Key Points
- After a stent procedure or a heart attack, you will be prescribed antiplatelet medication. Understanding why you need it is one of the most important things you can do for your recovery.
- Antiplatelet agents reduce the stickiness of platelets, the small cells in your blood that form clots, protecting you during a critical period of healing.
- The duration and choice of antiplatelet therapy is entirely individualised. Only your cardiologist, who knows your specific procedure, your coronary anatomy, and your overall clinical picture, can advise you on what is right for you.
- Never stop antiplatelet medication without speaking to your cardiologist first. Stopping suddenly can be dangerous.
If you have recently had a stent placed in one of your coronary arteries, or if you have been admitted to hospital with a heart attack, your cardiologist will have prescribed antiplatelet medication as part of your treatment.
You may be taking this medication faithfully without fully understanding what it does or why it matters so much. Others stop taking it too soon because they feel well, or because they are concerned about side effects.
Understanding the rationale behind antiplatelet therapy, why your heart needs this protection and what happens if it is withdrawn, is one of the most important things you can do for your recovery and your long-term heart health.
What are antiplatelet agents?
Platelets are tiny cells that circulate in your blood. Their job is to respond to injury by clumping together to form a clot and seal a wound. This is an essential and life-saving function in the right circumstances.
In the context of coronary artery disease, however, platelet clumping in the wrong place at the wrong time can be dangerous. Antiplatelet agents work by reducing the stickiness of platelets, making them less likely to clump together and form a clot inside your coronary arteries.
These medications are sometimes referred to informally as blood thinners, though strictly speaking they are not the same as anticoagulants, which work differently. The more precise term is antiplatelet therapy, and that is what your cardiologist will use when discussing your treatment.
What happens inside your artery during a heart attack?
Your blood vessels
Blood cells circulate through your coronary arteries, carrying oxygen to the heart muscle.
Plaque rupture
When a fatty plaque on the artery wall cracks, it triggers an immediate platelet response that can form a dangerous clot.
The stent
A metal mesh scaffold holds the artery open after a blockage is cleared. Antiplatelet therapy protects it during the critical healing period.
To understand why antiplatelet therapy matters, it helps to understand what actually happens inside a coronary artery during a heart attack. The sequence below shows how a healthy artery becomes blocked.
How a heart attack happens
The journey from healthy artery to restricted flow
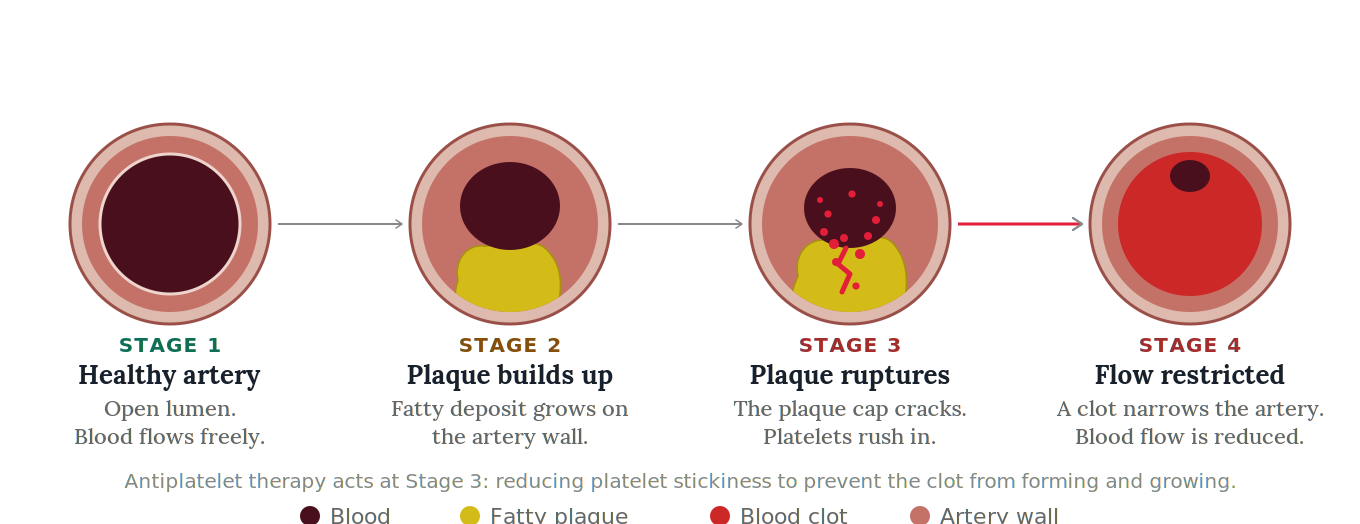
Plaque is made up of fat, cholesterol, calcium, and other substances that build up inside the artery wall over many years. This process is known as atherosclerosis. It grows as a deposit on the wall itself, gradually protruding inward and narrowing the channel through which blood flows.
