the valve leaflets. This is not a defect in any serious sense; it is more of a structural variation that most people carry without ever knowing.
A small number of people develop MVP in the context of connective tissue conditions such as Marfan syndrome or Ehlers-Danlos syndrome, where the body’s collagen is more elastic than usual. In these cases, the valve tissue can be more mobile and more prone to leaking, and closer monitoring is typically recommended.
Occasionally, MVP can develop as a consequence of other conditions, rheumatic fever (now rare in countries with good antibiotic access), age-related changes to the valve, or other heart conditions that alter the shape of the left ventricle and place different mechanical stresses on the valve apparatus.
How common is it?
people has mitral valve prolapse, making it one of the most common heart valve findings
In my practice, MVP is probably one of the most frequently asked-about diagnoses, precisely because it sounds more dramatic than it usually is. It tends to be slightly more common in women and is often picked up in adolescence or early adulthood, though it can be found at any age.
Most of my patients with MVP are surprised to discover they have it, and even more surprised to hear that a check-up every few years is usually all they need.
What symptoms might I notice?
Many people with MVP have no symptoms whatsoever. The condition is discovered during a routine check, a doctor hears a faint clicking sound through a stethoscope, and the echocardiogram confirms the finding.
When symptoms do occur, they are usually mild and manageable:
| Symptom | What it may feel like |
|---|---|
| Palpitations | A fluttering, skipping, or racing sensation in the chest |
| Fatigue | Feeling more tired than expected after activity |
| Mild breathlessness | Especially with exertion; rarely at rest |
| Light-headedness | Particularly when standing up quickly |
| Chest awareness | A vague awareness of the heartbeat, not pain |
It is worth knowing that these symptoms are not always directly caused by the valve itself. Changes in the autonomic nervous system, the part that regulates heart rate and blood pressure automatically, may play a role in some people with MVP. This is another reason why symptoms rarely signal anything serious.
How is MVP diagnosed?
Your doctor may first notice a soft clicking sound when listening to your heart with a stethoscope. This distinctive sound is caused by the valve leaflets snapping back during the heartbeat, it is not harmful, but it is a useful clue that prompts further investigation.
The diagnosis is confirmed with an echocardiogram, a painless ultrasound that shows the heart in real time. The echocardiogram tells us not just whether the valve is prolapsing, but also whether any blood is leaking backward (mitral regurgitation) and, if so, how much. This assessment is the key factor in deciding how closely the condition needs to be followed.
Occasionally, a Holter monitor may be arranged if palpitations are frequent, to check whether any heart rhythm changes are present.
Can MVP cause complications?
For most people, it does not. But it is worth knowing what can occasionally arise, so you have a clear picture:
Mitral regurgitation
The most common complication is the valve becoming slightly leaky, allowing a small amount of blood to flow backward into the atrium when the heart contracts. Mild leakage is common and often remains stable for many years without causing any problems. Significant leakage is much less common, and your cardiologist will monitor for this with periodic echocardiograms.
Heart rhythm changes
Palpitations are the most frequently reported symptom in MVP. In the majority of cases these are benign extra heartbeats, uncomfortable but not dangerous. Occasionally, MVP is associated with atrial fibrillation, an irregular heart rhythm that may require treatment.
Infective endocarditis
People with significant prolapse or regurgitation have a slightly increased susceptibility to valve infection. Good oral hygiene and prompt treatment of skin infections are the best forms of prevention. Routine antibiotics before dental work are no longer recommended for most people with MVP, but always check with your own cardiologist, as the advice depends on your individual situation.
Rarely, significant valve dysfunction
In a small number of people, worsening mitral regurgitation over time may eventually require intervention. Modern valve repair techniques, including minimally invasive options, have excellent outcomes, and surgery is only recommended when the heart shows early signs of strain from carrying extra volume.
How is MVP managed?
| Situation | Typical approach |
|---|---|
| No symptoms, mild or no leakage | Observation only, echocardiogram every 3–5 years |
| Palpitations or mild symptoms | Lifestyle adjustments; occasionally beta-blockers |
| Moderate leakage, no symptoms | More frequent monitoring, typically every 1–2 years |
| Significant leakage with heart strain | Valve repair or replacement considered |
For most people, management is simply a matter of keeping up with scheduled check-ups. Staying active, avoiding excessive caffeine and alcohol if these trigger palpitations, and maintaining good general heart health are all beneficial. There is no diet or lifestyle restriction that applies specifically to MVP in most cases.
Living well with MVP
The most important thing to understand about this diagnosis is that most people with MVP live completely unrestricted lives. They exercise, travel, have families, and grow old without their valve ever becoming a significant clinical issue. The monitoring we do over time is not because we expect things to change, it is because we want to be certain they have not.
If you notice new symptoms, particularly worsening breathlessness, a more pronounced awareness of your heart, or episodes of irregular rhythm, bring these to your doctor’s attention. Not because they are likely to be serious, but because they are worth knowing about and easy to assess.
With the right follow-up and a focus on general wellbeing, MVP is a condition that sits quietly in the background of a full and active life.
Questions to Ask Your Cardiologist
Going to your appointment with a few questions prepared makes a real difference. Here are some worth raising if you have been told you have MVP:
Questions worth asking
- Is my MVP mild, moderate, or significant, and what does that mean for how often I need monitoring?
- Is there any leakage through the valve, and has it changed since my last echocardiogram?
- Are there any activities or sports I should avoid, or am I fine to stay as active as I like?
- Do I need to take any precautions before dental work or surgery?
- What symptoms should prompt me to get in touch before my next scheduled review?
Conclusion
Mitral valve prolapse is a common finding, far more common than most people realise, and for the vast majority of those who have it, it remains a background observation rather than a medical problem. The echocardiogram is the cornerstone of assessment, giving your cardiologist a clear picture of how the valve is behaving and whether any monitoring adjustments are needed.
If you have been told you have MVP, the message from your cardiologist is likely to be one of reassurance. That reassurance is well founded in the evidence, and in the experience of the many patients we see who carry this diagnosis comfortably for decades.
If you have questions about your own situation, bring them to your next appointment. A short conversation with your doctor can do a great deal to put your mind at ease, and that is always a worthwhile use of your time together.
Free Resources
Our Heart Glossary explains terms like mitral regurgitation, echocardiogram, and atrial fibrillation in plain language, useful to have open before your next cardiology appointment.