When a plaque ruptures, the body treats it like any other wound and sends platelets rushing to the site to form a clot. In the coronary arteries, this response can be catastrophic: the clot can grow large enough to cut off blood flow to the heart entirely.
This is precisely the moment where antiplatelet therapy becomes critical. By reducing the stickiness of platelets, these medications can slow or prevent the runaway clotting that leads to a full blockage.
Why do you need antiplatelet therapy after a stent?
When a stent is placed inside a coronary artery, it is a small metal scaffold that holds the artery open where it has been narrowed by a blockage. The stent becomes a permanent part of your artery, but in the weeks and months after the procedure, your body needs time to heal the vessel wall around it.
During this healing period, the surface of the stent can attract platelets. If platelets accumulate and a clot forms inside the stent, it can block the artery at precisely the point where it was just opened. This is called stent thrombosis, meaning a dangerous blood clot forming inside the very device that was placed to keep the artery open. It is a serious event, and antiplatelet therapy dramatically reduces this risk by keeping platelets from clustering on the stent surface while the healing process completes.
Why do you need antiplatelet therapy after a heart attack?
After a heart attack, even when the artery has been opened and a stent placed, the underlying coronary artery disease remains. The plaque that caused the event has been stabilised but not eliminated, and the arteries are in an inflammatory state that makes further events more likely in the weeks and months that follow.
Antiplatelet therapy during this period provides critical protection against a further clot forming, either in the treated artery or elsewhere in the heart’s circulation.
The period immediately after a heart attack is when your risk of a further event is at its highest. Antiplatelet therapy during this time is one of the most evidence-based and effective treatments available.
One of the things I emphasise most strongly to my patients is the importance of understanding why they are taking antiplatelet therapy. When you understand that these medications are protecting you during a genuinely vulnerable period of healing, you are far more likely to take them consistently. And consistent treatment saves lives.
What does dual antiplatelet therapy mean?
Many people after a stent or a heart attack are prescribed two antiplatelet medications together. This combination is called dual antiplatelet therapy, or DAPT.
The two medications work through different mechanisms, and together they provide more complete platelet protection than either alone during the period when it matters most.
Your cardiologist will determine which medications are most appropriate for you, and for how long you need to take both. This decision is based on the complexity of your procedure, your coronary anatomy, your other medical conditions, and many factors that are unique to you.
The antiplatelet medications you may be prescribed
There are several antiplatelet medications used in cardiology. They are known by different names in different countries, which can cause confusion when you read about them online or travel abroad.
Aspirin
Also known as
Disprin
Cartia
Cardiprin
Ecotrin
Angettes
Aspro
Astrix
The oldest and most widely used antiplatelet agent. Most people continue a low-dose aspirin long term after a stent or heart attack.
Clopidogrel
Also known as
Iscover
Clopilet
Ceruvin
Antiplaq
Clopivas
A stronger antiplatelet agent commonly prescribed alongside aspirin as part of dual antiplatelet therapy after a stent or heart attack. Read more in our article on what clopidogrel is used for.
Ticagrelor
Also known as
Brilique
Possia
A newer and more potent antiplatelet agent that works more rapidly than clopidogrel. Commonly prescribed for people at higher risk as part of dual antiplatelet therapy. Read more in our article on ticagrelor (Brilinta).
Your cardiologist will choose the most appropriate agent based on your clinical situation, your other medications, and your individual risk profile. Do not switch between these medications or adjust your dose without discussing it with your clinical team first.
An important note
The duration and choice of antiplatelet therapy is one of the most individualised decisions in cardiology. It depends on the complexity of your procedure, your coronary anatomy, your other medical conditions, and many other factors that only your cardiologist fully understands. No article, however well informed, can tell you what the right treatment is for you. That conversation belongs with your clinical team.
The most important thing you can do
Take your antiplatelet medication exactly as prescribed, and do not stop it without speaking to your cardiologist first.
Stopping antiplatelet therapy early, even for a short period, can dramatically increase the risk of a clot forming in your stent or a further cardiac event. Even if you feel completely well, your medication is still doing important work that you cannot feel.
If you are due to have surgery, a dental procedure, or any other invasive treatment, always tell the treating team that you are on antiplatelet therapy before anything is done. Your cardiologist should be involved in any decision about temporarily adjusting your medication around a procedure.
Questions to ask your cardiologist
Understanding your antiplatelet therapy is entirely reasonable, and your cardiologist should welcome the conversation. Here are some questions worth raising at your next appointment.
Why am I on this medication?
Understanding the specific reason for your antiplatelet therapy helps you understand what it is protecting against and why it matters for your individual situation.
What should I do before a procedure?
If you need surgery, dental work, or any invasive treatment, ask your cardiologist how to manage your antiplatelet therapy around it. Never stop it based on advice from another clinician without checking first.
What are the signs I should watch for?
Ask what symptoms would warrant an urgent call or visit, and what you can manage with a routine appointment. Being prepared gives you confidence.
When will my treatment be reviewed?
Ask when your cardiologist plans to review your antiplatelet therapy and what factors will guide any change. Understanding the plan helps you stay engaged in your own care.
Conclusion
Antiplatelet therapy after a stent or a heart attack is not optional, and it is not indefinite. It is a carefully considered treatment designed to protect you during a period when your heart is most vulnerable.
The most powerful thing you can do is understand why it matters, take it consistently, and have an open conversation with your cardiologist about any concerns.
Your cardiologist has considered your specific situation in detail when prescribing your antiplatelet therapy. Trust that plan, follow it carefully, and ask questions whenever you are uncertain. Understanding your wider cardiovascular risk factors is also an important part of your long-term heart health.
References
- Valgimigli M, Bueno H, Byrne RA, et al. 2017 ESC focused update on dual antiplatelet therapy in coronary artery disease. European Heart Journal 2018;39:213-260
- Mehran R, Baber U, Sharma SK, et al. Ticagrelor with or without Aspirin in High-Risk Patients after PCI. New England Journal of Medicine 2019;381:2032-2042
- Urban P, Mehran R, Colleran R, et al. Defining High Bleeding Risk in Patients Undergoing Percutaneous Coronary Intervention. Circulation 2019;140:240-261
- Goel R, Spirito A, Cao D, Sartori S, Dangas GD, Mehran R, et al. Procedural Complexity and Bleeding Risk in Patients Undergoing Percutaneous Coronary Intervention. American Journal of Cardiology 2026;263:43-52
More from Heart Matters
- Heart Stent Unboxing: What’s Inside the Tiny Device That Keeps Arteries Open
- Stents or Bypass Surgery: How Your Heart Team Decides
- Recovering After a Heart Attack
- What Is Clopidogrel Used For?
- Ticagrelor (Brilinta): Understanding Your Heart Medication
- Aspirin and Heart Health: What the Latest Evidence Shows
- What Is Atherosclerosis?